Usefulness of the Modified Videofluoroscopic Dysphagia Scale in Choosing the Feeding Method for Stroke Patients with Dysphagia
- PMID: 34071752
- PMCID: PMC8226657
- DOI: 10.3390/healthcare9060632
Usefulness of the Modified Videofluoroscopic Dysphagia Scale in Choosing the Feeding Method for Stroke Patients with Dysphagia
Abstract
Introduction: The Videofluoroscopic Dysphagia Scale (VDS) is used to predict the long-term prognosis of dysphagia in patients with strokes. However, the inter-rater reliability of the VDS was low in a previous study. To overcome the mentioned limitations of the VDS, the modified version of the VDS (mVDS) was created and clinically applied to evaluate its usefulness in choosing the feeding method for stroke patients with dysphagia.
Methods: The videofluoroscopic swallowing study (VFSS) data of 56 stroke patients with dysphagia were collected retrospectively. We investigated the presence of aspiration pneumonia and the selected feeding method. We also evaluated the correlations between the mVDS and the selected feeding method, and between the mVDS and the presence of aspiration pneumonia after stroke. Univariate logistic regression and receiver operating characteristic analyses were used in the data analysis.
Results: The inter-rater reliability (Cronbach α value) of the total score of the mVDS was 0.886, which was consistent with very good inter-rater reliability. In all patients with dysphagia, the supratentorial stroke subgroup, and the infratentorial stroke subgroup, the mVDS scores were statistically correlated with the feeding method selected (p < 0.05) and the presence of aspiration pneumonia (p < 0.05).
Conclusions: The mVDS can be a useful scale for quantifying the severity of dysphagia, and it can be a useful tool in the clinical setting and in studies for interpreting the VFSS findings in stroke patients with dysphagia. Further studies with a greater number of patients and various stroke etiologies are required for more generalized applications of the mVDS.
Keywords: deglutition; dysphagia; modified version of the videofluoroscopic dysphagia scale; swallowing difficulty; videofluoroscopic dysphagia scale; videofluoroscopic swallowing study.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
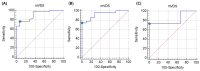
References
LinkOut - more resources
Full Text Sources

