Nomograms for Estimating Cause-Specific Death Rates of Patients With Inflammatory Breast Cancer: A Competing-Risks Analysis
- PMID: 34013802
- PMCID: PMC8141985
- DOI: 10.1177/15330338211016371
Nomograms for Estimating Cause-Specific Death Rates of Patients With Inflammatory Breast Cancer: A Competing-Risks Analysis
Abstract
Purpose: Inflammatory breast cancer (IBC) is a rare, aggressive and special subtype of primary breast cancer. We aimed to establish competing-risks nomograms to predict the IBC-specific death (BCSD) and other-cause-specific death (OCSD) of IBC patients.
Methods: We extracted data on primary IBC patients from the SEER (Surveillance, Epidemiology, and End Results) database by applying specific inclusion and exclusion criteria. Cumulative incidence function (CIF) was used to calculate the cumulative incidence rates and Gray's test was used to evaluate the difference between groups. Fine-Gray proportional subdistribution hazard method was applied to identify the independent predictors. We then established nomograms to predict the 1-, 3-, and 5-year cumulative incidence rates of BCSD and OCSD based on the results. The calibration curves and concordance index (C-index) were adopted to validate the nomograms.
Results: We enrolled 1699 eligible IBC patients eventually. In general, the 1-, 3-, and 5-years cumulative incidence rates of BCSD were 15.3%, 41.0%, and 50.7%, respectively, while those of OCSD were 3.0%, 5.1%, and 7.4%. The following 9 variables were independent predictive factors for BCSD: race, lymph node ratio (LNR), AJCC M stage, histological grade, ER (estrogen receptor) status, PR (progesterone receptor) status, HER-2 (human epidermal growth factor-like receptor 2) status, surgery status, and radiotherapy status. Meanwhile, age, ER, PR and chemotherapy status could predict OCSD independently. These factors were integrated for the construction of the competing-risks nomograms. The results of calibration curves and C-indexes indicated the nomograms had good performance.
Conclusions: Based on the SEER database, we established the first competing-risks nomograms to predict BCSD and OCSD of IBC patients. The good performance indicated that they could be incorporated in clinical practice to provide references for clinicians to make individualized treatment strategies.
Keywords: SEER; cause-specific death; competing-risks analysis; inflammatory breast cancer; nomogram.
Conflict of interest statement
Figures
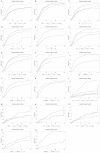


Similar articles
-
Competing-risks nomograms for predicting cause-specific mortality in parotid-gland carcinoma: A population-based analysis.Cancer Med. 2021 Jun;10(11):3756-3769. doi: 10.1002/cam4.3919. Epub 2021 May 7. Cancer Med. 2021. PMID: 33960711 Free PMC article.
-
Nomogram Predicting Cause-Specific Mortality in Nonmetastatic Male Breast Cancer: A Competing Risk Analysis.J Cancer. 2019 Jan 1;10(3):583-593. doi: 10.7150/jca.28991. eCollection 2019. J Cancer. 2019. PMID: 30719155 Free PMC article.
-
Competing-Risk Nomograms for Predicting the Prognosis of Patients With Infiltrating Lobular Carcinoma of the Breast.Clin Breast Cancer. 2021 Dec;21(6):e704-e714. doi: 10.1016/j.clbc.2021.03.008. Epub 2021 Mar 18. Clin Breast Cancer. 2021. PMID: 33846097
-
Inflammatory breast cancer: Epidemiologic data and therapeutic results.Int Rev Cell Mol Biol. 2024;384:1-23. doi: 10.1016/bs.ircmb.2023.10.003. Epub 2024 Feb 6. Int Rev Cell Mol Biol. 2024. PMID: 38637094 Review.
-
Systematic Review and Meta-Analysis of Treatment Effects on Survival in Patients with Inflammatory Breast Cancer.Asian Pac J Cancer Prev. 2023 Oct 1;24(10):3335-3343. doi: 10.31557/APJCP.2023.24.10.3335. Asian Pac J Cancer Prev. 2023. PMID: 37898836 Free PMC article.
Cited by
-
A nomogram for predicting survival in patients with gastrointestinal stromal tumor: a study based on the surveillance, epidemiology, and end results database.Front Med (Lausanne). 2024 May 23;11:1403189. doi: 10.3389/fmed.2024.1403189. eCollection 2024. Front Med (Lausanne). 2024. PMID: 38846147 Free PMC article.
-
Nomograms to predict the long-term prognosis for non-metastatic invasive lobular breast carcinoma: a population-based study.Sci Rep. 2024 Aug 22;14(1):19477. doi: 10.1038/s41598-024-68931-5. Sci Rep. 2024. PMID: 39174612 Free PMC article.
-
Prognostic prediction for inflammatory breast cancer patients using random survival forest modeling.Transl Oncol. 2025 Feb;52:102246. doi: 10.1016/j.tranon.2024.102246. Epub 2024 Dec 15. Transl Oncol. 2025. PMID: 39675249 Free PMC article.
-
How to Define Inflammatory Breast Cancer: A Systematic Review.Indian J Surg Oncol. 2025 Apr;16(2):393-400. doi: 10.1007/s13193-024-02094-7. Epub 2024 Sep 26. Indian J Surg Oncol. 2025. PMID: 40337028 Review.
-
Time-varying effect in older patients with early-stage breast cancer: a model considering the competing risks based on a time scale.Front Oncol. 2024 Jul 2;14:1352111. doi: 10.3389/fonc.2024.1352111. eCollection 2024. Front Oncol. 2024. PMID: 39015489 Free PMC article.
References
-
- Labidi SI, Mrad K, Mezlini A, et al. Inflammatory breast cancer in tunisia in the era of multimodality therapy. Ann Oncol. 2007;19(3):473–480. - PubMed
-
- Sutherland S, Ashley S, Walsh G, Smith IE, Johnston SRD. Inflammatory breast cancer-the royal marsden hospital experience. Cancer-Am Cancer Soc. 2010;116(11):2815–2820. - PubMed
-
- Dawood S. Biology and management of inflammatory breast cancer. Expert Rev Anticanc. 2010;10(2):209–220. - PubMed
-
- Warren LEG, Guo H, Regan MM, Nakhlis F, Yeh ED, Jacene HA. Inflammatory breast cancer: patterns of failure and the case for aggressive locoregional management. Ann Surg Oncol. 2015;22(8):2483–2491. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

