The Effect of Thyrotropin-Releasing Hormone and Antithyroid Drugs on Fetal Thyroid Function
- PMID: 34071168
- PMCID: PMC8228147
- DOI: 10.3390/children8060454
The Effect of Thyrotropin-Releasing Hormone and Antithyroid Drugs on Fetal Thyroid Function
Abstract
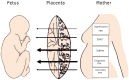
A euthyroid pregnant woman will normally have a fetus that displays normal fetal development. However, studies have long demonstrated the role of T3 (Triiodothyronine), T4 (Thyroxine), and TSH (Thyroid Stimulating Hormone) and their degree of penetrability into the fetal circulation. Maternal thyrotropin-releasing hormone (TRH) crosses the placental site and, from mid-gestation onward, is able to promote fetal TSH secretion. Its origin is not only hypothalamic, as was believed until recently. The maternal pancreas, and other extraneural and extrahypothalamic organs, can produce TRH variants, which are transported through the placenta affecting, to a degree, fetal thyroid function. Antithyroid drugs (ATDs) also cross the placenta and, because of their therapeutic actions, can affect fetal thyroid development, leading in some cases to adverse outcomes. Furthermore, there are a number of TRH analogues that share the same properties as the endogenous hormone. Thus, in this narrative review, we highlight the interaction of all the above with fetal growth in uncomplicated pregnancies.
Keywords: TRH; antithyroid drugs; feto-maternal interaction; fetus; thyroid.
Conflict of interest statement
All authors declare no conflicts of interest.
Figures
Similar articles
-
Effect of thyrotropin-releasing hormone on secretion of thyrotropin, prolactin, thyroxine, and triiodothyronine in pregnant and fetal rhesus monkeys.J Clin Endocrinol Metab. 1976 Nov;43(5):1020-8. doi: 10.1210/jcem-43-5-1020. J Clin Endocrinol Metab. 1976. PMID: 825527
-
Thyrotropin-releasing hormone is not required for thyrotropin secretion in the perinatal rat.J Clin Invest. 1979 Apr;63(4):588-94. doi: 10.1172/JCI109340. J Clin Invest. 1979. PMID: 108290 Free PMC article.
-
Response of the maternal, fetal, and neonatal pituitary-thyroid axis to thyrotropin-releasing hormone.Pediatr Res. 1986 Oct;20(10):982-6. doi: 10.1203/00006450-198610000-00018. Pediatr Res. 1986. PMID: 3095783
-
Drug therapy for hyperthyroidism in pregnancy: safety issues for mother and fetus.Drug Saf. 2000 Sep;23(3):229-44. doi: 10.2165/00002018-200023030-00005. Drug Saf. 2000. PMID: 11005705 Review.
-
Thyrotropin-releasing hormone and thyrotropin secretion.J Lab Clin Med. 1987 Mar;109(3):327-35. J Lab Clin Med. 1987. PMID: 3102657 Review.
Cited by
-
Preexisting Thyroid Disease in Pregnancy: A Brief Overview.Mo Med. 2022 Jul-Aug;119(4):360-365. Mo Med. 2022. PMID: 36118823 Free PMC article.
-
Cord blood metabolomic profiling in high risk newborns born to diabetic, obese, and overweight mothers: preliminary report.J Pediatr Endocrinol Metab. 2025 Apr 8;38(6):577-589. doi: 10.1515/jpem-2024-0605. Print 2025 Jun 26. J Pediatr Endocrinol Metab. 2025. PMID: 40196912
References
Publication types
LinkOut - more resources
Full Text Sources