Recurrent and Treatment-Unresponsive Spontaneous Bacterial Peritonitis Worsens survival in Decompensated Liver Cirrhosis
- PMID: 33994716
- PMCID: PMC8103328
- DOI: 10.1016/j.jceh.2020.08.010
Recurrent and Treatment-Unresponsive Spontaneous Bacterial Peritonitis Worsens survival in Decompensated Liver Cirrhosis
Abstract
Background: Spontaneous bacterial peritonitis (SBP) remains a major complication of cirrhosis. However, the incidence and the real impact of SBP in determining patient survival rates remain unclear. This study aims to evaluate the incidence and risk factors for SBP development and the role of SBP in predicting transplant-free survival.
Methods: Two hundred two consecutive patients underwent 492 paracenteses with biochemical and microbiological analysis of the ascitic fluid. When multiple paracenteses had been performed on a given patient, the first SBP-positive paracentesis or the first paracentesis conducted when none was diagnostic for SBP was included in the study.
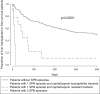
Results: SBP was detected in 28 of 202 (13.9%) patients; in 26 of 28 patients, the neutrophil count in the ascitic fluid was ≥250 cells/μl, and in 15 of 28 patients, the cultures were positive. Variables independently associated with SBP were as follows: a higher model of end-stage liver disease (MELD) score, the serum glucose value, elevated CRP serum levels, and higher potassium serum levels. Overall, the median (range) transplant-free survival was 289 (54-1253) days. One hundred (49.5%) patients died, whereas 35 patients (17.3%) underwent liver transplantation. Independent predictors of death or liver transplantation were a higher MELD score and the development of SBP, especially if it was antibiotic-resistant or recurrent SBP.
Conclusion: The occurrence of SBP is associated with more severe liver dysfunction in conjunction with the presence of inflammation. Unlike the occurrence of SBP per se, failure of first-line antibiotic treatment and SBP recurrence appear to strongly influence the mortality rate.
Keywords: ALP, alkaline phosphatase; ALT, alanine aminotransferase; AST, aspartate aminotransferase; BMI, body mass index; CLIF-SOFA, chronic liver failure-sequential organ failure assessment; CP, Child-Pugh; CRP, C-reactive protein; EPS, hepatic encephalopathy; HBV, hepatitis B virus; HCV, hepatitis C virus; INR, international normalized ratio; LT, liver transplantation; MELD, model of end-stage liver disease; OR, odds ratio; PLT, platelet; SBP, Spontaneous bacterial peritonitis; SIRS, systemic inflammatory response syndrome; WBC, white blood cell; antibiotic-resistant infections; ascites; gGT, gamma-glutamyl transpeptidase; liver transplantation; survival.
© 2020 Indian National Association for Study of the Liver. Published by Elsevier B.V. All rights reserved.
Figures
Similar articles
-
Overview of Complications in Cirrhosis.J Clin Exp Hepatol. 2022 Jul-Aug;12(4):1150-1174. doi: 10.1016/j.jceh.2022.04.021. Epub 2022 May 14. J Clin Exp Hepatol. 2022. PMID: 35814522 Free PMC article. Review.
-
Risk factors for development of spontaneous bacterial peritonitis and subsequent mortality in cirrhotic patients with ascites.Liver Int. 2015 Sep;35(9):2121-8. doi: 10.1111/liv.12795. Epub 2015 Feb 18. Liver Int. 2015. PMID: 25644943
-
Level of MFAP4 in ascites independently predicts 1-year transplant-free survival in patients with cirrhosis.JHEP Rep. 2021 Mar 29;3(3):100287. doi: 10.1016/j.jhepr.2021.100287. eCollection 2021 Jun. JHEP Rep. 2021. PMID: 34041469 Free PMC article.
-
Determinants of Outcomes in Autoimmune Hepatitis Presenting as Acute on Chronic Liver Failure Without Extrahepatic Organ Dysfunction upon Treatment With Steroids.J Clin Exp Hepatol. 2021 Mar-Apr;11(2):171-180. doi: 10.1016/j.jceh.2020.08.007. Epub 2020 Aug 22. J Clin Exp Hepatol. 2021. PMID: 33746441 Free PMC article.
-
Surgery in a patient with liver disease.J Clin Exp Hepatol. 2012 Sep;2(3):238-46. doi: 10.1016/j.jceh.2012.05.003. Epub 2012 Sep 21. J Clin Exp Hepatol. 2012. PMID: 25755440 Free PMC article. Review.
Cited by
-
Therapeutic effect of autologous bone marrow cells injected into the liver under the guidance of B‑ultrasound in the treatment of HBV‑related decompensated liver cirrhosis.Exp Ther Med. 2022 Aug 22;24(4):633. doi: 10.3892/etm.2022.11570. eCollection 2022 Oct. Exp Ther Med. 2022. PMID: 36160909 Free PMC article.
-
Application of mNGS in the Etiological Diagnosis of Thoracic and Abdominal Infection in Patients With End-Stage Liver Disease.Front Cell Infect Microbiol. 2022 Jan 5;11:741220. doi: 10.3389/fcimb.2021.741220. eCollection 2021. Front Cell Infect Microbiol. 2022. PMID: 35071029 Free PMC article.
-
Variables associated with antibiotic administration for performing paracentesis among patients with ascites in a community hospital.Clin Exp Hepatol. 2024 Mar;10(1):47-52. doi: 10.5114/ceh.2024.136215. Epub 2024 Mar 28. Clin Exp Hepatol. 2024. PMID: 38765905 Free PMC article.
-
Overview of Complications in Cirrhosis.J Clin Exp Hepatol. 2022 Jul-Aug;12(4):1150-1174. doi: 10.1016/j.jceh.2022.04.021. Epub 2022 May 14. J Clin Exp Hepatol. 2022. PMID: 35814522 Free PMC article. Review.
-
Serum copeptin is associated with major complications of liver cirrhosis and spontaneous bacterial peritonitis.Clin Exp Hepatol. 2023 Mar;9(1):71-78. doi: 10.5114/ceh.2023.125970. Epub 2023 Mar 21. Clin Exp Hepatol. 2023. PMID: 37064833 Free PMC article.
References
-
- Evans L.T., Kim W.R., Poterucha J.J., Kamath P.S. Spontaneous bacterial peritonitis in asymptomatic outpatients with cirrhotic ascites. Hepatology. 2003;37:897–901. - PubMed
-
- Oliveira A.M., Branco J.C., Barosa R. Clinical and microbiological characteristics associated with mortality in spontaneous bacterial peritonitis: a multicenter cohort study. Eur J Gastroenterol Hepatol. 2016;28:1216–1222. - PubMed
-
- Rimola A., Garcia-Tsao G., Navasa M. Diagnosis, treatment and prophylaxis of spontaneous bacterial peritonitis: a consensus document. International Ascites Club. J Hepatol. 2000;32:142–153. - PubMed
-
- Piano S., Fasolato S., Salinas F. The empirical antibiotic treatment of nosocomial spontaneous bacterial peritonitis: results of a randomized, controlled clinical trial. Hepatology. 2016;63:1299–1309. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

