Rates and Risk Factors for Interval Gastric Cancers at Screening Gastroscopy
- PMID: 33960944
- PMCID: PMC8975297
- DOI: 10.5152/tjg.2021.20129
Rates and Risk Factors for Interval Gastric Cancers at Screening Gastroscopy
Abstract
Backgrounds/aims: Interval gastric cancers (GCs) can be encountered during screening gastroscopy. This study investigated the rate of interval GCs and their risk factors.
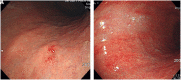
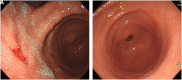
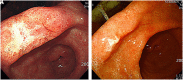
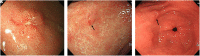
Materials and methods: We retrospectively investigated subjects who underwent screening gastroscopy from 2005 to 2017 in a university hospital and were diagnosed with GC. Subjects were grouped based on their endoscopic images and descriptive results into interval GC and initially diagnosed GC groups. Interval GCs were defined when endoscopic results within the previous 3 years were negative for GC. The clinico-pathological characteristics of the groups and risk factors for interval GCs were evaluated.
Results: Of 54 724 subjects who underwent screening gastroscopy, 234 were diagnosed with GC, of which 43 were interval GCs. The rate of interval GCs was 18.4% (43/234, mean age 61.6 years). Interval GCs were smaller than initially diagnosed GCs (1.6 vs 1.9 cm, P = .011). They were located in the low-to-mid-body in 44.2%, antrum in 48.8%, and high body and cardia in 7%. Their observation time was shorter (248.74 vs 410.64 sec, P = .032). In multivariate analysis, they were associated with short observation time (odds ratio [OR] 0.99, 95% CI 0.994-0.998, P < .001) and location in the low-to-mid-body (OR 2.12, 95% CI 1.071-4.181, P = .031), although differentiation, ulcerated type, metaplasia, Helicobacter pylori infection, and endoscopists' experience were not associated with interval GCs.
Conclusions: The rate of interval GCs was significant during screening gastroscopy. They might be reduced by increasing observation time, focusing on smaller lesions, and observing the low-to-mid-body of the stomach more carefully.
Conflict of interest statement
Figures


References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous
