Severe injury to the brachial neurovascular bundle and muscles due to a horse bite: a case report
- PMID: 34030734
- PMCID: PMC8145829
- DOI: 10.1186/s13256-021-02863-w
Severe injury to the brachial neurovascular bundle and muscles due to a horse bite: a case report
Abstract
Introduction: Only a small portion of horse injuries are related to horse bites. In the majority of these occurrences, injuries are minor and self-treated. However, in some cases, the injury may be destructive and limb- and life-threatening. In these instances, the patient requires complex surgery and compound perioperative care.
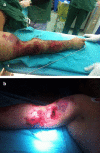
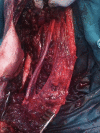
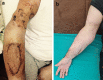
Case report: We present the case of a 35-year-old Albanian male farm-worker in whom a horse bite caused an extensive lacero-contusive and avulsive wound to the arm. The wound resulted in injury to the brachial artery, brachial and basilic vein, and biceps and brachialis muscles. Nerve structures and underlying humerus remained intact. The initial management of the severe hemorrhagic shock caused by the bleeding at the site of injury included reconstruction of the brachial artery by interposing saphenous graft and that of the brachial vein by termino-terminal anastomosis. Basilic vein was ligated. The wound was extensively debrided, and after a drain was placed in the wound, biceps and brachialis muscles were reconstructed. The patient received several units of red blood cells and fresh frozen plasma before and after surgery, as well as antibiotic, antitetanic, and antirabies prophylaxes. He had several consecutive necrectomies in the following days. However, due to postoperative sepsis and hemorrhagic shock at time of admission, the patient developed acute renal failure, therefore requiring several hemodialysis sessions. After his general and local condition was stabilized, the patient also underwent several reconstructive surgeries.
Conclusion: Horse bites of large extent require a multidisciplinary approach. The composition of the team of physicians needed for treatment varies depending on the degree of the injury and eventual complications. In the case of our patient, emergency department physicians, vascular and plastic surgeons, intensive care specialists, nephrologists, and infective care specialists were involved. In different instances, the inclusion of other specialists may be necessary to save and functionalize the limbs of the patient, or save his/her life.
Keywords: Arterial injury; Hemodialysis; Horse bite; Sepsis.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

Similar articles
-
Arterial Injury in the Upper Limb Resulting from Dog Bite.Ann Vasc Surg. 2018 May;49:314.e5-314.e10. doi: 10.1016/j.avsg.2017.11.053. Epub 2018 Feb 23. Ann Vasc Surg. 2018. PMID: 29481925 Review.
-
Delayed brachial artery occlusion owing to a dog bite of the upper extremity.Pediatr Emerg Care. 1990 Dec;6(4):293-5. doi: 10.1097/00006565-199012000-00011. Pediatr Emerg Care. 1990. PMID: 2290729
-
Management of vascular trauma from dog bites.J Vasc Surg. 2013 Nov;58(5):1346-52. doi: 10.1016/j.jvs.2013.05.101. Epub 2013 Jul 24. J Vasc Surg. 2013. PMID: 23891489
-
Brachial Artery Injury Resulting From a Dog Bite in a Pediatric Patient: A Case Report.Cureus. 2023 Sep 25;15(9):e45889. doi: 10.7759/cureus.45889. eCollection 2023 Sep. Cureus. 2023. PMID: 37885488 Free PMC article.
-
Carotido-brachial artery bypass for radiation induced injury of the subclavian artery. The value of a lateral mid-arm approach.J Cardiovasc Surg (Torino). 1994 Aug;35(4):321-4. J Cardiovasc Surg (Torino). 1994. PMID: 7929544 Review.
References
-
- Dendle C, Looke D. Animal bites: an update for management with a focus on infections. Emerg Med Australas. 2008;20(6):458–467. - PubMed
-
- Emet M, Beyhun NE, Kosan Z, Aslan S, Uzkeser M, Cakir ZG. Animal-related injuries: epidemiological and meteorogical features. Ann Agric Environ Med. 2009;16(1):87–92. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

