Saliva RNA biomarkers predict concussion duration and detect symptom recovery: a comparison with balance and cognitive testing
- PMID: 34028616
- PMCID: PMC8505318
- DOI: 10.1007/s00415-021-10566-x
Saliva RNA biomarkers predict concussion duration and detect symptom recovery: a comparison with balance and cognitive testing
Abstract
Objective: The goals of this study were to assess the ability of salivary non-coding RNA (ncRNA) levels to predict post-concussion symptoms lasting ≥ 21 days, and to examine the ability of ncRNAs to identify recovery compared to cognition and balance.
Methods: RNA sequencing was performed on 505 saliva samples obtained longitudinally from 112 individuals (8-24-years-old) with mild traumatic brain injury (mTBI). Initial samples were obtained ≤ 14 days post-injury, and follow-up samples were obtained ≥ 21 days post-injury. Computerized balance and cognitive test performance were assessed at initial and follow-up time-points. Machine learning was used to define: (1) a model employing initial ncRNA levels to predict persistent post-concussion symptoms (PPCS) ≥ 21 days post-injury; and (2) a model employing follow-up ncRNA levels to identify symptom recovery. Performance of the models was compared against a validated clinical prediction rule, and balance/cognitive test performance, respectively.
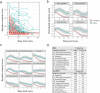
Results: An algorithm using age and 16 ncRNAs predicted PPCS with greater accuracy than the validated clinical tool and demonstrated additive combined utility (area under the curve (AUC) 0.86; 95% CI 0.84-0.88). Initial balance and cognitive test performance did not differ between PPCS and non-PPCS groups (p > 0.05). Follow-up balance and cognitive test performance identified symptom recovery with similar accuracy to a model using 11 ncRNAs and age. A combined model (ncRNAs, balance, cognition) most accurately identified recovery (AUC 0.86; 95% CI 0.83-0.89).
Conclusions: ncRNA biomarkers show promise for tracking recovery from mTBI, and for predicting who will have prolonged symptoms. They could provide accurate expectations for recovery, stratify need for intervention, and guide safe return-to-activities.
Keywords: mTBI; microRNA; prognosis; return to play; spit; traumatic brain injury.
© 2021. The Author(s).
Conflict of interest statement
SDH serves as a consultant for Quadrant Biosciences. SDH and FAM are scientific advisory board members for Quadrant Biosciences and are named as a co-inventors on intellectual property related to saliva RNA biomarkers in concussion that are patented by The Penn State College of Medicine and The SUNY Upstate Research Foundation and licensed to Quadrant Biosciences. SDV, GF, AR, and JR are paid employees of Quadrant Biosciences. RM has received funding from the NFL foundation. The other authors have no conflicts of interest to declare.
Figures



Similar articles
-
Diagnosing mild traumatic brain injury using saliva RNA compared to cognitive and balance testing.Clin Transl Med. 2020 Oct;10(6):e197. doi: 10.1002/ctm2.197. Clin Transl Med. 2020. PMID: 33135344 Free PMC article.
-
American Medical Society for Sports Medicine position statement: concussion in sport.Br J Sports Med. 2013 Jan;47(1):15-26. doi: 10.1136/bjsports-2012-091941. Br J Sports Med. 2013. PMID: 23243113 Review.
-
The diagnostic and prognostic utility of the dual-task tandem gait test for pediatric concussion.J Sport Health Sci. 2021 Mar;10(2):131-137. doi: 10.1016/j.jshs.2020.08.005. Epub 2020 Aug 12. J Sport Health Sci. 2021. PMID: 32795624 Free PMC article.
-
Multiple Object Tracking Scores Predict Post-Concussion Status Years after Mild Traumatic Brain Injury.J Neurotrauma. 2020 Aug 15;37(16):1777-1787. doi: 10.1089/neu.2019.6842. Epub 2020 Apr 17. J Neurotrauma. 2020. PMID: 31950862
-
Clinical test instrument development to identify and track recovery from concussion.Semin Speech Lang. 2014 Aug;35(3):173-85. doi: 10.1055/s-0034-1384679. Epub 2014 Aug 12. Semin Speech Lang. 2014. PMID: 25116211 Review.
Cited by
-
Tailored Anti-miR Decorated Covalent Organic Framework Enables Electrochemical Detection of Salivary miRNAs for Mild Traumatic Brain Injury.Small. 2025 Apr;21(14):e2412107. doi: 10.1002/smll.202412107. Epub 2025 Feb 17. Small. 2025. PMID: 39961046 Free PMC article.
-
Systematic Review of the Diagnostic and Clinical Utility of Salivary microRNAs in Traumatic Brain Injury (TBI).Int J Mol Sci. 2022 Oct 29;23(21):13160. doi: 10.3390/ijms232113160. Int J Mol Sci. 2022. PMID: 36361944 Free PMC article.
-
Review on the Role of Salivary Biomarkers in the Diagnosis of Mild Traumatic Brain Injury and Post-Concussion Syndrome.Diagnostics (Basel). 2023 Apr 7;13(8):1367. doi: 10.3390/diagnostics13081367. Diagnostics (Basel). 2023. PMID: 37189468 Free PMC article. Review.
-
Defining Biological Phenotypes of Mild Traumatic Brain Injury Using Saliva MicroRNA Profiles.J Neurotrauma. 2022 Jul;39(13-14):923-934. doi: 10.1089/neu.2022.0018. Epub 2022 May 9. J Neurotrauma. 2022. PMID: 35412857 Free PMC article.
-
Selecting outcome measures to validate prognostic biomarkers of paediatric mild traumatic brain injury: challenges and priorities.Front Neurol. 2025 Jul 17;16:1620178. doi: 10.3389/fneur.2025.1620178. eCollection 2025. Front Neurol. 2025. PMID: 40746647 Free PMC article.
References
-
- Lumba-Brown A, Yeates KO, Sarmiento K, Breiding MJ, Haegerich TM, Gioia GA, Turner M, Benzel EC, Suskauer SJ, Giza CC. Centers for Disease Control and Prevention guideline on the diagnosis and management of mild traumatic brain injury among children. JAMA Pediatr. 2018;172:e182853–e182853. doi: 10.1001/jamapediatrics.2018.2853. - DOI - PMC - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

