Brain injury in preterm infants with surgical necrotizing enterocolitis: clinical and bowel pathological correlates
- PMID: 34103675
- PMCID: PMC10308193
- DOI: 10.1038/s41390-021-01614-3
Brain injury in preterm infants with surgical necrotizing enterocolitis: clinical and bowel pathological correlates
Abstract
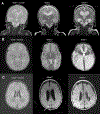
Background: The objective of this study was to determine the risk factors and outcomes of white matter brain injury (WMBI) on magnetic resonance imaging (MRI) at term-equivalent age in infants with surgical necrotizing enterocolitis (NEC).
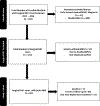
Methods: This retrospective study compared clinical/pathological information between infants with and those without WMBI.
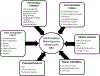
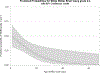
Results: Out of 69 infants with surgical NEC, 17 (24.6%) had mild WMBI, 13 (18.8%) had moderate WMBI, and six (8.7%) had severe WMBI on the brain MRI. Several clinical factors (gestational age, more red blood cell (RBC) transfusions before NEC onset, pneumoperitoneum, earlier NEC onset age, postoperative ileus, acute kidney injury (AKI) by serum creatinine, postnatal steroids, hospital stay) and histopathological findings (necrosis, hemorrhage) had univariate associations with WMBI. Associations with RBC transfusion (odds ratio (OR) 23.6 [95% confidence interval (CI): 4.73-117.97]; p = 0.0001), age at NEC onset (OR 0.30 [95%CI: 0.11-0.84]; p = 0.021), necrosis (OR 0.10 [95%CI: 0.01-0.90]; p = 0.040), and bowel hemorrhage (OR 7.79 [95%CI: 2.19-27.72]; p = 0.002) persisted in multivariable association with grade 3-4 WMBI. The infants with WMBI had lower mean motor, cognitive, language scores, and higher ophthalmic morbidity at 2 years of age.
Conclusions: The WMBI was most likely associated with earlier NEC onset, higher RBC transfusions, and less necrosis and greater hemorrhage lesions on intestinal pathology in preterm infants with surgical NEC.
Impact: In preterm infants with surgical NEC, brain MRI showed injury in the white matter in 52%, gray matter in 10%, and cerebellar region in 30%. Preterm infants with severe WMBI (grade 3-4) had less necrosis and greater hemorrhagic lesions on histopathology of the bowel. Preterm infants with WMBI were more likely to have a more severe postoperative course, AKI, and longer length of hospitalization. Neuroprotective strategies to prevent brain injury in preterm infants with surgical NEC are needed with the goal of improving the neurodevelopmental outcomes.
© 2021. The Author(s), under exclusive licence to the International Pediatric Research Foundation, Inc.
Conflict of interest statement
Figures