Recurrent urinary tract infection: Association of clinical profiles with urobiome composition in women
- PMID: 34036621
- PMCID: PMC8298270
- DOI: 10.1002/nau.24707
Recurrent urinary tract infection: Association of clinical profiles with urobiome composition in women
Abstract
Aims: Clinical profiles of women with recurrent urinary tract infection (RUTI) are correlated with their urinary microbes.
Methods: This IRB-approved, cross-sectional study enrolled adult women with RUTI. Urine samples (catheterized and voided) underwent culture by expanded quantitative urine culture (EQUC) and standard urine culture (SUC) methods. A validated symptom questionnaire, relevant clinical variables, and EQUC were used to identify symptom clusters and detect associations with specific urinary microbes.
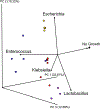
Results: Most (36/43) participants were postmenopausal; the average age was 67 years. 51% reported vaginal estrogen use; 51% reported sexual activity. Although single symptoms were not associated with specific urinary microbes, EQUC results were correlated with five distinct clinical profile clusters: Group A: odor, cloudiness, and current vaginal estrogen use (no culture result association). Group B: frequency, low back pain, incomplete emptying, and vaginal estrogen (significantly increased proportion of Lactobacillus-positive cultures). Group C: pain/burning, odor, cloudiness, and urgency (high proportions of UTI-associated microbe-positive cultures). Group D: frequency, urgency, pain/burning, and current vaginal estrogen use (increased number of no growth cultures). Group E: frequency, urgency, pain/burning, odor, overactive bladder, and sexually active (significantly increased proportion of Klebsiella-positive cultures).
Conclusions: Distinct clinical profiles are associated with specific urinary microbes in women with RUTI. Refined assessments of clinical profiles may provide useful insights that could inform diagnostic and therapeutic considerations.
Keywords: enhanced urine culture; recurrent urinary tract infection; symptomatology; urinary microbiome; urinary microbiota.
© 2021 Wiley Periodicals LLC.
Figures

References
-
- Foxman B Epidemiology of urinary tract infections: incidence, morbidity, and economic costs. Am J Med. 2002;113 Suppl 1A:5S–13S. - PubMed
-
- No Time to Wait: Securing the future from drug-resistant infections. World Health Organization; April 2019.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

