Short and Long-term Outcomes of Subarachnoid Hemorrhage Treatment according to Hospital Volume in Korea: a Nationwide Multicenter Registry
- PMID: 34100560
- PMCID: PMC8185126
- DOI: 10.3346/jkms.2021.36.e146
Short and Long-term Outcomes of Subarachnoid Hemorrhage Treatment according to Hospital Volume in Korea: a Nationwide Multicenter Registry
Abstract
Background: Subarachnoid hemorrhage is a potentially devastating cerebrovascular attack with a high proportion of poor outcomes and mortality. Recent studies have reported decreased mortality with the improvement in devices and techniques for treating ruptured aneurysms and neurocritical care. This study investigated the relationship between hospital volume and short- and long-term mortality in patients treated with subarachnoid hemorrhage.
Methods: We selected subarachnoid hemorrhage patients treated with clipping and coiling from March-May 2013 to June-August 2014 using data from Acute Stroke Registry, and the selected subarachnoid hemorrhage (SAH) patients were tracked in connection with data of Health Insurance Review and Assessment Service to evaluate the short-term and long-term mortality.
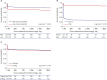
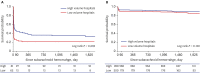
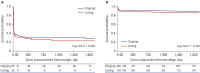
Results: A total of 625 subarachnoid hemorrhage patients were admitted to high-volume hospitals (n = 355, 57%) and low-volume hospitals (n = 270, 43%) for six months. The mortality of SAH patients treated with clipping and coiling was 12.3%, 20.2%, 21.4%, and 24.3% at 14 days, three months, one year, and five years, respectively. The short-term and long-term mortality in high-volume hospitals was significantly lower than that in low-volume hospitals. On Cox regression analysis of death in patients with severe clinical status, low-volume hospitals had significantly higher mortality than high-volume hospitals during short-term follow-up. On Cox regression analysis in the mild clinical status group, there was no statistical difference between high-volume hospitals and low-volume hospitals.
Conclusion: In subarachnoid hemorrhage patients treated with clipping and coiling, low-volume hospitals had higher short-term mortality than high-volume hospitals. These results from a nationwide database imply that acute SAH should be treated by a skilled neurosurgeon with adequate facilities in a high-volume hospital.
Keywords: Mortality; Stroke; Subarachnoid Hemorrhage.
© 2021 The Korean Academy of Medical Sciences.
Conflict of interest statement
The authors have no potential conflicts of interest to disclose.
Figures
Similar articles
-
Short- and long-term mortality of subarachnoid hemorrhage according to hospital volume and severity using a nationwide multicenter registry study.Front Neurol. 2022 Aug 5;13:952794. doi: 10.3389/fneur.2022.952794. eCollection 2022. Front Neurol. 2022. PMID: 35989903 Free PMC article.
-
Effects of case volume and comprehensive stroke center capabilities on patient outcomes of clipping and coiling for subarachnoid hemorrhage.J Neurosurg. 2020 Mar 13;134(3):929-939. doi: 10.3171/2019.12.JNS192584. Print 2021 Mar 1. J Neurosurg. 2020. PMID: 32168489
-
Association Between Hospital Volumes and Clinical Outcomes for Patients With Nontraumatic Subarachnoid Hemorrhage.J Am Heart Assoc. 2021 Aug 3;10(15):e018373. doi: 10.1161/JAHA.120.018373. Epub 2021 Jul 30. J Am Heart Assoc. 2021. PMID: 34325522 Free PMC article.
-
Endovascular coiling versus neurosurgical clipping for people with aneurysmal subarachnoid haemorrhage.Cochrane Database Syst Rev. 2018 Aug 15;8(8):CD003085. doi: 10.1002/14651858.CD003085.pub3. Cochrane Database Syst Rev. 2018. PMID: 30110521 Free PMC article.
-
In-hospital mortality and poor outcome after surgical clipping and endovascular coiling for aneurysmal subarachnoid hemorrhage using nationwide databases: a systematic review and meta-analysis.Neurosurg Rev. 2020 Apr;43(2):655-667. doi: 10.1007/s10143-019-01096-2. Epub 2019 Apr 2. Neurosurg Rev. 2020. PMID: 30941595
Cited by
-
Utility of Exosomes in Ischemic and Hemorrhagic Stroke Diagnosis and Treatment.Int J Mol Sci. 2022 Jul 28;23(15):8367. doi: 10.3390/ijms23158367. Int J Mol Sci. 2022. PMID: 35955498 Free PMC article. Review.
-
Trends in Incidences, Treatments and Outcomes of Spontaneous Subarachnoid Hemorrhage in Korea Between 2002 and 2022.J Korean Med Sci. 2025 Jul 28;40(29):e171. doi: 10.3346/jkms.2025.40.e171. J Korean Med Sci. 2025. PMID: 40726239 Free PMC article.
-
Epidemiology and Functional Outcome of Acute Stroke Patients in Korea Using Nationwide data.J Korean Neurosurg Soc. 2025 Mar;68(2):159-176. doi: 10.3340/jkns.2024.0118. Epub 2024 Sep 24. J Korean Neurosurg Soc. 2025. PMID: 39313854 Free PMC article.
-
Short- and long-term mortality of subarachnoid hemorrhage according to hospital volume and severity using a nationwide multicenter registry study.Front Neurol. 2022 Aug 5;13:952794. doi: 10.3389/fneur.2022.952794. eCollection 2022. Front Neurol. 2022. PMID: 35989903 Free PMC article.
-
Clinical Characteristics and Outcomes of Patients with Aneurysmal Subarachnoid Hemorrhage: A Prospective Multicenter Study in a Middle-Income Country.Neurocrit Care. 2023 Apr;38(2):378-387. doi: 10.1007/s12028-022-01629-6. Epub 2022 Nov 2. Neurocrit Care. 2023. PMID: 36324005
References
-
- Chan V, O'Kelly C, McQuiggan J, Zagorski B, Hill MD, O'Kelly C. Declining admission and mortality rates for subarachnoid hemorrhage in Canada between 2004 and 2015. Stroke. 2019;50(5):e133. - PubMed
-
- Suarez JI, Zaidat OO, Suri MF, Feen ES, Lynch G, Hickman J, et al. Length of stay and mortality in neurocritically ill patients: impact of a specialized neurocritical care team. Crit Care Med. 2004;32(11):2311–2317. - PubMed
-
- Rincon F, Rossenwasser RH, Dumont A. The epidemiology of admissions of nontraumatic subarachnoid hemorrhage in the United States. Neurosurgery. 2013;73(2):217–222. - PubMed
-
- Spetzler RF, McDougall CG, Zabramski JM, Albuquerque FC, Hills NK, Russin JJ, et al. The barrow ruptured aneurysm trial: 6-year results. J Neurosurg. 2015;123(3):609–617. - PubMed
-
- Spetzler RF, McDougall CG, Zabramski JM, Albuquerque FC, Hills NK, Nakaji P, et al. Ten-year analysis of saccular aneurysms in the barrow ruptured aneurysm trial. J Neurosurg. 2019;132(3):771–776. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

