Associations of midpoint of sleep and night sleep duration with type 2 diabetes mellitus in Chinese rural population: the Henan rural cohort study
- PMID: 33962597
- PMCID: PMC8106181
- DOI: 10.1186/s12889-021-10833-6
Associations of midpoint of sleep and night sleep duration with type 2 diabetes mellitus in Chinese rural population: the Henan rural cohort study
Abstract
Background: The study aimed to investigate the independent and combined effects of midpoint of sleep and night sleep duration on type 2 diabetes mellitus (T2DM) in areas with limited resources.
Methods: A total of 37,276 participants (14,456 men and 22,820 women) were derived from the Henan Rural Cohort Study. Sleep information was assessed based on the Pittsburgh Sleep Quality Index. Logistic regression models and restricted cubic splines were used to estimate the relationship of the midpoint of sleep and night sleep duration with T2DM.
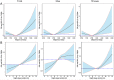
Results: Of the 37,276 included participants, 3580 subjects suffered from T2DM. The mean midpoint of sleep among the Early, Intermediate and Late groups were 1:05 AM ±23 min, 1:56 AM ±14 min, and 2:57 AM ±34 min, respectively. Compared to the Intermediate group, adjusted odds ratios (ORs) and 95% confidence interval (CI) of T2DM were 1.13 (1.04-1.22) and 1.14 (1.03-1.26) in the Early group and the Late group. Adjusted OR (95% CI) for T2DM compared with the reference (7- h) was 1.28 (1.08-1.51) for longer (≥ 10 h) night sleep duration. The combination of late midpoint of sleep and night sleep duration (≥ 9 h) increased 38% (95% CI 10-74%) prevalence of T2DM. These associations were more obvious in women than men.
Conclusions: Late and early midpoint of sleep and long night sleep duration were all associated with higher prevalence of T2DM. Meanwhile, midpoint of sleep and night sleep duration might have combined effects on the prevalence of T2DM, which provided potential health implications for T2DM prevention, especially in rural women.
Trial registration: The Henan Rural Cohort Study has been registered at Chinese Clinical Trial Register (Registration number: ChiCTR-OOC-15006699 ). Date of registration: 2015-07-06.
Keywords: Midpoint of sleep; Night sleep duration; Rural population; Type 2 diabetes mellitus.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
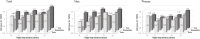
References
-
- Saeedi P, Salpea P, Karuranga S, Petersohn I, Malanda B, Gregg EW, Unwin N, Wild SH, Williams R. Mortality attributable to diabetes in 20–79 years old adults, 2019 estimates: Results from the International Diabetes Federation Diabetes Atlas, 9(th) edition. Diabetes Res Clin Pract. 2020;162:108086. doi: 10.1016/j.diabres.2020.108086. - DOI - PubMed
-
- Williams R, Karuranga S, Malanda B, Saeedi P, Basit A, Besançon S, Bommer C, Esteghamati A, Ogurtsova K, Zhang P, Colagiuri S. Global and regional estimates and projections of diabetes-related health expenditure: Results from the International Diabetes Federation Diabetes Atlas, 9th edition. Diabetes Res Clin Pract. 2020;162:108072. doi: 10.1016/j.diabres.2020.108072. - DOI - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
- 2016YFC0900803/Foundation of National Key Program of Research and Development of China
- 81573243, 81602925/National Natural Science Foundation of China
- 201702367, 2017T02098/Foundation of Medical Science and Technology of Henan province
- 182300410293/Henan Natural Science Foundation of China
- XKZDQY202008, XKZDQY202002/Discipline Key Research and Development Program of Zhengzhou University
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

