Clinical outcome of intradural extramedullary spinal cord tumors: A single-center retrospective analytical study
- PMID: 33948315
- PMCID: PMC8088529
- DOI: 10.25259/SNI_839_2020
Clinical outcome of intradural extramedullary spinal cord tumors: A single-center retrospective analytical study
Abstract
Background: Intradural extramedullary spinal cord tumors (IESCT) account for approximately two-thirds of largely benign intraspinal neoplasms. They occasionally present with acute neurological deterioration warranting emergent surgical intervention.
Methods: Here, we reviewed a series of 31 patients with intradural extramedullary spinal tumors who underwent surgery from 2012 to 2019. Patients averaged 50.8 years of age, and there were 16 males and 15 females. Patients were followed for a minimum of 1 year. Multiple clinical outcome variables were studied (e.g., Karnofsky Performance Score [KPS], visual analog scale (VAS), and Frankel grade).
Results: The majority of IESCT tumors were found in the thoracic spine 18 (58.06%) followed by the lumbar 8 (25.80%), cervical 1 (3.22%), and combined junctional tumors 4 (12.90%) (cervicothoracic-02 and thoracolumbar-02). Histopathological diagnoses included schwannomas-16 (51.61%), meningiomas-11 (35.48%), lipomas-2 (6.45%), hemangiomas-1 (3.22), and ependymomas-01 (03.22%). The VAS score was reduced in all cases, while KPS and Frankel grades were significantly improved. Complications included cerebrospinal fluid leakage, new/residual paresthesias, and tumor recurrence (12.50%).
Conclusion: Most intradural extramedullary tumors are benign and are readily diagnosed utilizing MRI scans. Notably, good functional outcomes follow surgical intervention.
Keywords: Clinical outcome; Intradural extramedullary tumors; Spinal tumors; Surgical excision.
Copyright: © 2021 Surgical Neurology International.
Conflict of interest statement
There are no conflicts of interest.
Figures
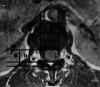
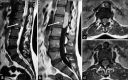
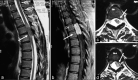
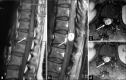
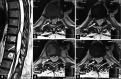
Similar articles
-
Functional outcomes in intradural extramedullary spinal tumors.Surg Neurol Int. 2024 Apr 5;15:114. doi: 10.25259/SNI_689_2023. eCollection 2024. Surg Neurol Int. 2024. PMID: 38742010 Free PMC article.
-
Clinicopathological Study of Intradural Extramedullary Spinal Tumors and Its Correlation With Functional Outcome.Cureus. 2021 Jun 18;13(6):e15733. doi: 10.7759/cureus.15733. eCollection 2021 Jun. Cureus. 2021. PMID: 34285844 Free PMC article.
-
Modified paramedian transpedicular approach and spinal reconstruction for intradural tumors of the cervical and cervicothoracic spine: clinical experience.Spine (Phila Pa 1976). 2007 Mar 15;32(6):E203-10. doi: 10.1097/01.brs.0000257567.91176.76. Spine (Phila Pa 1976). 2007. PMID: 17413461
-
Multifocal intradural extramedullary ependymoma. Case report.J Neurosurg Spine. 2011 Jan;14(1):65-70. doi: 10.3171/2010.9.SPINE09963. Epub 2010 Dec 10. J Neurosurg Spine. 2011. PMID: 21142461 Review.
-
Minimally invasive removal of thoracic and lumbar spinal tumors using a nonexpandable tubular retractor.J Neurosurg Spine. 2013 Dec;19(6):708-15. doi: 10.3171/2013.9.SPINE121061. Epub 2013 Oct 18. J Neurosurg Spine. 2013. PMID: 24138063 Review.
Cited by
-
Intradural extra-medullary spinal cord tumor after dorso-lumbar spine fixation following 12th dorsal vertebra burst fracture: A case report with literature review.Radiol Case Rep. 2024 Dec 18;20(3):1393-1397. doi: 10.1016/j.radcr.2024.11.080. eCollection 2025 Mar. Radiol Case Rep. 2024. PMID: 39801524 Free PMC article.
-
The lamina-spinous process-ligament complex implantation for the spinal stability: A case report and review of literature.Medicine (Baltimore). 2025 Apr 4;104(14):e42044. doi: 10.1097/MD.0000000000042044. Medicine (Baltimore). 2025. PMID: 40193667 Free PMC article. Review.
-
Surgical and clinical outcomes of ventral versus dorsal/lateral intradural extramedullary schwannomas: a retrospective comparative study.Spinal Cord. 2025 Aug;63(8):410-417. doi: 10.1038/s41393-025-01105-w. Epub 2025 Jul 9. Spinal Cord. 2025. PMID: 40628951
-
Factors Determining Rehabilitation Needs After Intradural Spinal Tumor Surgery: A Prospective Study.Brain Sci. 2025 Jan 8;15(1):51. doi: 10.3390/brainsci15010051. Brain Sci. 2025. PMID: 39851419 Free PMC article.
-
Spinal Cord Tumors: A Review of Demographic Characteristics and Treatment Follow-Up of Patients in Isfahan City, Iran.Adv Biomed Res. 2023 Oct 28;12:239. doi: 10.4103/abr.abr_168_23. eCollection 2023. Adv Biomed Res. 2023. PMID: 38073727 Free PMC article.
References
-
- Ahsan MK, Awwal MA, Khan SI, Haque MH, Zaman N. Intradural extramedullary spinal cord tumours: A retrospective study of surgical outcomes. Bangabandhu Sheikh Mujib Med Univ J. 2016;9:11–9.
-
- Cohen-Gadol AA, Zikel OM, Koch CA, Scheithauer BW, Krauss WE. Spinal meningiomas in patients younger than 50 years of age: A 21-year experience. J Neurosurg. 2003;98(Suppl 3):258–63. - PubMed
-
- Govind M, Mittal R, Sharma A, Gandhi A. Intradural extramedullary spinal cord tumors: A retrospective study at tertiary referral hospital. Rom Neurosurg. 2016;30:106–12.
-
- Mehta AI, Adogwa O, Karikari IO, Thompson P, Verla T, Null UT, et al. Anatomical location dictating major surgical complications for intradural extramedullary spinal tumors: A 10-year single-institutional experience. J Neurosurg Spine. 2013;19:701–7. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
