Maximal Voluntary Breath-Holding Tele-Inspiratory Test in Patients with Chronic Obstructive Pulmonary Disease
- PMID: 33993797
- PMCID: PMC8127757
- DOI: 10.1177/15579883211015857
Maximal Voluntary Breath-Holding Tele-Inspiratory Test in Patients with Chronic Obstructive Pulmonary Disease
Abstract
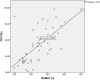
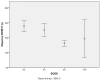
Maximal voluntary inspiratory breath-holding time (MVIBHT) has proved to be of clinical utility in some obstructive ventilatory defects. This study aims to correlate the breath-holding time with pulmonary function tests in patients with chronic obstructive pulmonary disease (COPD) and to determine the feasibility of using a breath-holding test in assessing the severity of COPD.A cross-sectional study including male patients with stable COPD were conducted. Patients with respiratory comorbidities and severe or unstable cardiac diseases were excluded. Patients were interviewed and examined. Six-minute walk test (6MWT) and plethysmography were performed.For MVIBHT collection, the subject was asked to inspire deeply and to hold the breath as long as possible at the maximum inspiratory level. This maneuver was repeated three times. The best value was used for further analysis.A total of 79 patients (mean age: 64.2 ± 8) were included in this study. The mean value of MVIBHT was 24.2 ± 8.5 s. We identified a positive and significant correlations between MVIBHT and forced vital capacity (r = .630; p < .001) as well as MVIBHT and forced expiratory volume in 1 s (FEV1%) (r = .671; p < .001). A significant inverse correlation with total lung capacity (r = -.328; p = .019) and residual volume to total lung capacity ratio (r = -.607; p < .001) was noted. MVIBHT was significantly correlated to the distance in the 6MWT (r = .494; p < .001). The mean MVIBHT was significantly different within spirometric grades (p < .001) and GOLD groups (p = .002). At 20.5 s, MVIBHT had a sensitivity of 72% and specificity of 96% in determining COPD patients with FEV1 <50%.Our results provide additional evidence of the usefulness of MVIBHT in COPD patients as a pulmonary function parameter.
Keywords: apnea; breathing test; chronic obstructive pulmonary disease; pulmonary function; six minute walk test; spirometry.
Conflict of interest statement
Figures
Similar articles
-
The relationship between exercise capacity and different functional markers in pulmonary rehabilitation for COPD.Int J Chron Obstruct Pulmon Dis. 2018 Feb 28;13:717-724. doi: 10.2147/COPD.S153525. eCollection 2018. Int J Chron Obstruct Pulmon Dis. 2018. PMID: 29535512 Free PMC article.
-
The relationship between steps of 6MWT and COPD severity: a cross-sectional study.Int J Chron Obstruct Pulmon Dis. 2018 Dec 28;14:141-148. doi: 10.2147/COPD.S188994. eCollection 2019. Int J Chron Obstruct Pulmon Dis. 2018. PMID: 30643400 Free PMC article.
-
Relation of exercise capacity with lung volumes before and after 6-minute walk test in subjects with COPD.Respir Care. 2014 Nov;59(11):1687-95. doi: 10.4187/respcare.03082. Epub 2014 Sep 23. Respir Care. 2014. PMID: 25249649
-
Diagnostic management of chronic obstructive pulmonary disease.Neth J Med. 2012 Jan;70(1):6-11. Neth J Med. 2012. PMID: 22271808 Review.
-
The impacts of parity on spirometric parameters: a systematic review.Expert Rev Respir Med. 2021 Sep;15(9):1169-1185. doi: 10.1080/17476348.2021.1935246. Epub 2021 Jun 23. Expert Rev Respir Med. 2021. PMID: 34033730
Cited by
-
Body Oxygen Level Test (BOLT) is not associated with exercise performance in highly-trained individuals.Front Physiol. 2024 Aug 28;15:1430837. doi: 10.3389/fphys.2024.1430837. eCollection 2024. Front Physiol. 2024. PMID: 39290618 Free PMC article.
-
Aerosol Plumes of Inhalers Used in COPD.Pulm Ther. 2024 Mar;10(1):109-122. doi: 10.1007/s41030-023-00249-5. Epub 2024 Jan 9. Pulm Ther. 2024. PMID: 38194194 Free PMC article.
References
-
- Adeloye D., Chua S., Lee C., Basquill C., Papana A., Theodoratou E., Nair H., Gasevic D., Sridhar D., Campbell H., Chan K. Y., Sheikh A., Rudan I., & Global Health Epidemiology Reference Group (GHERG). (2015). Global and regional estimates of COPD prevalence: Systematic review and meta-analysis. Journal of Global Health, 5(2), 020415. 10.7189/jogh.05-020415 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

