Preoperative Gadoxetic Acid-Enhanced MRI Based Nomogram Improves Prediction of Early HCC Recurrence After Ablation Therapy
- PMID: 34094938
- PMCID: PMC8176857
- DOI: 10.3389/fonc.2021.649682
Preoperative Gadoxetic Acid-Enhanced MRI Based Nomogram Improves Prediction of Early HCC Recurrence After Ablation Therapy
Abstract
Purpose: This study aimed to identify preoperative gadoxetic acid-enhanced MRI features and establish a nomogram for predicting early recurrence (≤ 2 years) of hepatocellular carcinoma (HCC) after ablation therapy.
Methods: A total of 160 patients who underwent gadoxetic acid-enhanced MRI and ablation HCC therapy from January 2015 to June 2018, were included retrospectively and divided into a training cohort (n = 112) and a validation cohort (n = 48). Independent clinical risk factors and gadoxetic acid-enhanced MRI features associated with early recurrence were identified by univariate and multivariate logistic regression analysis and used for construction of a nomogram. The performance of the nomogram was evaluated by discrimination, calibration, and clinical utility.
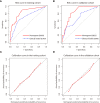
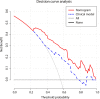
Results: Alpha-fetoprotein (AFP) level, tumor number, arterial peritumoral enhancement, satellite nodule and peritumoral hypointensity at hepatobiliary phases in the training cohort were identified as independent risk factors for early recurrence after ablation. A new nomogram that was constructed with these five features showed an area under the curve (AUC) of 0.843 (95%CI 0.771-0.916) and 0.835 (95%CI 0.713-0.956) in the training and validation cohort, respectively. The calibration curve and decision curve analysis (DCA) suggested that the nomogram had good consistency and clinical utility.
Conclusions: A new nomogram that was constructed using four preoperative gadoxetic acid-enhanced MRI features and serum AFP level can predict the risk of early HCC recurrence after ablation therapy with AUC up to 0.843. The strong performance of this nomogram may help hepatologists to categorize patients' recurrent risk to guide selecting treatment options and improve postoperative management.
Keywords: ablation technique; early recurrence; hepatocellular carcinoma; magnetic resonance imaging; nomogram; prediction.
Copyright © 2021 Hu, Song, Zhang, Dai, Tang, Li, Liao, Zhou, Xu, Zhang and Zhou.
Conflict of interest statement
Y-YZ is the founder and CSO of HBVtech. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures





References
-
- Fitzmaurice C, Allen C, Barber RM, Barregard L, Bhutta ZA, Brenner H, et al. Global, Regional, and National Cancer Incidence, Mortality, Years of Life Lost, Years Lived With Disability, and Disability-Adjusted Life-Years for 32 Cancer Groups, 1990 to 2015: A Systematic Analysis for the Global Burden of Disease Study. JAMA Oncol (2017) 3(4):524–48. 10.1001/jamaoncol.2016.5688 - DOI - PMC - PubMed
-
- Vietti VN, Duran R, Guiu B, Cercueil JP, Aube C, Digklia A, et al. Efficacy of Microwave Ablation Versus Radiofrequency Ablation for the Treatment of Hepatocellular Carcinoma in Patients With Chronic Liver Disease: A Randomised Controlled Phase 2 Trial. Lancet Gastroenterol Hepatol (2018) 3(5):317–25. 10.1016/S2468-1253(18)30029-3 - DOI - PubMed
LinkOut - more resources
Full Text Sources

