Role of Surgical Approach to Synchronous Colorectal Liver Metastases: A Retrospective Analysis
- PMID: 33994810
- PMCID: PMC8112857
- DOI: 10.2147/CMAR.S300890
Role of Surgical Approach to Synchronous Colorectal Liver Metastases: A Retrospective Analysis
Abstract
Purpose: This study is a retrospective analysis of exploring the efficiency of surgical management on patients with synchronous colorectal liver metastasis (SCLM).
Patients and methods: Nine hundred fifty-three consecutive patients with SCLM from Weifang People's Hospital of Shandong Province between January 2006 and December 2015 were reviewed. The values of different factors were analyzed, such as different surgical indications of liver metastases, simultaneous or staged resection of primary colorectal cancer and liver metastases, and primary tumor resection (PTR) of asymptomatic patients with unresectable liver metastases.
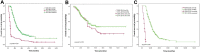
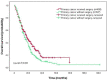
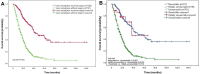
Results: Median survival time (47.3 months) and 5-year survival rate (31%) for patients with resected liver metastases were significantly superior to that of with nonoperative treatment (17.2 months, 4%, P<0.001); enlarging the standard of liver metastases resection can improve the resection rates (31.0% vs 13.6%, P<0.001); for patients with resectable liver metastases, the in-hospital cost for simultaneous resection group was lower than that in the staged resection group (36,698 vs 45,134 RMB, P<0.001); for patients of the asymptomatic primary tumor with unresectable liver metastases, PTR was associated with improved median survival (18.0 vs 15.0 months, P=0.006).
Conclusion: For patients with SCLM, liver resection is considered the best treatment; expanding indications of liver resection can improve the resection rates. Simultaneous resection of the primary tumor and liver metastases were indicated in patients with resectable SCLM; PTR was recommended for asymptomatic patients with unresectable hepatic metastases.
Keywords: primary tumor resection; surgical treatment; survival analysis; synchronous colorectal liver metastases.
© 2021 Zhai et al.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures


Similar articles
-
Simultaneous versus staged resection for synchronous colorectal liver metastases: A population-based cohort study.Int J Surg. 2020 Feb;74:68-75. doi: 10.1016/j.ijsu.2019.12.009. Epub 2019 Dec 14. Int J Surg. 2020. PMID: 31843676
-
Preoperative chemotherapy prior to primary tumour resection for asymptomatic synchronous unresectable colorectal liver-limited metastases: The RECUT multicenter randomised controlled trial.Eur J Cancer. 2023 Sep;191:112961. doi: 10.1016/j.ejca.2023.112961. Epub 2023 Jun 29. Eur J Cancer. 2023. PMID: 37473466 Clinical Trial.
-
The Role of Primary Tumor Resection in Colorectal Cancer Patients with Asymptomatic, Synchronous, Unresectable Metastasis: A Multicenter Randomized Controlled Trial.Cancers (Basel). 2020 Aug 16;12(8):2306. doi: 10.3390/cancers12082306. Cancers (Basel). 2020. PMID: 32824392 Free PMC article.
-
Primary tumor resection in colorectal cancer with unresectable synchronous metastases: A review.World J Gastrointest Oncol. 2014 Jun 15;6(6):156-69. doi: 10.4251/wjgo.v6.i6.156. World J Gastrointest Oncol. 2014. PMID: 24936226 Free PMC article. Review.
-
Treatment strategies for colorectal carcinoma with synchronous liver metastases: Which way to go?World J Gastroenterol. 2015 Jun 14;21(22):7014-21. doi: 10.3748/wjg.v21.i22.7014. World J Gastroenterol. 2015. PMID: 26078580 Free PMC article. Review.
Cited by
-
The Influence of Radiological "Disappearing Lesions" on the Efficacy and Prognosis of Patients with Colorectal Liver Metastases Undergoing Conversion Therapy.Gastroenterol Res Pract. 2022 Feb 22;2022:2200598. doi: 10.1155/2022/2200598. eCollection 2022. Gastroenterol Res Pract. 2022. PMID: 35242182 Free PMC article.
-
Laparoscopic Resection of Synchronous Liver Metastasis Involving the Left Hepatic Vein and the Common Trunk Bifurcation: A Strategy of Parenchyma-Sparing Resection with Left Sectionectomy and 4a Subsegmentectomy by Arantius Approach.Healthcare (Basel). 2022 Mar 11;10(3):517. doi: 10.3390/healthcare10030517. Healthcare (Basel). 2022. PMID: 35326995 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Other Literature Sources

