Predictors of mortality and loss to follow-up among drug resistant tuberculosis patients in Oromia Hospitals, Ethiopia: A retrospective follow-up study
- PMID: 33956812
- PMCID: PMC8101723
- DOI: 10.1371/journal.pone.0250804
Predictors of mortality and loss to follow-up among drug resistant tuberculosis patients in Oromia Hospitals, Ethiopia: A retrospective follow-up study
Abstract
Background: Drug resistance tuberculosis (DR-TB) patients' mortality and loss to follow-up (LTF) from treatment and care is a growing worry in Ethiopia. However, little is known about predictors of mortality and LTF among drug-resistant tuberculosis patients in Oromia region, Ethiopia. The current study aimed to identify predictors of mortality and loss to follow-up among drug resistance tuberculosis patients in Oromia Hospitals, Ethiopia.
Methods: A retrospective follow up study was carried out from 01 November 2012 to 31 December 2017 among DR-TB patients after calculating sample size using single proportion population formula. Mean, median, Frequency tables and bar charts were used to describe patients' characteristics in the cohort. The Kaplan-Meier curve was used to estimate the probability of death and LTF after the treatment was initiated. The log-rank test was used to compare time to death and time to LTF. The Cox proportional hazard model was used to determine predictors of mortality and LTF after DR-TB diagnosis. The Crude and adjusted Cox proportional hazard ratio was used to measure the strength of association whereas p-value less than 0.05 were used to declare statistically significant predictors.
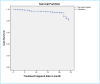
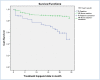
Result: A total of 406 DR-TB patients were followed for 7084 person-months observations. Among the patients, 71 (17.5%) died and 32 (7.9%) were lost to follow up (LTF). The incidence density of death and LTF in the cohort was 9.8 and 4.5 per 1000 person-months, respectively. The median age of the study participants was 28 years (IQR: 27.1, 29.1). The overall cumulative survival probability of patients at the end of 24 months was 77.5% and 84.5% for the mortality and LTF, respectively. The independent predictors of death was chest radiographic findings (AHR = 0.37, 95% CI: 0.17-0.79) and HIV serostatus 2.98 (95% CI: 1.72-5.19). Drug adverse effect (AHR = 6.1; 95% CI: 2.5, 14.34) and culture test result (AHR = 0.1; 95% CI: 0.1, 0.3) were independent predictors of LTF.
Conclusion: This study concluded that drug-resistant tuberculosis mortality and LTF remains high in the study area. Continual support of the integration of TB/HIV service with emphasis and work to identified predictors may help in reducing drug-resistant tuberculosis mortality and LTF.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures



References
-
- Nahid P, Mase SR, Migliori GB, Sotgiu G, Bothamley GH, Brozek JL, et al. Treatment of drug-resistant tuberculosis. An official ATS/CDC/ERS/IDSA clinical practice guideline. American journal of respiratory and critical care medicine. 2019;200(10):e93–e142. 10.1164/rccm.201909-1874ST - DOI - PMC - PubMed
-
- Branigan D. THE RIGHT TO QUALITY TB DIAGNOSTIC TESTING.
-
- Organization WH. Global tuberculosis report 2020. Global tuberculosis report 20202020.
-
- Organization WH. World Health Organization Global tuberculosis repot 2013. Gevena: World Health Organization. 2013.
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

