Prognostic Nomogram for patients undergoing radical Pancreaticoduodenectomy for adenocarcinoma of the pancreatic head
- PMID: 34044806
- PMCID: PMC8161963
- DOI: 10.1186/s12885-021-08295-5
Prognostic Nomogram for patients undergoing radical Pancreaticoduodenectomy for adenocarcinoma of the pancreatic head
Abstract
Background: Radical pancreaticoduodenectomy is the most common treatment strategy for patients diagnosed with adenocarcinoma of the pancreatic head. Few studies have reported the clinical characteristics and treatment efficacies of patients undergoing radical pancreaticoduodenectomy for adenocarcinoma of the pancreatic head.
Methods: A total of 177 pancreatic head cancer patients who underwent radical pancreaticoduodenectomy and were pathologically confirmed as having pancreatic ductal adenocarcinoma were screened in the West China Hospital of Sichuan University. The multivariate analysis results were implemented to construct a nomogram. The concordance index (c-index), the area under the curve (AUC) and calibration were utilized to evaluate the predictive performance of the nomogram.
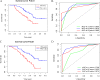
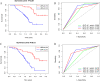
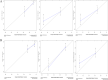
Results: The prognostic nutritional index (PNI), the lymph node ratio (LNR) and the American Joint Committee on Cancer (AJCC) staging served as independent prognostic factors and were used to construct the nomogram. The c-indexes of the nomogram were 0.799 (confidence interval (CI), 0.741-0.858) and 0.732 (0.657-0.807) in the primary set and validation set, respectively. The AUCs of the nomogram at 1 and 3 years were 0.832 and 0.783, which were superior to the AJCC staging values of 0.759 and 0.705, respectively.
Conclusions: The nomogram may be used to predict the prognosis of radical resection for adenocarcinoma of the pancreatic head. These findings may represent an effective model for the developing an optimal therapeutic schedule for malnourished patients who need early effective nutritional intervention and may promote the treatment efficacy of resectable adenocarcinoma of the pancreatic head.
Keywords: Adenocarcinoma of the pancreatic head; Nomogram; Pancreaticoduodenectomy; Prognostic.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures



References
-
- Elshaer M, Gravante G, Kosmin M, Riaz A, Al-Bahrani A. A systematic review of the prognostic value of lymph node ratio, number of positive nodes and total nodes examined in pancreatic ductal adenocarcinoma. Ann R Coll Surg Engl. 2017;99(2):101–106. doi: 10.1308/rcsann.2016.0340. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

