Trigeminal neuralgia: a practical guide
- PMID: 34108244
- PMCID: PMC8461413
- DOI: 10.1136/practneurol-2020-002782
Trigeminal neuralgia: a practical guide
Abstract
Trigeminal neuralgia (TN) is a highly disabling disorder characterised by very severe, brief and electric shock like recurrent episodes of facial pain. New diagnostic criteria, which subclassify TN on the basis of presence of trigeminal neurovascular conflict or an underlying neurological disorder, should be used as they allow better characterisation of patients and help in decision-making regarding medical and surgical treatments. MR imaging, including high-resolution trigeminal sequences, should be performed as part of the diagnostic work-up. Carbamazepine and oxcarbazepine are drugs of first choice. Lamotrigine, gabapentin, pregabalin, botulinum toxin type A and baclofen can be used either alone or as add-on therapy. Surgery should be considered if the pain is poorly controlled or the medical treatments are poorly tolerated. Trigeminal microvascular decompression is the first-line surgery in patients with trigeminal neurovascular conflict while neuroablative surgical treatments can be offered if MR imaging does not show any neurovascular contact or where patients are considered too frail for microvascular decompression or do not wish to take the risk.
Keywords: headache; pain; trigeminal nerve; trigeminal neuralgia.
© Author(s) (or their employer(s)) 2021. Re-use permitted under CC BY. Published by BMJ.
Conflict of interest statement
Competing interests: GL has received speaker honoraria, funding for travel and has received honoraria for participation in advisory boards sponsored by Allergan, Novartis, Eli Lilly and TEVA. He has received speaker honoraria, funding for travel from electroCore, Nevro Corp and Autonomic Technologies. JZ serves on the advisory board of Biogen and Eli Lilly and received payment from Biogen for design of drug trials. MM serves on the advisory board for Abbott, Allergan, Eli Lilly, Medtronic, Novartis and TEVA, and has received payment for the development of educational presentations from Allergan, electroCore, Eli Lilly, Novartis and TEVA.
Figures
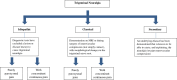


References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
