Hepatic sclerosed hemangioma and sclerosing cavernous hemangioma: a radiological study
- PMID: 34041675
- PMCID: PMC8568860
- DOI: 10.1007/s11604-021-01139-z
Hepatic sclerosed hemangioma and sclerosing cavernous hemangioma: a radiological study
Abstract
Purpose: To investigate and compare the CT and MRI features of hepatic sclerosed hemangioma (HSH) and sclerosing cavernous hemangioma (SCH).
Materials and methods: Twelve HSH cases and 36 SCH cases were included, the imaging findings on CT (9 HSH and 34 SCH) and MRI (8 HSH and 10 SCH) were analyzed. Qualitative image analysis included the location, size, shape, capsular retraction, density, calcification, signal intensity on T1-weighted image (T1WI) and T2-weighted image (T2WI), presence of diffusion restriction, apparent diffusion coefficient (ADC) map, transient hepatic attenuation difference around the lesion, and the dynamic enhancement patterns.
Results: The presence of liver cirrhosis in patients with HSH (3/12) was higher than SCH (1/36) (P = 0.043). The morphology appearance before enhancement showed no significant difference between HSH and SCH. Moreover, SCH had a stronger trend of centripetal enhancement patterns of cavernous hemangiomas (83.3%) compared to HSH (25%) (P < 0.001). Due to more frequent atypical enhancement features, containing rim-like enhancement, no enhancement, and peripheral heterogeneous enhancement, the misdiagnosis rate of HSH (75%) was significantly higher than that of SCH (16.7%) (P < 0.001). Furthermore, the ADC values of HSH and SCH were both higher than that of the surrounding liver parenchyma (P = 0.009, P = 0.002); however, there was no significant difference in ADC values between themselves (P = 0.613).
Conclusion: SCH showed the same trend of centripetal enhancement characteristics as typical hemangioma, while HSH exhibited atypical enhancement features due to complete sclerosis. Higher ADC values might contribute to the identification of atypical HSH and SCH from malignancies.
Keywords: Computed tomography; Diagnosis; Hepatic sclerosed hemangioma; Magnetic resonance imaging; Sclerosing cavernous hemangioma.
© 2021. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures

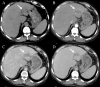
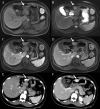




Similar articles
-
Differentiation of Hepatic Sclerosed Hemangiomas From Cavernous Hemangiomas Based on Gadoxetic Acid-Enhanced Magnetic Resonance Imaging Features.J Comput Assist Tomogr. 2019 Sep/Oct;43(5):762-769. doi: 10.1097/RCT.0000000000000905. J Comput Assist Tomogr. 2019. PMID: 31356526
-
Hepatic sclerosed hemangioma with special attention to diffusion-weighted magnetic resonance imaging.Surg Case Rep. 2018 Jan 3;4(1):3. doi: 10.1186/s40792-017-0414-z. Surg Case Rep. 2018. PMID: 29299708 Free PMC article.
-
Computed tomography and magnetic resonance imaging findings of nasal cavity hemangiomas according to histological type.Korean J Radiol. 2015 May-Jun;16(3):566-74. doi: 10.3348/kjr.2015.16.3.566. Epub 2015 May 13. Korean J Radiol. 2015. PMID: 25995686 Free PMC article.
-
Hepatic Sclerosed Hemangioma: a case report and review of the literature.BMC Surg. 2015 Apr 17;15:45. doi: 10.1186/s12893-015-0029-x. BMC Surg. 2015. PMID: 25927893 Free PMC article. Review.
-
The humbling hemangioma: uncommon CT and MRI imaging features and mimickers of hepatic hemangiomas.Clin Imaging. 2021 Jun;74:55-63. doi: 10.1016/j.clinimag.2020.12.028. Epub 2021 Jan 5. Clin Imaging. 2021. PMID: 33434867 Review.
Cited by
-
Diagnostic Pitfalls of Hepatic Sclerosed Hemangiomas: A Case Report.Cureus. 2025 Mar 17;17(3):e80738. doi: 10.7759/cureus.80738. eCollection 2025 Mar. Cureus. 2025. PMID: 40248561 Free PMC article.
-
Solitary hypovascular hepatic nodules: comparison and differentiation between peripheral nodular cholangiocarcinoma and atypical liver hemangioma with MRI.Transl Cancer Res. 2023 Sep 30;12(9):2308-2318. doi: 10.21037/tcr-23-27. Epub 2023 Aug 25. Transl Cancer Res. 2023. PMID: 37859741 Free PMC article.
-
Current State of Artificial Intelligence in Clinical Applications for Head and Neck MR Imaging.Magn Reson Med Sci. 2023 Oct 1;22(4):401-414. doi: 10.2463/mrms.rev.2023-0047. Epub 2023 Aug 1. Magn Reson Med Sci. 2023. PMID: 37532584 Free PMC article. Review.
-
Hepatic sclerosing haemangioma showing restricted diffusion: A case report with histopathologic correlation.BJR Case Rep. 2022 May 12;8(4):20220029. doi: 10.1259/bjrcr.20220029. eCollection 2022 Jul 1. BJR Case Rep. 2022. PMID: 36451903 Free PMC article.
-
Multiple sclerosing hemangiomas mimicking hepatocellular carcinoma: A case report.Int J Immunopathol Pharmacol. 2023 Jan-Dec;37:3946320231190898. doi: 10.1177/03946320231190898. Int J Immunopathol Pharmacol. 2023. PMID: 37614092 Free PMC article.
References
MeSH terms
Grants and funding
- No. 81771806/National Natural Science Foundation of China
- 61936013/National Natural Science Foundation of China
- No. BMU2018MX027/Peking University Medicine Seed Fund for Interdisciplinary Research
- No. YNKTTS20180130/Project of Incubating Young and Middle-aged Talents
- No. PYZ2017124/Capital Medical University Research and Incubation Funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

