Census Tract Patterns and Contextual Social Determinants of Health Associated With COVID-19 in a Hispanic Population From South Texas: A Spatiotemporal Perspective
- PMID: 34081608
- PMCID: PMC8354426
- DOI: 10.2196/29205
Census Tract Patterns and Contextual Social Determinants of Health Associated With COVID-19 in a Hispanic Population From South Texas: A Spatiotemporal Perspective
Erratum in
-
Correction: Census Tract Patterns and Contextual Social Determinants of Health Associated With COVID-19 in a Hispanic Population From South Texas: A Spatiotemporal Perspective.JMIR Public Health Surveill. 2021 Aug 18;7(8):e32870. doi: 10.2196/32870. JMIR Public Health Surveill. 2021. PMID: 34406965 Free PMC article.
Abstract
Background: Previous studies have shown that various social determinants of health (SDOH) may have contributed to the disparities in COVID-19 incidence and mortality among minorities and underserved populations at the county or zip code level.
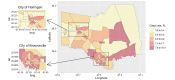
Objective: This analysis was carried out at a granular spatial resolution of census tracts to explore the spatial patterns and contextual SDOH associated with COVID-19 incidence from a Hispanic population mostly consisting of a Mexican American population living in Cameron County, Texas on the border of the United States and Mexico. We performed age-stratified analysis to identify different contributing SDOH and quantify their effects by age groups.
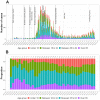
Methods: We included all reported COVID-19-positive cases confirmed by reverse transcription-polymerase chain reaction testing between March 18 (first case reported) and December 16, 2020, in Cameron County, Texas. Confirmed COVID-19 cases were aggregated to weekly counts by census tracts. We adopted a Bayesian spatiotemporal negative binomial model to investigate the COVID-19 incidence rate in relation to census tract demographics and SDOH obtained from the American Community Survey. Moreover, we investigated the impact of local mitigation policy on COVID-19 by creating the binary variable "shelter-in-place." The analysis was performed on all COVID-19-confirmed cases and age-stratified subgroups.
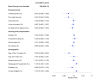
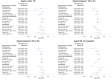
Results: Our analysis revealed that the relative incidence risk (RR) of COVID-19 was higher among census tracts with a higher percentage of single-parent households (RR=1.016, 95% posterior credible intervals [CIs] 1.005, 1.027) and a higher percentage of the population with limited English proficiency (RR=1.015, 95% CI 1.003, 1.028). Lower RR was associated with lower income (RR=0.972, 95% CI 0.953, 0.993) and the percentage of the population younger than 18 years (RR=0.976, 95% CI 0.959, 0.993). The most significant association was related to the "shelter-in-place" variable, where the incidence risk of COVID-19 was reduced by over 50%, comparing the time periods when the policy was present versus absent (RR=0.506, 95% CI 0.454, 0.563). Moreover, age-stratified analyses identified different significant contributing factors and a varying magnitude of the "shelter-in-place" effect.
Conclusions: In our study, SDOH including social environment and local emergency measures were identified in relation to COVID-19 incidence risk at the census tract level in a highly disadvantaged population with limited health care access and a high prevalence of chronic conditions. Results from our analysis provide key knowledge to design efficient testing strategies and assist local public health departments in COVID-19 control, mitigation, and implementation of vaccine strategies.
Keywords: Bayesian; COVID-19; health inequity; social determinants of health; spatial pattern; underserved population.
©Cici Bauer, Kehe Zhang, Miryoung Lee, Susan Fisher-Hoch, Esmeralda Guajardo, Isela de la Cerda, Isela de la Cerda, Maria E Fernandez, Belinda Reininger. Originally published in JMIR Public Health and Surveillance (https://publichealth.jmir.org), 05.08.2021.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures
References
-
- Abrams EM, Szefler SJ. COVID-19 and the impact of social determinants of health. Lancet Respir Med. 2020 Jul;8(7):659–661. doi: 10.1016/S2213-2600(20)30234-4. http://europepmc.org/abstract/MED/32437646 - DOI - PMC - PubMed
-
- Golestaneh L, Neugarten J, Fisher M, Billett HH, Gil MR, Johns T, Yunes M, Mokrzycki MH, Coco M, Norris KC, Perez HR, Scott S, Kim RS, Bellin E. The association of race and COVID-19 mortality. EClinicalMedicine. 2020 Aug;25:100455. doi: 10.1016/j.eclinm.2020.100455. https://linkinghub.elsevier.com/retrieve/pii/S2589-5370(20)30199-1 - DOI - PMC - PubMed
-
- Boserup B, McKenney M, Elkbuli A. Disproportionate impact of COVID-19 pandemic on racial and ethnic minorities. Am Surg. 2020 Dec;86(12):1615–1622. doi: 10.1177/0003134820973356. https://journals.sagepub.com/doi/10.1177/0003134820973356?url_ver=Z39.88... - DOI - PMC - PubMed
-
- Li D, Gaynor SM, Quick C, Chen JT, Stephenson BJK, Coull BA, Lin X. Unraveling US National COVID-19 racial/ethnic disparities using county level data among 328 million Americans. medRxiv. doi: 10.1101/2020.12.02.20234989. Preprint posted online on January 12, 2021. - DOI
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

