Presepsin (Soluble CD14 Subtype) as an Early Marker of Neonatal Sepsis and Septic Shock: A Prospective Diagnostic Trial
- PMID: 34068959
- PMCID: PMC8156848
- DOI: 10.3390/antibiotics10050580
Presepsin (Soluble CD14 Subtype) as an Early Marker of Neonatal Sepsis and Septic Shock: A Prospective Diagnostic Trial
Abstract
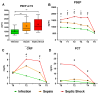
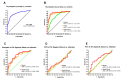
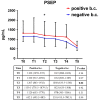
In the context of suspected neonatal sepsis, early diagnosis and stratification of patients according to clinical severity is not yet effectively achieved. In this diagnostic trial, we aimed to assess the accuracy of presepsin (PSEP) for the diagnosis and early stratification of supposedly septic neonates. PSEP, C-reactive protein (CRP), and procalcitonin (PCT) were assessed at the onset of sepsis suspicion (T0), every 12-24 h for the first 48 h (T1-T4), and at the end of antibiotic therapy (T5). Enrolled neonates were stratified into three groups (infection, sepsis, septic shock) according to Wynn and Wong's definitions. Sensitivity, specificity, and area under the ROC curve (AUC) according to the severity of clinical conditions were assessed. We enrolled 58 neonates with infection, 77 with sepsis, and 24 with septic shock. PSEP levels were higher in neonates with septic shock (median 1557.5 pg/mL) and sepsis (median 1361 pg/mL) compared to those with infection (median 977.5 pg/mL) at T0 (p < 0.01). Neither CRP nor PCT could distinguish the three groups at T0. PSEP's AUC was 0.90 (95% CI: 0.854-0.943) for sepsis and 0.94 (95% CI: 0.885-0.988) for septic shock. Maximum Youden index was 1013 pg/mL (84.4% sensitivity, 88% specificity) for sepsis, and 971.5 pg/mL for septic shock (92% sensitivity, 86% specificity). However, differences in PSEP between neonates with positive and negative blood culture were limited. Thus, PSEP was an early biomarker of neonatal sepsis severity, but did not support the early identification of neonates with positive blood culture.
Keywords: biomarkers; inflammation; neonatal sepsis; newborn; presepsin; septic shock.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
Similar articles
-
Presepsin: gelsolin ratio, as a promising marker of sepsis-related organ dysfunction: a prospective observational study.Front Med (Lausanne). 2023 May 5;10:1126982. doi: 10.3389/fmed.2023.1126982. eCollection 2023. Front Med (Lausanne). 2023. PMID: 37215727 Free PMC article.
-
Soluble CD14 subtype (sCD14-ST) presepsin in premature and full term critically ill newborns with sepsis and SIRS.Clin Chim Acta. 2015 Dec 7;451(Pt A):65-70. doi: 10.1016/j.cca.2015.07.025. Epub 2015 Jul 29. Clin Chim Acta. 2015. PMID: 26232159
-
Role of procalcitonin, C-reactive protein, interleukin-6, interleukin-8 and tumor necrosis factor-alpha in the diagnosis of neonatal sepsis.Turk J Pediatr. 2007 Jan-Mar;49(1):7-20. Turk J Pediatr. 2007. PMID: 17479639
-
The combination of procalcitonin and C-reactive protein or presepsin alone improves the accuracy of diagnosis of neonatal sepsis: a meta-analysis and systematic review.Crit Care. 2018 Nov 21;22(1):316. doi: 10.1186/s13054-018-2236-1. Crit Care. 2018. PMID: 30463590 Free PMC article.
-
Presepsin as a diagnostic marker of sepsis in children and adolescents: a systemic review and meta-analysis.BMC Infect Dis. 2019 Aug 30;19(1):760. doi: 10.1186/s12879-019-4397-1. BMC Infect Dis. 2019. PMID: 31470804 Free PMC article.
Cited by
-
The Emerging Role of Presepsin (P-SEP) in the Diagnosis of Sepsis in the Critically Ill Infant: A Literature Review.Int J Mol Sci. 2021 Nov 10;22(22):12154. doi: 10.3390/ijms222212154. Int J Mol Sci. 2021. PMID: 34830040 Free PMC article. Review.
-
Variations in Antibiotic Use and Sepsis Management in Neonatal Intensive Care Units: A European Survey.Antibiotics (Basel). 2021 Aug 27;10(9):1046. doi: 10.3390/antibiotics10091046. Antibiotics (Basel). 2021. PMID: 34572631 Free PMC article.
-
Biomarkers of Neonatal Sepsis: Where We Are and Where We Are Going.Antibiotics (Basel). 2023 Jul 26;12(8):1233. doi: 10.3390/antibiotics12081233. Antibiotics (Basel). 2023. PMID: 37627653 Free PMC article. Review.
-
Can Presepsin Be Valuable in Reducing Unnecessary Antibiotic Exposure after Birth?Antibiotics (Basel). 2023 Apr 2;12(4):695. doi: 10.3390/antibiotics12040695. Antibiotics (Basel). 2023. PMID: 37107057 Free PMC article.
-
Stop in Time: How to Reduce Unnecessary Antibiotics in Newborns with Late-Onset Sepsis in Neonatal Intensive Care.Trop Med Infect Dis. 2024 Mar 19;9(3):63. doi: 10.3390/tropicalmed9030063. Trop Med Infect Dis. 2024. PMID: 38535886 Free PMC article. Review.
References
-
- Pugni L., Ronchi A., Bizzarri B., Consonni D., Pietrasanta C., Ghirardi B., Fumagalli M., Ghirardello S., Mosca F. Exchange Transfusion in the Treatment of Neonatal Septic Shock: A Ten-Year Experience in a Neonatal Intensive Care Unit. Int. J. Mol. Sci. 2016;17:695. doi: 10.3390/ijms17050695. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

