Genetic causes of neonatal and infantile hypercalcaemia
- PMID: 33990852
- PMCID: PMC8816529
- DOI: 10.1007/s00467-021-05082-z
Genetic causes of neonatal and infantile hypercalcaemia
Abstract
The causes of hypercalcaemia in the neonate and infant are varied, and often distinct from those in older children and adults. Hypercalcaemia presents clinically with a range of symptoms including failure to thrive, poor feeding, constipation, polyuria, irritability, lethargy, seizures and hypotonia. When hypercalcaemia is suspected, an accurate diagnosis will require an evaluation of potential causes (e.g. family history) and assessment for physical features (such as dysmorphology, or subcutaneous fat deposits), as well as biochemical measurements, including total and ionised serum calcium, serum phosphate, creatinine and albumin, intact parathyroid hormone (PTH), vitamin D metabolites and urinary calcium, phosphate and creatinine. The causes of neonatal hypercalcaemia can be classified into high or low PTH disorders. Disorders associated with high serum PTH include neonatal severe hyperparathyroidism, familial hypocalciuric hypercalcaemia and Jansen's metaphyseal chondrodysplasia. Conditions associated with low serum PTH include idiopathic infantile hypercalcaemia, Williams-Beuren syndrome and inborn errors of metabolism, including hypophosphatasia. Maternal hypocalcaemia and dietary factors and several rare endocrine disorders can also influence neonatal serum calcium levels. This review will focus on the common causes of hypercalcaemia in neonates and young infants, considering maternal, dietary, and genetic causes of calcium dysregulation. The clinical presentation and treatment of patients with these disorders will be discussed.
Keywords: Calcium homeostasis; Genetic disease; Parathyroid hormone; Phosphate; Vitamin D.
© 2021. The Author(s).
Conflict of interest statement
The authors declare no conflict of interest.
Figures
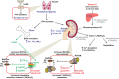
References
-
- Kovacs CS. In: Calcium and phosphate metabolism and related disorders during pregnancy and lactation. Feingold KR, Anawalt B, Boyce A, Chrousos G, de Herder WW, Dungan K, Grossman A, Hershman JM, Hofland J, Kaltsas G, Koch C, Kopp P, Korbonits M, McLachlan R, Morley JE, New M, Purnell J, Singer F, Stratakis CA, Trence DL, Wilson DP, editors. South Dartmouth, MA: Endotext; 2000. - PubMed
-
- Tsang RC, Strub R, Brown DR, Steichen J, Hartman C, Chen IW. Hypomagnesemia in infants of diabetic mothers: perinatal studies. J Pediatr. 1976;89:115–119. - PubMed
Publication types
MeSH terms
Substances
Supplementary concepts
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

