Incidence of relapse following a new approach to simplifying and optimising acute malnutrition treatment in children aged 6-59 months: a prospective cohort in rural Northern Burkina Faso
- PMID: 33996040
- PMCID: PMC8080230
- DOI: 10.1017/jns.2021.18
Incidence of relapse following a new approach to simplifying and optimising acute malnutrition treatment in children aged 6-59 months: a prospective cohort in rural Northern Burkina Faso
Abstract
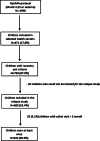
The present study aimed to determine the 3-month incidence of relapse and associated factors among children who recovered under the Optimising treatment for acute MAlnutrition (OptiMA) strategy, a MUAC-based protocol. A prospective cohort of children successfully treated for acute malnutrition was monitored between April 2017 and February 2018. Children were seen at home by community health workers (CHWs) every 2 weeks for 3 months. Relapse was defined as a child who had met OptiMA recovery criteria (MUAC ≥ 125 mm for two consecutive weeks) but subsequently had a MUAC < 125 mm at any home visit. Cumulative incidence and incidence rates per 100 child-months were estimated. Multivariable survival analysis was conducted using a shared frailty model with a random effect on health facilities to identify associated factors. Of the 640 children included, the overall 3-month cumulative incidence of relapse was 6⋅8 % (95 % CI 5⋅2, 8⋅8). Globally, the incidence rate of relapse was 2⋅5 (95 % CI 1⋅9, 3⋅3) per 100 child-months and 3⋅7 (95 % CI 1⋅9, 6⋅8) per 100 child-months among children admitted with a MUAC < 115 mm. Most (88⋅6 %) relapses were detected early when MUAC was between 120 and 124 mm. Relapse was positively associated with hospitalisation, with an adjusted hazard ratio (aHR) of 2⋅06 (95 % CI 1⋅01, 4⋅26) for children who had an inpatient stay at any point during treatment compared with children who did not. The incidence of relapse following recovery under OptiMA was relatively low in this context, but the lack of a standard relapse definition does not allow for comparison across settings Closer follow-up with caretakers whose children are admitted with MUAC < 115 mm or required hospitalisation during treatment should be considered in managing groups at high risk of relapse. Training caretakers to screen their children for relapse at home using MUAC could be more effective at detecting early relapse, and less costly, than home visits by CHWs.
Keywords: AM, acute malnutrition; Acute malnutrition; CHWs, community health workers; CIs, confidence intervals; CORTASAM, Council of Research & Technical Advice on Acute Malnutrition; Children; HAZ, height-for-age Z-score; IQR, interquartile range; Incidence; MAM, moderate acute malnutrition; MUAC, mid-upper arm circumference; MUAC-based and reduced doses protocol; OptiMA, Optimising treatment for acute MAlnutrition; RDT, rapid diagnostic tests; RUTF, ready-to-use therapeutic food; Relapse; SAM, severe acute malnutrition; WHO, World Health Organization; WHZ, weight-for-height Z-score; West Africa; aHR, adjusted hazard ratio; sd, standard deviation.
© The Author(s) 2021.
Figures

References
-
- Black RE, Victora CG, Walker SP, et al. (2013) Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet (Lond Engl) 382, 427–451. - PubMed
-
- UNICEF/WHO/World Bank Group. Levels and trends in child malnutrition. Key findings of the 2019 edition [Internet]. https://www.who.int/nutgrowthdb/jme-2019-key-findings.pdf?ua=1
-
- World Health Organization (WHO) (2013) Guideline: Updates on the Management of Severe Acute Malnutrition in Infants and Children. Geneva: WHO. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

