Sarcopenia as a predictor of mortality among the critically ill in an intensive care unit: a systematic review and meta-analysis
- PMID: 34078275
- PMCID: PMC8173733
- DOI: 10.1186/s12877-021-02276-w
Sarcopenia as a predictor of mortality among the critically ill in an intensive care unit: a systematic review and meta-analysis
Abstract
Background: The evidence of sarcopenia based on CT-scan as an important prognostic factor for critically ill patients has not seen consistent results. To determine the impact of sarcopenia on mortality in critically ill patients, we performed a systematic review and meta-analysis to quantify the association between sarcopenia and mortality.
Methods: We searched studies from the literature of PubMed, EMBASE, and Cochrane Library from database inception to June 15, 2020. All observational studies exploring the relationship between sarcopenia based on CT-scan and mortality in critically ill patients were included. The search and data analysis were independently conducted by two investigators. A meta-analysis was performed using STATA Version 14.0 software using a fixed-effects model.
Results: Fourteen studies with a total of 3,249 participants were included in our meta-analysis. The pooled prevalence of sarcopenia among critically ill patients was 41 % (95 % CI:33-49 %). Critically ill patients with sarcopenia in the intensive care unit have an increased risk of mortality compared to critically ill patients without sarcopenia (OR = 2.28, 95 %CI: 1.83-2.83; P < 0.001; I2 = 22.1 %). In addition, a subgroup analysis found that sarcopenia was associated with high risk of mortality when defining sarcopenia by total psoas muscle area (TPA, OR = 3.12,95 %CI:1.71-5.70), skeletal muscle index (SMI, OR = 2.16,95 %CI:1.60-2.90), skeletal muscle area (SMA, OR = 2.29, 95 %CI:1.37-3.83), and masseter muscle(OR = 2.08, 95 %CI:1.15-3.77). Furthermore, critically ill patients with sarcopenia have an increased risk of mortality regardless of mortality types such as in-hospital mortality (OR = 1.99, 95 %CI:1.45-2.73), 30-day mortality(OR = 2.08, 95 %CI:1.36-3.19), and 1-year mortality (OR = 3.23, 95 %CI:2.08 -5.00).
Conclusions: Sarcopenia increases the risk of mortality in critical illness. Identifying the risk factors of sarcopenia should be routine in clinical assessments and offering corresponding interventions may help medical staff achieve good patient outcomes in ICU departments.
Keywords: Critically ill; Intensive care unit; Meta-analysis; Mortality; Sarcopenia.
Conflict of interest statement
None of the authors has any conflict of interest to declare.
Figures


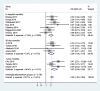



References
-
- Darmon M, Bourmaud A, Georges Q, Soares M, Jeon K, Oeyen S, Rhee CK, Gruber P, Ostermann M, Hill QA, et al. Changes in critically ill cancer patients’ short-term outcome over the last decades: results of systematic review with meta-analysis on individual data. Intensive care medicine. 2019;45(7):977–87. doi: 10.1007/s00134-019-05653-7. - DOI - PubMed
-
- Ceniccola GD, Holanda TP, Pequeno RSF, Mendonca VS, Oliveira ABM, Carvalho LSF, de Brito-Ashurst I, Araujo WMC. Relevance of AND-ASPEN criteria of malnutrition to predict hospital mortality in critically ill patients: A prospective study. J Crit Care. 2018;44:398–403. doi: 10.1016/j.jcrc.2017.12.013. - DOI - PubMed
-
- Rudd KE, Johnson SC, Agesa KM, Shackelford KA, Tsoi D, Kievlan DR, Colombara DV, Ikuta KS, Kissoon N, Finfer S, et al. Global, regional, and national sepsis incidence and mortality, 1990–2017: analysis for the Global Burden of Disease Study. Lancet. 2020;395(10219):200–11. doi: 10.1016/S0140-6736(19)32989-7. - DOI - PMC - PubMed
-
- Lee CW, Kou HW, Chou HS, Chou HH, Huang SF, Chang CH, Wu CH, Yu MC, Tsai HI. A combination of SOFA score and biomarkers gives a better prediction of septic AKI and in-hospital mortality in critically ill surgical patients: a pilot study. World journal of emergency surgery: WJES. 2018;13:41. doi: 10.1186/s13017-018-0202-5. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

