Acute kidney injury in 3182 patients admitted with COVID-19: a single-center, retrospective, case-control study
- PMID: 34079618
- PMCID: PMC7929007
- DOI: 10.1093/ckj/sfab021
Acute kidney injury in 3182 patients admitted with COVID-19: a single-center, retrospective, case-control study
Abstract
Background: Acute kidney injury (AKI) may develop in coronavirus disease 2019 (COVID-19) patients and may be associated with a worse outcome. The aim of this study is to describe AKI incidence during the first 45 days of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) pandemic in Spain, its reversibility and the association with mortality.
Methods: This was an observational retrospective case-control study based on patients hospitalized between 1 March and 15 April 2020 with SARS-CoV-2 infection and AKI. Confirmed AKI cases were compared with stable kidney function patients for baseline characteristics, analytical data, treatment and renal outcome. Patients with end-stage kidney disease were excluded.
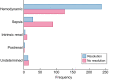
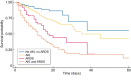
Results: AKI incidence was 17.22% among 3182 admitted COVID-19 patients and acute kidney disease (AKD) incidence was 6.82%. The most frequent causes of AKI were prerenal (68.8%) and sepsis (21.9%). Odds ratio (OR) for AKI was increased in patients with pre-existent hypertension [OR 2.58, 95% confidence interval (CI) 1.71-3.89] and chronic kidney disease (CKD) (OR 2.14, 95% CI 1.33-3.42) and in those with respiratory distress (OR 2.37, 95% CI 1.52-3.70). Low arterial pressure at admission increased the risk for Stage 3 AKI (OR 1.65, 95% CI 1.09-2.50). Baseline kidney function was not recovered in 45.73% of overall AKI cases and in 52.75% of AKI patients with prior CKD. Mortality was 38.5% compared with 13.4% of the overall sample population. AKI increased mortality risk at any time of hospitalization (hazard ratio 1.45, 95% CI 1.09-1.93).
Conclusions: AKI is frequent in COVID-19 patients and is associated with mortality, independently of acute respiratory distress syndrome. AKD was also frequent and merits adequate follow-up.
Keywords: COVID-19; acute kidney disease; acute kidney injury; case–control; chronic kidney disease; mortality.
© The Author(s) 2021. Published by Oxford University Press on behalf of ERA-EDTA.
Figures





References
LinkOut - more resources
Full Text Sources
Miscellaneous

