International Prospective Registry of Acute Coronary Syndromes in Patients With COVID-19
- PMID: 34016259
- PMCID: PMC8128002
- DOI: 10.1016/j.jacc.2021.03.309
International Prospective Registry of Acute Coronary Syndromes in Patients With COVID-19
Abstract
Background: Published data suggest worse outcomes in acute coronary syndrome (ACS) patients and concurrent coronavirus disease 2019 (COVID-19) infection. Mechanisms remain unclear.
Objectives: The purpose of this study was to report the demographics, angiographic findings, and in-hospital outcomes of COVID-19 ACS patients and compare these with pre-COVID-19 cohorts.
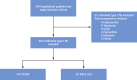
Methods: From March 1, 2020 to July 31, 2020, data from 55 international centers were entered into a prospective, COVID-ACS Registry. Patients were COVID-19 positive (or had a high index of clinical suspicion) and underwent invasive coronary angiography for suspected ACS. Outcomes were in-hospital major cardiovascular events (all-cause mortality, re-myocardial infarction, heart failure, stroke, unplanned revascularization, or stent thrombosis). Results were compared with national pre-COVID-19 databases (MINAP [Myocardial Ischaemia National Audit Project] 2019 and BCIS [British Cardiovascular Intervention Society] 2018 to 2019).
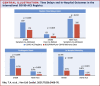
Results: In 144 ST-segment elevation myocardial infarction (STEMI) and 121 non-ST-segment elevation acute coronary syndrome (NSTE-ACS) patients, symptom-to-admission times were significantly prolonged (COVID-STEMI vs. BCIS: median 339.0 min vs. 173.0 min; p < 0.001; COVID NSTE-ACS vs. MINAP: 417.0 min vs. 295.0 min; p = 0.012). Mortality in COVID-ACS patients was significantly higher than BCIS/MINAP control subjects in both subgroups (COVID-STEMI: 22.9% vs. 5.7%; p < 0.001; COVID NSTE-ACS: 6.6% vs. 1.2%; p < 0.001), which remained following multivariate propensity analysis adjusting for comorbidities (STEMI subgroup odds ratio: 3.33 [95% confidence interval: 2.04 to 5.42]). Cardiogenic shock occurred in 20.1% of COVID-STEMI patients versus 8.7% of BCIS patients (p < 0.001).
Conclusions: In this multicenter international registry, COVID-19-positive ACS patients presented later and had increased in-hospital mortality compared with a pre-COVID-19 ACS population. Excessive rates of and mortality from cardiogenic shock were major contributors to the worse outcomes in COVID-19 positive STEMI patients.
Keywords: COVID-19; ST-segment elevation myocardial infarction; acute coronary syndrome; cardiogenic shock; non–ST-segment elevation myocardial infarction.
Copyright © 2021 American College of Cardiology Foundation. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Funding Support and Author Disclosures The study was supported by the Clinical Trials Unit at The University of Glasgow. Dr. Gale has received personal fees from AstraZeneca, Bayer, Boehringer Ingelheim, Daiichi-Sankyo, and Vifor Pharma; and has received grants from Abbott and Bristol Myers Squibb. Dr. Sabate has received personal fees from Abbott Vascular and IVascular. Dr. Sinagra has received personal fees from Biotronik, Boston Scientific, AstraZeneca, and Novartis. Dr. Savonitto has received personal fees from Bayer and Abbott. Dr. Curzen has received grants, personal fees, and nonfinancial support from Boston Scientific, Haemonetics, HeartFlow, and Abbott; has received grants from Beckmann Coulter; and has received nonfinancial support from Biosensors and Medtronic. Dr. Berry is supported by the British Heart Foundation (grant reference RE/18/6134217). Dr. Stone has received personal fees from Terumo, Cook, TherOx, Reva, Vascular Dynamics, Robocath, HeartFlow, Gore, Ablative Solutions, Matrizyme, Miracor, Neovasc, V-wave, Abiomed, Shockwave, MAIA Pharmaceuticals, and Vectorious; has received equity/options in Applied Therapeutics, Biostar, MedFocus, Aria, Cardiac Success, and Cagent; and has received personal fees and equity/options from SpectraWave, Valfix, Ancora, Orchestra Biomed, Qool Therapeutics, and Cardiomech. All other authors have reported that they have no relationships relevant to the contents of this paper to disclose.
Figures
References
-
- Kwong J.C., Schwartz K.L., Campitelli M.A. Acute myocardial infarction after laboratory-confirmed influenza infection. N Engl J Med. 2018;378:2540–2541. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

