Prevalence and outcomes of co-infection and superinfection with SARS-CoV-2 and other pathogens: A systematic review and meta-analysis
- PMID: 33956882
- PMCID: PMC8101968
- DOI: 10.1371/journal.pone.0251170
Prevalence and outcomes of co-infection and superinfection with SARS-CoV-2 and other pathogens: A systematic review and meta-analysis
Abstract
Introduction: The recovery of other pathogens in patients with SARS-CoV-2 infection has been reported, either at the time of a SARS-CoV-2 infection diagnosis (co-infection) or subsequently (superinfection). However, data on the prevalence, microbiology, and outcomes of co-infection and superinfection are limited. The purpose of this study was to examine the occurrence of co-infections and superinfections and their outcomes among patients with SARS-CoV-2 infection.
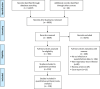
Patients and methods: We searched literature databases for studies published from October 1, 2019, through February 8, 2021. We included studies that reported clinical features and outcomes of co-infection or superinfection of SARS-CoV-2 and other pathogens in hospitalized and non-hospitalized patients. We followed PRISMA guidelines, and we registered the protocol with PROSPERO as: CRD42020189763.
Results: Of 6639 articles screened, 118 were included in the random effects meta-analysis. The pooled prevalence of co-infection was 19% (95% confidence interval [CI]: 14%-25%, I2 = 98%) and that of superinfection was 24% (95% CI: 19%-30%). Pooled prevalence of pathogen type stratified by co- or superinfection were: viral co-infections, 10% (95% CI: 6%-14%); viral superinfections, 4% (95% CI: 0%-10%); bacterial co-infections, 8% (95% CI: 5%-11%); bacterial superinfections, 20% (95% CI: 13%-28%); fungal co-infections, 4% (95% CI: 2%-7%); and fungal superinfections, 8% (95% CI: 4%-13%). Patients with a co-infection or superinfection had higher odds of dying than those who only had SARS-CoV-2 infection (odds ratio = 3.31, 95% CI: 1.82-5.99). Compared to those with co-infections, patients with superinfections had a higher prevalence of mechanical ventilation (45% [95% CI: 33%-58%] vs. 10% [95% CI: 5%-16%]), but patients with co-infections had a greater average length of hospital stay than those with superinfections (mean = 29.0 days, standard deviation [SD] = 6.7 vs. mean = 16 days, SD = 6.2, respectively).
Conclusions: Our study showed that as many as 19% of patients with COVID-19 have co-infections and 24% have superinfections. The presence of either co-infection or superinfection was associated with poor outcomes, including increased mortality. Our findings support the need for diagnostic testing to identify and treat co-occurring respiratory infections among patients with SARS-CoV-2 infection.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Comment in
-
Appropriate use of antimicrobial therapy for COVID-19 co-infection.Immunotherapy. 2021 Sep;13(13):1067-1070. doi: 10.2217/imt-2021-0134. Epub 2021 Jun 11. Immunotherapy. 2021. PMID: 34114473 Free PMC article. No abstract available.
References
-
- Centers for Disease Control and Prevention. Coronavirus Disease 2019 (COVID-19): cases in US 2020 [Available from: https://www.cdc.gov/coronavirus/2019-ncov/cases-updates/cases-in-us.html.
-
- The World Health Organization. Coronavirus disease (COVID-19) Pandemic 2020 [Available from: https://www.who.int/emergencies/diseases/novel-coronavirus-2019.
-
- The World Health Organization. Modes of transmission of virus causing COVID-19: implications for IPC precaution recommendations 2019 [Available from: https://www.who.int/news-room/commentaries/detail/modes-of-transmission-....
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous