Evaluation of splenic accumulation and colocalization of immature reticulocytes and Plasmodium vivax in asymptomatic malaria: A prospective human splenectomy study
- PMID: 34038413
- PMCID: PMC8154101
- DOI: 10.1371/journal.pmed.1003632
Evaluation of splenic accumulation and colocalization of immature reticulocytes and Plasmodium vivax in asymptomatic malaria: A prospective human splenectomy study
Abstract
Background: A very large biomass of intact asexual-stage malaria parasites accumulates in the spleen of asymptomatic human individuals infected with Plasmodium vivax. The mechanisms underlying this intense tropism are not clear. We hypothesised that immature reticulocytes, in which P. vivax develops, may display high densities in the spleen, thereby providing a niche for parasite survival.
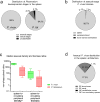
Methods and findings: We examined spleen tissue in 22 mostly untreated individuals naturally exposed to P. vivax and Plasmodium falciparum undergoing splenectomy for any clinical indication in malaria-endemic Papua, Indonesia (2015 to 2017). Infection, parasite and immature reticulocyte density, and splenic distribution were analysed by optical microscopy, flow cytometry, and molecular assays. Nine non-endemic control spleens from individuals undergoing spleno-pancreatectomy in France (2017 to 2020) were also examined for reticulocyte densities. There were no exclusion criteria or sample size considerations in both patient cohorts for this demanding approach. In Indonesia, 95.5% (21/22) of splenectomy patients had asymptomatic splenic Plasmodium infection (7 P. vivax, 13 P. falciparum, and 1 mixed infection). Significant splenic accumulation of immature CD71 intermediate- and high-expressing reticulocytes was seen, with concentrations 11 times greater than in peripheral blood. Accordingly, in France, reticulocyte concentrations in the splenic effluent were higher than in peripheral blood. Greater rigidity of reticulocytes in splenic than in peripheral blood, and their higher densities in splenic cords both suggest a mechanical retention process. Asexual-stage P. vivax-infected erythrocytes of all developmental stages accumulated in the spleen, with non-phagocytosed parasite densities 3,590 times (IQR: 2,600 to 4,130) higher than in circulating blood, and median total splenic parasite loads 81 (IQR: 14 to 205) times greater, accounting for 98.7% (IQR: 95.1% to 98.9%) of the estimated total-body P. vivax biomass. More reticulocytes were in contact with sinus lumen endothelial cells in P. vivax- than in P. falciparum-infected spleens. Histological analyses revealed 96% of P. vivax rings/trophozoites and 46% of schizonts colocalised with 92% of immature reticulocytes in the cords and sinus lumens of the red pulp. Larger splenic cohort studies and similar investigations in untreated symptomatic malaria are warranted.
Conclusions: Immature CD71+ reticulocytes and splenic P. vivax-infected erythrocytes of all asexual stages accumulate in the same splenic compartments, suggesting the existence of a cryptic endosplenic lifecycle in chronic P. vivax infection. Findings provide insight into P. vivax-specific adaptions that have evolved to maximise survival and replication in the spleen.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures




References
-
- WHO. World Malaria Report 2020. Geneva: World Health Organisation, 2020.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

