Impact of photoreceptor density in a 3D simulation of panretinal laser photocoagulation
- PMID: 33962561
- PMCID: PMC8103585
- DOI: 10.1186/s12886-021-01945-z
Impact of photoreceptor density in a 3D simulation of panretinal laser photocoagulation
Abstract
Background: During panretinal photocoagulation (PRP), the outer retina, especially the photoreceptors, are destroyed. During such procedures, the impact of the retinal photocoagulation, which is performed in the same photocoagulated area, may change if it is applied to different locations with different photoreceptor densities. Thus, we aimed to evaluate the influence of photoreceptor density on PRP.
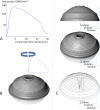
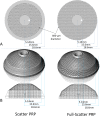
Methods: We constructed a three-dimensional (3D) average distribution of photoreceptors with 3D computer-aided design (CAD) software using previously derived photoreceptor density data and calculated the number of photoreceptors destroyed by scatter PRP and full-scatter PRP (size 400-μm on the retina, spacing 1.0 spot) using a geometry-based simulation. To investigate the impact of photoreceptor density on PRP, we calculated the ratio of the number of photoreceptors destroyed to the total number of photoreceptors, termed the photoreceptor destruction index.
Results: In this 3D simulation, the total number of photoreceptors was 96,571,900. The total number of photoreceptors destroyed by scatter PRP and full-scatter PRP were 15,608,200 and 19,120,600, respectively, and the respective photoreceptor destruction indexes were 16.2 and 19.8%, respectively.
Conclusions: Scatter PRP is expected to have 4/5 of the number of photoreceptors destroyed by full-scatter PRP.
Keywords: Computer based methods; Panretinal laser photocoagulation; Photocoagulation index; Photoreceptor density; Photoreceptor destruction index.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


Similar articles
-
Simulation of panretinal laser photocoagulation using geometric methods for calculating the photocoagulation index.Eur J Ophthalmol. 2017 Mar 10;27(2):205-209. doi: 10.5301/ejo.5000865. Epub 2016 Sep 13. Eur J Ophthalmol. 2017. PMID: 27646339
-
The impact of spot size, spacing, pattern, duration and intensity of burns on the photocoagulation index in a geometric simulation of pan-retinal laser photocoagulation.Acta Ophthalmol. 2019 Jun;97(4):e551-e558. doi: 10.1111/aos.13939. Epub 2018 Dec 3. Acta Ophthalmol. 2019. PMID: 30511421
-
High-resolution imaging of the human retina in vivo after scatter photocoagulation treatment using a semiautomated laser system.Ophthalmology. 2010 Mar;117(3):545-51. doi: 10.1016/j.ophtha.2009.07.031. Epub 2010 Jan 19. Ophthalmology. 2010. PMID: 20031226
-
Visual side effects of successful scatter laser photocoagulation surgery for proliferative diabetic retinopathy: a literature review.Retina. 2007 Sep;27(7):816-24. doi: 10.1097/IAE.0b013e318042d32c. Retina. 2007. PMID: 17891003 Review.
-
Photoreceptors in diabetic retinopathy.J Diabetes Investig. 2015 Jul;6(4):371-80. doi: 10.1111/jdi.12312. Epub 2015 Jan 7. J Diabetes Investig. 2015. PMID: 26221514 Free PMC article. Review.
Cited by
-
Gut microbiota alterations in children and their relationship with primary immune thrombocytopenia.Front Pediatr. 2023 Jun 21;11:1213607. doi: 10.3389/fped.2023.1213607. eCollection 2023. Front Pediatr. 2023. PMID: 37416817 Free PMC article.
-
Jatrorrhizine alleviates ulcerative colitis via regulating gut microbiota and NOS2 expression.Gut Pathog. 2022 Oct 21;14(1):41. doi: 10.1186/s13099-022-00514-z. Gut Pathog. 2022. PMID: 36271438 Free PMC article.
References
-
- Allingham R. Shields textbook of glaucoma. 6th ed: Alphen aan den Rijn: Wolters Kluwer; 2011. p. 294.
-
- Hoskins HD., Jr Neovascular glaucoma: current concepts. Trans Am Acad Ophthalmol Otolaryngol. 1974;78:330–333. - PubMed
-
- Ryan SJ. Retina. 6th ed: Philadelphia: Elsevier Saunders; 2017. p. 1105.
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

