Non-Persistence With Antiplatelet Medications Among Older Patients With Peripheral Arterial Disease
- PMID: 34093210
- PMCID: PMC8170080
- DOI: 10.3389/fphar.2021.687549
Non-Persistence With Antiplatelet Medications Among Older Patients With Peripheral Arterial Disease
Abstract
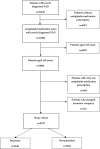
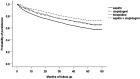
Introduction: Antiplatelet therapy needs to be administered life-long in patients with peripheral arterial disease (PAD). Our study was aimed at 1) the analysis of non-persistence with antiplatelet medication in older PAD patients and 2) identification of patient- and medication-related characteristics associated with non-persistence. Methods: The study data was retrieved from the database of the General Health Insurance Company. The study cohort of 9,178 patients aged ≥ 65 years and treated with antiplatelet medications was selected from 21,433 patients in whom PAD was newly diagnosed between 01/2012 and 12/2012. Patients with a 6 months treatment gap without antiplatelet medication prescription were classified as non-persistent. Characteristics associated with non-persistence were identified using the Cox regression. Results: At the end of the 5 years follow-up, 3,032 (33.0%) patients were non-persistent. Age, history of ischemic stroke or myocardial infarction, clopidogrel or combination of aspirin with clopidogrel used at the index date, higher co-payment, general practitioner as index prescriber and higher overall number of medications were associated with persistence, whereas female sex, atrial fibrillation, anxiety disorders, bronchial asthma/chronic obstructive pulmonary disease, being a new antiplatelet medication user (therapy initiated in association with PAD diagnosis), and use of anticoagulants or antiarrhythmic agents were associated with non-persistence. Conclusion: In patients with an increased probability of non-persistence, an increased attention should be paid to improvement of persistence.
Keywords: antiplatelet medications; anxiety disorders; atrial fibrillation; discontinuation; non-persistence; peripheral arterial disease.
Copyright © 2021 Wawruch, Murin, Tesar, Paduchova, Petrova, Celovska, Havelkova, Trnka and Aarnio.
Conflict of interest statement
BH is employed by General Health Insurance Company. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Aboyans V., Ricco J. B., Bartelink M. E. L., Björck M., Brodmann M., Cohnert T., et al. (2018). ESC Scientific Document GroupESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in Collaboration with the European Society for Vascular Surgery (ESVS): Document Covering Atherosclerotic Disease of Extracranial Carotid and Vertebral, Mesenteric, Renal, Upper and Lower Extremity arteriesEndorsed by: the European Stroke Organization (ESO)The Task Force for the Diagnosis and Treatment of Peripheral Arterial Diseases of the European Society of Cardiology (ESC) and of the European Society for Vascular Surgery (ESVS). Eur. Heart J. 39 (9), 763–816. 10.1093/eurheartj/ehx095 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous