Double-balloon endoscopic retrograde cholangiography can make a reliable diagnosis and good prognosis for postoperative complications of congenital biliary dilatation
- PMID: 34040119
- PMCID: PMC8155203
- DOI: 10.1038/s41598-021-90550-7
Double-balloon endoscopic retrograde cholangiography can make a reliable diagnosis and good prognosis for postoperative complications of congenital biliary dilatation
Abstract
Bile duct and anastomotic strictures and intrahepatic stones are common postoperative complications of congenital biliary dilatation (CBD). We performed double-balloon endoscopic retrograde cholangiography (DBERC) for diagnostic and therapeutic purposes after radical surgery. We focused on the effectiveness of DBERC for the treatment of postoperative complications of CBD patients. Bile duct and anastomotic strictures and intrahepatic stones are common postoperative complications of congenital biliary dilatation (CBD). We performed double-balloon endoscopic retrograde cholangiography (DBERC) for diagnostic and therapeutic purposes after radical surgery. We focused on the effectiveness of DBERC for the treatment of postoperative complications of CBD patients. This retrospective study included 28 patients who underwent DBERC (44 procedures) after radical surgery for CBD between January 2011 and December 2019. Strictures were diagnosed as "bile duct strictures" if endoscopy confirmed the presence of bile duct mucosa between the stenotic and anastomotic regions, and as "anastomotic strictures" if the mucosa was absent. The median patient age was 4 (range 0-67) years at the time of primary surgery for CBD and 27.5 (range 8-76) years at the time of DBERC. All anastomotic strictures could be treated with only by 1-2 courses of balloon dilatation of DBERC, while many bile duct strictures (41.2%) needed ≥ 3 treatments, especially those who underwent operative bile duct plasty as the first treatment (83.3%). Although the study was limited by the short follow-up period after DBERC treatment, DBERC is recommended as the first-line treatment for hepatolithiasis associated with biliary and anastomotic strictures in CBD patients, and it can be safely performed multiple times.
Conflict of interest statement
The authors declare no competing interests.
Figures
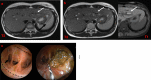

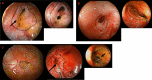
Similar articles
-
Late postoperative complications of congenital biliary dilatation in pediatric patients: a single-center experience of managing complications for over 20 years.Surg Today. 2021 Sep;51(9):1488-1495. doi: 10.1007/s00595-021-02238-0. Epub 2021 Mar 10. Surg Today. 2021. PMID: 33689035
-
Laparoscopic closure of Roux limb perforation during double-balloon endoscopic retrograde cholangiography with laparoscopy-assisted endoscopic hepatolithectomy 30 years after congenital biliary dilatation radical surgery: A case report.Asian J Endosc Surg. 2023 Jan;16(1):118-122. doi: 10.1111/ases.13116. Epub 2022 Aug 11. Asian J Endosc Surg. 2023. PMID: 35957492
-
Factors affecting complete stone removal and bile duct stone recurrence in patients with surgically altered anatomy treated by double-balloon endoscopy-assisted endoscopic retrograde cholangiography.Dig Endosc. 2024 Nov;36(11):1269-1279. doi: 10.1111/den.14824. Epub 2024 Jun 25. Dig Endosc. 2024. PMID: 38923022
-
Postoperative bile duct strictures.Surg Clin North Am. 1990 Dec;70(6):1355-80. doi: 10.1016/s0039-6109(16)45289-8. Surg Clin North Am. 1990. PMID: 2247820 Review.
-
Endoscopic retrograde cholangiography for biliary anastomotic strictures after liver transplantation.Clin Liver Dis. 2014 Nov;18(4):913-26. doi: 10.1016/j.cld.2014.07.009. Epub 2014 Aug 22. Clin Liver Dis. 2014. PMID: 25438291 Review.
Cited by
-
Current treatment strategies for postoperative intrahepatic bile duct stones in congenital biliary dilatation: a single center retrospective study.BMC Pediatr. 2022 Dec 3;22(1):695. doi: 10.1186/s12887-022-03759-4. BMC Pediatr. 2022. PMID: 36463156 Free PMC article.
-
Global research trends in surgical management of choledochal cysts: a bibliometric analysis from 2000 to 2024.Front Med (Lausanne). 2025 Jul 11;12:1611045. doi: 10.3389/fmed.2025.1611045. eCollection 2025. Front Med (Lausanne). 2025. PMID: 40718413 Free PMC article.
-
Presentation and outcomes of surgery for choledochal cyst in children and adults: an experience of 329 cases.Updates Surg. 2025 Apr;77(2):459-470. doi: 10.1007/s13304-025-02138-9. Epub 2025 Mar 4. Updates Surg. 2025. PMID: 40035920
-
Risk factors for postoperative stone formation in pediatric choledochal cysts: a study of 457 cases.Sci Rep. 2025 Mar 18;15(1):9235. doi: 10.1038/s41598-025-94308-3. Sci Rep. 2025. PMID: 40097690 Free PMC article.
-
Non-cirrhotic portal hypertension secondary to cholangiointestinal anastomotic stricture after choledochal cyst excision: a case report.Front Med (Lausanne). 2023 May 23;10:1149484. doi: 10.3389/fmed.2023.1149484. eCollection 2023. Front Med (Lausanne). 2023. PMID: 37287745 Free PMC article.
References
-
- Urushihara N, Fukumoto K, Fukuzawa H, Mitsunaga M, Watanabe K, Aoba T, Yamoto M, Miyake H. Long-term outcomes after excision of choledochal cysts in a single institution: operative procedures and late complications. J. Pediatr. Surg. 2012;47:2169–2174. doi: 10.1016/j.jpedsurg.2012.09.001. - DOI - PubMed
-
- Mukai M, Kaji T, Masuya R, Yamada K, Sugita K, Moriguchi T, Onishi S, Yamada W, Kawano T, Machigashira S, Nakame K, Takamatsu H, Leiri S. Long-term outcomes of surgery for choledochal cysts: a single-institution study focusing on follow-up and late complications. Surg. Today. 2018;48:835–840. doi: 10.1007/s00595-018-1660-9. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

