Natural history and prognostic implications of left ventricular end-diastolic pressure in reperfused ST-segment elevation myocardial infarction: an analysis of the thrombolysis in myocardial infarction (TIMI) II randomized controlled trial
- PMID: 34001032
- PMCID: PMC8130170
- DOI: 10.1186/s12872-021-02046-x
Natural history and prognostic implications of left ventricular end-diastolic pressure in reperfused ST-segment elevation myocardial infarction: an analysis of the thrombolysis in myocardial infarction (TIMI) II randomized controlled trial
Abstract
Background: The aim of the current study is to assess the natural history and prognostic value of elevated left ventricular end-diastolic pressure (LVEDP) in patients with ST-segment elevation myocardial infarction (STEMI) after reperfusion with thrombolysis; we utilize data from the Thrombolysis in Myocardial Infarction (TIMI) II study.
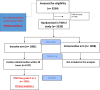
Methods: A total of 3339 patients were randomized to either an invasive (n = 1681) or a conservative (n = 1658) strategy in the TIMI II study following thrombolysis. To make the current cohort as relevant as possible to modern pharmaco-invasively managed cohorts, patients in the invasive arm with TIMI flow grade ≥ 2 (N = 1201) at initial catheterization are included in the analysis. Of these, 259 patients had a second catheterization prior to hospital discharge, and these were used to define the natural history of LVEDP in reperfused STEMI.
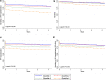
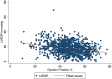
Results: The median LVEDP for the whole cohort was 18 mmHg (IQR: 12-23). Patients were divided into quartiles by LVEDP measured during the first cardiac catheterization. During a median follow up of 3 (IQR: 2.1-3.2) years, quartile 4 (highest LVEDP) had the highest incidence of mortality and heart failure admissions. In the cohort with paired catheterization data, the LVEDP dropped slightly from 18 mmHg (1QR: 12-22) to 15 mmHg (IQR: 10-20) (p = 0.01) from the first to the pre-hospital discharge catheterization.
Conclusions: LVEDP remains largely stable during hospitalisation post-STEMI. Elevated LVEDP is a predictor of death and heart failure hospitalization in STEMI patients undergoing successful thrombolysis.
Keywords: Left ventricular end diastolic pressure; ST-segment elevation myocardial infarction.
Conflict of interest statement
Author’s declare that they have no competing interests.
Figures
Similar articles
-
Targeting elevated left ventricular end-diastolic pressure following primary percutaneous coronary intervention for ST-segment elevation myocardial infarction - a phase one safety and feasibility study.Eur Heart J Acute Cardiovasc Care. 2020 Oct;9(7):758-763. doi: 10.1177/2048872618819657. Epub 2018 Dec 20. Eur Heart J Acute Cardiovasc Care. 2020. PMID: 30569736 Clinical Trial.
-
Efficacy and Safety of a Pharmaco-Invasive Strategy With Half-Dose Alteplase Versus Primary Angioplasty in ST-Segment-Elevation Myocardial Infarction: EARLY-MYO Trial (Early Routine Catheterization After Alteplase Fibrinolysis Versus Primary PCI in Acute ST-Segment-Elevation Myocardial Infarction).Circulation. 2017 Oct 17;136(16):1462-1473. doi: 10.1161/CIRCULATIONAHA.117.030582. Epub 2017 Aug 27. Circulation. 2017. PMID: 28844990 Clinical Trial.
-
Ratio of systolic blood pressure to left ventricular end-diastolic pressure at the time of primary percutaneous coronary intervention predicts in-hospital mortality in patients with ST-elevation myocardial infarction.Catheter Cardiovasc Interv. 2017 Sep 1;90(3):389-395. doi: 10.1002/ccd.26963. Epub 2017 Mar 17. Catheter Cardiovasc Interv. 2017. PMID: 28303647
-
Prognostic Value of LVEDP in Acute Myocardial Infarction: a Systematic Review and Meta-Analysis.J Cardiovasc Transl Res. 2018 Feb;11(1):33-35. doi: 10.1007/s12265-017-9776-7. Epub 2017 Dec 14. J Cardiovasc Transl Res. 2018. PMID: 29243014
-
The use of hemodynamics to predict mortality in patients undergoing primary PCI for ST-elevation myocardial infarction.Expert Rev Cardiovasc Ther. 2018 Aug;16(8):551-557. doi: 10.1080/14779072.2018.1497484. Epub 2018 Jul 13. Expert Rev Cardiovasc Ther. 2018. PMID: 29975560 Review.
Cited by
-
Impact of left ventricular end-diastolic pressure on clinical outcomes in patients with ST-elevation myocardial infarction (Hunter LVEDP Study): a prospective, single-centre study.BMJ Open. 2025 Jul 5;15(7):e090465. doi: 10.1136/bmjopen-2024-090465. BMJ Open. 2025. PMID: 40617602 Free PMC article.
-
Isovolumic relaxation intraventricular pressure difference predicts elevated left ventricular end-diastolic pressure in patients with coronary artery disease.Sci Rep. 2024 Nov 13;14(1):27764. doi: 10.1038/s41598-024-79278-2. Sci Rep. 2024. PMID: 39533061 Free PMC article.
-
Improvement in LV end-diastolic pressure after primary PCI and its impact on patients' recovery.Br J Cardiol. 2023 Nov 29;30(4):43. doi: 10.5837/bjc.2023.043. eCollection 2023. Br J Cardiol. 2023. PMID: 39247413 Free PMC article.
-
Support Pressure Acting on the Epicardial Surface of a Rat Left Ventricle-A Computational Study.Front Cardiovasc Med. 2022 Jul 6;9:850274. doi: 10.3389/fcvm.2022.850274. eCollection 2022. Front Cardiovasc Med. 2022. PMID: 35872914 Free PMC article.
References
-
- Burns RJ, Gibbons RJ, Yi Q, et al. The relationships of left ventricular ejection fraction, end-systolic volume index and infarct size to six month mortality after hospital discharge following myocardial infarction treated by thrombolysis. J Am Coll Cardiol. 2002;39:30–36. doi: 10.1016/S0735-1097(01)01711-9. - DOI - PubMed
-
- Halkin A, Singh M, Nikolsky E, Grines CL, Tcheng JE, Garcia E, Cox DA, Turco M, Stuckey TD, Na Y, Lansky AJ, Gersh BJ, O’Neill WW, Mehran R, Stone GW. Prediction of mortality after primary percutaneous coronary intervention for acute myocardial infarction: the CA-DILLAC risk score. J Am Coll Cardiol. 2005;45:1397–1405. doi: 10.1016/j.jacc.2005.01.041. - DOI - PubMed
-
- De Luca G, Suryapranata H, Hof AW, de Boer MJ, Hoorntje JC, Dambrink JH, Gosselink AT, Ottervanger JP, Zijlstra F. Prognostic assessment of patients with acute myocardial infarction treated with primary angioplasty: implications for early discharge. Circulation. 2004;109:2737–2743. doi: 10.1161/01.CIR.0000131765.73959.87. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

