Comparison of the clinical effect between the lower sternal incision and the left parasternal fourth intercostal incision in the transthoracic closure of ventricular septal defect
- PMID: 34099026
- PMCID: PMC8186159
- DOI: 10.1186/s13019-021-01543-6
Comparison of the clinical effect between the lower sternal incision and the left parasternal fourth intercostal incision in the transthoracic closure of ventricular septal defect
Abstract
Background: To analyze the clinical effect of two different ways of minimally invasive transthoracic closure in children with ventricular septal defect (VSD).
Methods: From January 2015 to July 2019, 294 children with VSD were enrolled in the Fujian Medical University Union Hospital. Patients were divided into two groups - those who underwent VSD closure through the left sternal fourth intercostal incision (group A: n = 95) and the lower sternal incision (group B: n = 129).
Results: The operation time, bleeding volume, postoperative mechanical ventilation time, postoperative intensive care unit (ICU) monitoring time, postoperative hospitalization time and complication rate in group A were significantly lower than those in group B (P < 0.05). There was no significant difference between the two groups in the operation success rate, mechanical ventilation time and total hospitalization cost (P > 0.05).
Conclusion: The transthoracic closure of ventricular septal defect through the left sternal fourth intercostal incision is feasible, safe, cosmetic, and worth popularizing.
Keywords: Cardiac intervention; Congenital heart diseases; Ventricular septal defect.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

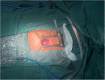
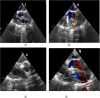
References
-
- Liang W, Zhou S, Fan T, et al. Midterm Results of Transaxillary Occluder Device Closure of Perimembranous Ventricular Septal Defect Guided Solely by Transesophageal Echocardiography. [J]. Heart Surgery Forum. 2019;22(2). - PubMed
-
- Roos-Hesselink JW, Meijboom FJ, Spitaels SE, Van Domburg R, Van Rijen EH, Utens EM, Bogers AJ, Simoons ML. Outcome of patients after surgical closure of ventricular septal defect at young age: longitudinal follow-up of 22-34 years. Eur Heart J. 2004;25(12):1057–1062. doi: 10.1016/j.ehj.2004.04.012. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

