Characterization of Bacterial and Fungal Infections in Hospitalized Patients With Coronavirus Disease 2019 and Factors Associated With Health Care-Associated Infections
- PMID: 34099978
- PMCID: PMC8135866
- DOI: 10.1093/ofid/ofab201
Characterization of Bacterial and Fungal Infections in Hospitalized Patients With Coronavirus Disease 2019 and Factors Associated With Health Care-Associated Infections
Abstract
Background: Patients hospitalized with coronavirus disease 2019 (COVID-19) are at increased risk of health care-associated infections (HAIs), especially with prolonged hospital stays. We sought to identify incidence, antimicrobial susceptibilities, and outcomes associated with bacterial/fungal secondary infections in a large cohort of patients with COVID-19.
Methods: We evaluated adult patients diagnosed with COVID-19 between 2 March and 31 May 2020 and hospitalized >24 hours. Data extracted from medical records included diagnoses, vital signs, laboratory results, microbiological data, and antibiotic use. Microbiologically confirmed bacterial and fungal pathogens from clinical cultures were evaluated to characterize community- and health care-associated infections, including describing temporal changes in predominant organisms on presentation and throughout hospitalization. Univariable and multivariable logistic regression analyses were performed to investigate risk factors for HAIs.
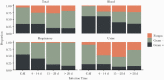
Results: A total of 3028 patients were included and accounted for 899 positive clinical cultures. Overall, 516 (17%) patients with positive cultures met criteria for infection. Community-associated coinfections were identified in 183 (6%) patients, whereas HAIs occurred in 350 (12%) patients. Fifty-seven percent of HAIs were caused by gram-negative bacteria and 19% by fungi. Antibiotic resistance increased with longer hospital stays, with incremental increases in the proportion of vancomycin resistance among enterococci and ceftriaxone and carbapenem resistance among Enterobacterales. Intensive care unit stay, invasive mechanical ventilation, and steroids were associated with HAIs.
Conclusions: HAIs occur in a small proportion of patients hospitalized with COVID-19 and are most often caused by gram-negative and fungal pathogens. Antibiotic resistance is more prevalent with prolonged hospital stays. Antimicrobial stewardship is imperative in this population to minimize unnecessary broad-spectrum antibiotic use.
Keywords: COVID-19; bacterial infections; health care–associated infection.
© The Author(s) 2021. Published by Oxford University Press on behalf of Infectious Diseases Society of America.
Figures
References
-
- Arabi YM, Al-Omari A, Mandourah Y, et al. . Saudi Critical Care Trial Group . Critically ill patients with the Middle East respiratory syndrome: a multicenter retrospective cohort study. Crit Care Med 2017; 45:1683–95. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous