Histopathological Growth Patterns and Survival After Resection of Colorectal Liver Metastasis: An External Validation Study
- PMID: 34056541
- PMCID: PMC8152695
- DOI: 10.1093/jncics/pkab026
Histopathological Growth Patterns and Survival After Resection of Colorectal Liver Metastasis: An External Validation Study
Abstract
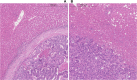
Background: After resection of colorectal cancer liver metastases (CRLM), 2 main histopathological growth patterns can be observed: a desmoplastic and a nondesmoplastic subtype. The desmoplastic subtype has been associated with superior survival. These findings require external validation.
Methods: An international multicenter retrospective cohort study was conducted in patients treated surgically for CRLM at 3 tertiary hospitals in the United States and the Netherlands. Determination of histopathological growth patterns was performed on hematoxylin and eosin-stained sections of resected CRLM according to international guidelines. Patients displaying a desmoplastic histopathological phenotype (only desmoplastic growth observed) were compared with patients with a nondesmoplastic phenotype (any nondesmoplastic growth observed). Cutoff analyses on the extent of nondesmoplastic growth were performed. Overall survival (OS) and disease-free survival (DFS) were estimated using Kaplan-Meier and multivariable Cox analysis. All statistical tests were 2-sided.
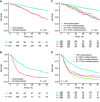
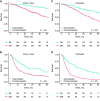
Results: In total 780 patients were eligible. A desmoplastic phenotype was observed in 19.1% and was associated with microsatellite instability (14.6% vs 3.6%, P = .01). Desmoplastic patients had superior 5-year OS (73.4%, 95% confidence interval [CI] = 64.1% to 84.0% vs 44.2%, 95% CI = 38.9% to 50.2%, P < .001) and DFS (32.0%, 95% CI = 22.9% to 44.7% vs 14.7%, 95% CI = 11.7% to 18.6%, P < .001) compared with their nondesmoplastic counterparts. A desmoplastic phenotype was associated with an adjusted hazard ratio for death of 0.36 (95% CI = 0.23 to 0.58) and 0.50 (95% CI = 0.37 to 0.66) for cancer recurrence. Prognosis was independent of KRAS and BRAF status. The cutoff analyses found no prognostic relationship between either OS or DFS and the extent of nondesmoplastic growth observed (all P > .1).
Conclusions: This external validation study confirms the remarkably good prognosis after surgery for CRLM in patients with a desmoplastic phenotype. The extent of nondesmoplastic growth does not affect prognosis.
© The Author(s) 2021. Published by Oxford University Press.
Figures
References
-
- Vermeulen PB, Colpaert C, Salgado R, et al.Liver metastases from colorectal adenocarcinomas grow in three patterns with different angiogenesis and desmoplasia. J Pathol. 2001;195(3):336–342. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous
