Psychological symptoms during and after Austrian first lockdown in individuals with bipolar disorder? A follow-up control-group investigation
- PMID: 34059980
- PMCID: PMC8166528
- DOI: 10.1186/s40345-021-00222-8
Psychological symptoms during and after Austrian first lockdown in individuals with bipolar disorder? A follow-up control-group investigation
Abstract
Background: The coronavirus disease (COVID-19) pandemic, a global health crisis, has resulted in widespread socioeconomic restrictions including lockdown, social distancing, and self-isolation. To date, little is known about the psychological impact of the COVID-19 pandemic and lockdown on patients with bipolar disorder as a particularly vulnerable group.
Methods: An online survey was conducted in Austria at two points of measurement (T1 April 2020 during the first lockdown vs. T2 May 2020 at post-lockdown). The sample comprises 20 patients with bipolar disorder (mean age = 49.4 ± 15.6 years) and 20 healthy controls (mean age = 32.7 ± 9.6 years). A 2 × 2 factorial design to compare two time points (T1 vs. T2) and two groups (patients vs. healthy controls) was used. Main outcome measures included the Brief Symptom Inventory-18 (BSI-18) and a (non-validated and non-standardized) assessment to determine COVID-19 fears and emotional distress due to social distancing. Multiple linear regression analyses were used to assess the longitudinal association of COVID-19 fears/emotional distress due to social distancing during lockdown (T1) and psychological symptoms after lockdown (T2).
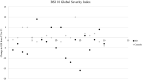
Results: At T1, results demonstrated higher scores in BSI-18 subscales depression, anxiety and global severity index as well as emotional distress due to social distancing in bipolar patients compared to controls. There was a significant time x group interaction in the BSI-18 subscale somatization showing a decreasing trend in patients with BD compared to controls. No time effects in BSI-18 subscales or COVID-19 fears/emotional distress due to social distancing were observed. Regression analyses showed that COVID-19 fears during lockdown predicted somatization, only in patients.
Conclusions: There was a connection between the lockdown measures and somatization symptoms observed in patients. When the first steps of easing the social restrictions in May 2020 took place, somatization decreased only in the bipolar compared to the control group. Higher COVID-19 fears during lockdown predicted later symptoms at post-lockdown. Long-term impacts of the COVID-19 pandemic need further investigations to improve current therapeutic approaches and prevent fears and distress during lockdown in individuals with bipolar disorder in times of crisis.
Keywords: Anxiety; Bipolar disorder; COVID-19; Depression; Global symptom load; Lockdown; Somatization.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures


Similar articles
-
Psychological and behavioral response on the COVID-19 pandemic in individuals with bipolar disorder: A multicenter study.Psychiatry Res. 2022 Apr;310:114451. doi: 10.1016/j.psychres.2022.114451. Epub 2022 Feb 16. Psychiatry Res. 2022. PMID: 35190338 Free PMC article.
-
Greater Emotional Distress Due to Social Distancing and Greater Symptom Severity during the COVID-19 Pandemic in Individuals with Bipolar Disorder: A Multicenter Study in Austria, Germany, and Denmark.Int J Environ Res Public Health. 2022 Jun 22;19(13):7626. doi: 10.3390/ijerph19137626. Int J Environ Res Public Health. 2022. PMID: 35805284 Free PMC article.
-
COVID-19 Pandemic Stress-Induced Somatization in Transplant Waiting List Patients.Front Psychiatry. 2021 Jul 6;12:671383. doi: 10.3389/fpsyt.2021.671383. eCollection 2021. Front Psychiatry. 2021. PMID: 34295270 Free PMC article.
-
Optimal strategies for COVID-19 prevention from global evidence achieved through social distancing, stay at home, travel restriction and lockdown: a systematic review.Arch Public Health. 2021 Aug 21;79(1):150. doi: 10.1186/s13690-021-00663-8. Arch Public Health. 2021. PMID: 34419145 Free PMC article. Review.
-
Aging, Social Distancing, and COVID-19 Risk: Who is more Vulnerable and Why?Aging Dis. 2021 Oct 1;12(7):1624-1643. doi: 10.14336/AD.2021.0319. eCollection 2021 Oct. Aging Dis. 2021. PMID: 34631211 Free PMC article. Review.
Cited by
-
Psychological and behavioral response on the COVID-19 pandemic in individuals with bipolar disorder: A multicenter study.Psychiatry Res. 2022 Apr;310:114451. doi: 10.1016/j.psychres.2022.114451. Epub 2022 Feb 16. Psychiatry Res. 2022. PMID: 35190338 Free PMC article.
-
Greater Emotional Distress Due to Social Distancing and Greater Symptom Severity during the COVID-19 Pandemic in Individuals with Bipolar Disorder: A Multicenter Study in Austria, Germany, and Denmark.Int J Environ Res Public Health. 2022 Jun 22;19(13):7626. doi: 10.3390/ijerph19137626. Int J Environ Res Public Health. 2022. PMID: 35805284 Free PMC article.
-
The global evolution of mental health problems during the COVID-19 pandemic: A systematic review and meta-analysis of longitudinal studies.J Affect Disord. 2022 Oct 15;315:70-95. doi: 10.1016/j.jad.2022.07.011. Epub 2022 Jul 14. J Affect Disord. 2022. PMID: 35842064 Free PMC article.
-
Decrease in Social Zeitgebers Is Associated With Worsened Delayed Sleep-Wake Phase Disorder: Findings During the Pandemic in Japan.Front Psychiatry. 2022 Jun 9;13:898600. doi: 10.3389/fpsyt.2022.898600. eCollection 2022. Front Psychiatry. 2022. PMID: 35757225 Free PMC article.
-
Mental Health in the Post-Lockdown Scenario: A Scientometric Investigation of the Main Thematic Trends of Research.Int J Environ Res Public Health. 2023 Jul 6;20(13):6310. doi: 10.3390/ijerph20136310. Int J Environ Res Public Health. 2023. PMID: 37444157 Free PMC article. Review.
References
-
- Barzilay R, Moore TM, Greenberg DM, DiDomenico GE, Brown LA, White LK, Gur RE. Resilience, COVID-19-related stress, anxiety and depression during the pandemic in a large population enriched for healthcare providers. Transl Psychiatry. 2020;10(1):1–8. doi: 10.1038/s41398-020-00982-4. - DOI - PMC - PubMed
-
- Bengesser S, Reininghaus E. Polygenic risk scores and bipolar disorder. J Psychiatry Brain Sci. 2018;3(6):1–11.
LinkOut - more resources
Full Text Sources
Miscellaneous

