The risk of venous thromboembolism associated with midline catheters compared with peripherally inserted central catheters: A systematic review and meta-analysis
- PMID: 33991462
- PMCID: PMC8994959
- DOI: 10.1002/nop2.935
The risk of venous thromboembolism associated with midline catheters compared with peripherally inserted central catheters: A systematic review and meta-analysis
Abstract
Background: Both midline catheters (MCs) and peripherally inserted central catheters (PICCs) can cause venous thromboembolism (VTE), but the prevalence associated with each is controversial.
Objective: To compare the risk of VTE between MCs and PICCs with a systematic review and meta-analysis.
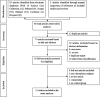
Methods: The Web of Science Core Collection, PubMed, Scopus, Embase, the Cochrane Library and ProQuest were searched from inception to January 2020. All studies comparing the risk of VTE between MCs and PICCs were included. Selected studies were assessed for methodological quality using the Downs and Black checklist. Two authors independently assessed the literature and extracted the data. Any different opinion was resolved through third-party consensus. Meta-analyses were conducted to generate estimates of VTE risk in patients with MCs versus PICCs, and publication bias was evaluated with RevMan 5.3.
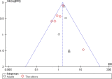
Results: A total of 86 studies were identified. Twelve studies were recruited, involving 40,871 patients. The prevalence of VTE with MCs and PICCs was 3.97% (310/7806) and 2.29% (758/33065), respectively. Meta-analysis showed that the prevalence of VTE with MCs was higher than that with PICCs (RR=1.53, 95% CI: 1.33-1.76, p < .00001). Subgroup analyses by age showed that the prevalence of VTE with MCs was higher than that with PICCs in the adult group (RR=1.75, 95% CI: 1.38-2.22, p < .00001), and higher than that with PICCs in the other subgroups (RR=1.42, 95% CI: 1.19-1.69, p = .0001). Subgroup analyses by nation showed that the prevalence of VTE with MCs was higher than that with PICCs (RR=1.50, 95% CI: 1.30-1.73, p < .00001) in US subgroup and higher than that with PICCs (RR=2.87, 95% CI: 1.24-6.65, p = .01) in the other nations. The sensitivity analysis shows that the results from this meta-analysis are robust and all studies have no significant publication bias.
Conclusions: This study provides the first systematic assessment of the risk of VTE between MCs and PICCs. MCs are associated with a higher risk of VTE than PICCs in all patients and adults. The findings of this study have several important implications for future practice. However, the risk of VTE between MCs and PICCs in children is unclear.
Keywords: complication; intravenous therapy; midline catheter; peripherally inserted central catheter; systematic review; venous thromboembolism.
© 2021 The Authors. Nursing Open published by John Wiley & Sons Ltd.
Conflict of interest statement
None of the authors have any financial and personal relationships with other people or organizations that could inappropriately influence their work.
Figures
Similar articles
-
Risk of catheter-related bloodstream infection associated with midline catheters compared with peripherally inserted central catheters: A meta-analysis.Nurs Open. 2021 May;8(3):1292-1300. doi: 10.1002/nop2.746. Epub 2020 Dec 29. Nurs Open. 2021. PMID: 33372316 Free PMC article.
-
A meta-analysis of the comparison of phlebitis between midline catheters and peripherally inserted central catheters in infusion therapy.Int J Nurs Pract. 2022 Apr;28(2):e12976. doi: 10.1111/ijn.12976. Epub 2021 Jun 1. Int J Nurs Pract. 2022. PMID: 34075655
-
Comparison of Venous Thrombosis Complications in Midlines Versus Peripherally Inserted Central Catheters: Are Midlines the Safer Option?Clin Appl Thromb Hemost. 2019 Jan-Dec;25:1076029619839150. doi: 10.1177/1076029619839150. Clin Appl Thromb Hemost. 2019. PMID: 30909723 Free PMC article.
-
The effect of laterality on venous thromboembolism formation after peripherally inserted central catheter placement.J Vasc Access. 2012 Jan-Mar;13(1):91-5. doi: 10.5301/jva.5000014. J Vasc Access. 2012. PMID: 21948128
-
Complications of peripherally inserted central catheters in pregnancy: a systematic review and meta-analysis.J Matern Fetal Neonatal Med. 2022 May;35(9):1739-1746. doi: 10.1080/14767058.2020.1769591. Epub 2020 May 22. J Matern Fetal Neonatal Med. 2022. PMID: 32441173
Cited by
-
The research status of central venous catheterization-associated thrombosis: a bibliometrics analysis.Ann Transl Med. 2022 May;10(10):561. doi: 10.21037/atm-22-1552. Ann Transl Med. 2022. PMID: 35722404 Free PMC article.
-
Thrombosis and infections associated with PICC in onco-hematological patients, what is their relevance?Clin Transl Oncol. 2024 Dec;26(12):3226-3235. doi: 10.1007/s12094-024-03548-8. Epub 2024 Jun 12. Clin Transl Oncol. 2024. PMID: 38865035
-
Midline catheter (10 cm) versus long peripheral intravenous catheter (6.4 cm): Randomized clinical trial protocol with economic analysis.PLoS One. 2025 Apr 24;20(4):e0319587. doi: 10.1371/journal.pone.0319587. eCollection 2025. PLoS One. 2025. PMID: 40273075 Free PMC article.
-
The Association of Vasopressor Administration through a Midline Catheter with Catheter-related Complications.Ann Am Thorac Soc. 2023 Jul;20(7):1003-1011. doi: 10.1513/AnnalsATS.202209-814OC. Ann Am Thorac Soc. 2023. PMID: 37166852 Free PMC article.
-
Risk factors analysis and the establishment of nomogram prediction model for PICC-related venous thrombosis in patients with lymphoma: a double-center cohort-based case-control study.Front Oncol. 2024 Mar 15;14:1347297. doi: 10.3389/fonc.2024.1347297. eCollection 2024. Front Oncol. 2024. PMID: 38559558 Free PMC article.
References
-
- Al‐Asadi, O. , Almusarhed, M. , & Eldeeb, H. (2019). Predictive risk factors of venous thromboembolism (VTE) associated with peripherally inserted central catheters (PICC) in ambulant solid cancer patients: Retrospective single Centre cohort study. Thrombosis Journal, 17, 2. 10.1186/s12959-019-0191-y - DOI - PMC - PubMed
-
- Benali, S. , Rypens, F. , Lacroix, J. , Dubois, J. , & Garel, L. (2013). Midline catheters versus peripherally inserted central catheters (PICC) in children: A randomized clinical trial. Pediatric Radiology, 43(S3), S541.
-
- Chopra, V. , Kaatz, S. , Swaminathan, L. , Boldenow, T. , Snyder, A. , Burris, R. , Bernstein, S. J. , & Flanders, S. (2019). Variation in use and outcomes related to midline catheters: Results from a multicentre pilot study. BMJ Quality & Safety, 28(9), 714–720. 10.1136/bmjqs-2018-008554 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources