Subjective cognition and mood in persistent chemotherapy-related cognitive impairment
- PMID: 33973154
- PMCID: PMC9390086
- DOI: 10.1007/s11764-021-01055-1
Subjective cognition and mood in persistent chemotherapy-related cognitive impairment
Abstract
Purpose: Persistent chemotherapy-related cognitive impairment (CRCI) is commonly reported following cancer treatment and negatively affects quality of life. While past research has focused on potential pathophysiological mechanisms underlying this relationship, the role of psychological factors, such as mood, stress, and anxiety, in the development of persistent CRCI has received less attention. As an additional analysis of data from a trial investigating the effects of transdermal nicotine patches on cognitive performance in patients with persistent CRCI, we examined whether change in mood was associated with changes in subjective and objective cognitive functioning.
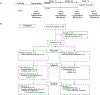
Methods: Participants were randomized to either placebo (n = 11) or transdermal nicotine (n = 11) for 6 weeks, followed by 2 weeks of treatment withdrawal for a total of 8 weeks. Participants were assessed using behavioral, subjective, and objective measures of cognitive functioning and mood at five visits before, during, and after treatment.
Results: Although we did not detect an effect of treatment assignment on mood, over the course of the study, we observed a significant improvement on measures of mood that correlated with improvement in subjective and objective cognitive performance.
Conclusions: We observed improvement in objective and subjective cognitive performance measures. These changes were associated with improvement in subsyndromal mood symptoms, likely resulting from participation in the trial itself.
Implications for cancer survivors: These results suggest that women with persistent CRCI may benefit from support and validation of their cognitive complaints, cognitive rehabilitation/therapies into their post-cancer care.
Trial registration: The study was registered with clinicaltrials.gov (trial registration: NCT02312943).
Keywords: Breast cancer; Chemotherapy-related cognitive impairment; Cognitive impairment; Survivorship.
© 2021. The Author(s), under exclusive licence to Springer Science+Business Media, LLC, part of Springer Nature.
Conflict of interest statement
Figures



Similar articles
-
Nicotinic treatment of post-chemotherapy subjective cognitive impairment: a pilot study.J Cancer Surviv. 2019 Oct;13(5):673-686. doi: 10.1007/s11764-019-00786-6. Epub 2019 Jul 23. J Cancer Surviv. 2019. PMID: 31338732 Free PMC article. Clinical Trial.
-
Transdermal Nicotine for the Treatment of Mood and Cognitive Symptoms in Nonsmokers With Late-Life Depression.J Clin Psychiatry. 2018 Aug 28;79(5):18m12137. doi: 10.4088/JCP.18m12137. J Clin Psychiatry. 2018. PMID: 30192444 Free PMC article. Clinical Trial.
-
Self-reported chemotherapy-related cognitive impairment compared with cognitive complaints following menopause.Psychooncology. 2018 Sep;27(9):2198-2205. doi: 10.1002/pon.4796. Epub 2018 Jul 13. Psychooncology. 2018. PMID: 29904964 Free PMC article.
-
Chemotherapy-induced cognitive impairment in breast cancer survivors: A systematic review of studies from 2000 to 2021.Cancer Rep (Hoboken). 2024 Feb;7(2):e1989. doi: 10.1002/cnr2.1989. Cancer Rep (Hoboken). 2024. PMID: 38351543 Free PMC article.
-
A systematic review of rehabilitation programs for cognitive impairment related to breast cancer: Different programs at different times?Ann Phys Rehabil Med. 2024 Jun;67(5):101832. doi: 10.1016/j.rehab.2024.101832. Epub 2024 Mar 26. Ann Phys Rehabil Med. 2024. PMID: 38537525
Cited by
-
Breast Cancer Survivorship: the Role of Rehabilitation According to the International Classification of Functioning Disability and Health-a Scoping Review.Curr Oncol Rep. 2022 Sep;24(9):1163-1175. doi: 10.1007/s11912-022-01262-8. Epub 2022 Apr 11. Curr Oncol Rep. 2022. PMID: 35403973 Free PMC article.
-
An Evaluation of the Multifactorial Model of Cancer-Related Cognitive Impairment.Nurs Res. 2023 Jul-Aug 01;72(4):272-280. doi: 10.1097/NNR.0000000000000660. Epub 2023 Apr 24. Nurs Res. 2023. PMID: 37104681 Free PMC article.
-
Effects of immersive virtual therapy on psychological and physical wellbeing in women with breast cancer at different stages of disease and treatment conditions: an experimental comparative study.Front Oncol. 2025 Aug 4;15:1581604. doi: 10.3389/fonc.2025.1581604. eCollection 2025. Front Oncol. 2025. PMID: 40831925 Free PMC article.
-
Accounting for unmet needs resulting from cancer-related cognitive impairment.J Cancer Surviv. 2025 Mar 11. doi: 10.1007/s11764-025-01769-6. Online ahead of print. J Cancer Surviv. 2025. PMID: 40067418
References
-
- Yang Y, Hendrix CC. Cancer-related cognitive impairment in breast cancer patients: influences of psychological variables. Asia-Pacific J Oncol Nurs. 2018;5:296–306 Available from: http://www.ncbi.nlm.nih.gov/pubmed/29963592. - PMC - PubMed
-
- Janelsins MC, Kohli S, Mohile SG, Usuki K, Ahles TA, Morrow GR. An update on cancer- and chemotherapy-related cognitive dysfunction: current status. Semin Oncol. 2011;38:431–8 Available from: http://www.sciencedirect.com/science/article/pii/S0093775411000844. - PMC - PubMed
-
- Wefel JS, Kesler SR, Noll KR, Schagen SB. Clinical characteristics, pathophysiology, and management of noncentral nervous system cancer-related cognitive impairment in adults. CA Cancer J Clin. 2015;65:123–38 Available from: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=4355212&tool=p.... - PMC - PubMed
-
- Derogatis LR, Morrow GR, Fetting J, Penman D, Piasetsky S, Schmale AM, et al. The prevalence of psychiatric disorders among cancer patients. JAMA. 1983;249:751–7 Available from: http://www.ncbi.nlm.nih.gov/pubmed/6823028. - PubMed
-
- Lloyd-Williams M, Friedman T. Depression in palliative care patients—a prospective study. Eur J Cancer Care (Engl). 2001;10: 270–4 Available from: http://www.ncbi.nlm.nih.gov/pubmed/11806678. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

