A Personalized Mobile Health Program for Type 2 Diabetes During the COVID-19 Pandemic: Single-Group Pre-Post Study
- PMID: 34111018
- PMCID: PMC8274679
- DOI: 10.2196/25820
A Personalized Mobile Health Program for Type 2 Diabetes During the COVID-19 Pandemic: Single-Group Pre-Post Study
Abstract
Background: With increasing type 2 diabetes prevalence, there is a need for effective programs that support diabetes management and improve type 2 diabetes outcomes. Mobile health (mHealth) interventions have shown promising results. With advances in wearable sensors and improved integration, mHealth programs could become more accessible and personalized.
Objective: The study aimed to evaluate the feasibility, acceptability, and effectiveness of a personalized mHealth-anchored intervention program in improving glycemic control and enhancing care experience in diabetes management. The program was coincidentally implemented during the national-level lockdown for COVID-19 in Singapore, allowing for a timely study of the use of mHealth for chronic disease management.
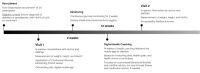
Methods: Patients with type 2 diabetes or prediabetes were enrolled from the Singapore Armed Forces and offered a 3-month intervention program in addition to the usual care they received. The program was standardized to include (1) in-person initial consultation with a clinical dietitian; (2) in-person review with a diabetes specialist doctor; (3) 1 continuous glucose monitoring device; (4) access to the mobile app for dietary intake and physical activity tracking, and communication via messaging with the dietitian and doctor; and (5) context-sensitive digital health coaching over the mobile app. Medical support was rendered to the patients on an as-needed basis when they required advice on adjustment of medications. Measurements of weight, height, and glycated hemoglobin A1c (HbA1c) were conducted at 2 in-person visits at the start and end of the program. At the end of the program, patients were asked to complete a short acceptability feedback survey to understand the motivation for joining the program, their satisfaction, and suggestions for improvement.
Results: Over a 4-week recruitment period, 130 individuals were screened, the enrollment target of 30 patients was met, and 21 patients completed the program and were included in the final analyses; 9 patients were lost to follow-up (full data were not available for the final analyses). There were no differences in the baseline characteristics between patients who were included and excluded from the final analyses (age category: P=.23; gender: P=.21; ethnicity: P>.99; diabetes status category: P=.52, medication adjustment category: P=.65; HbA1c category: P=.69; BMI: P>.99). The 21 patients who completed the study rated a mean of 9.0 out of 10 on the Likert scale for both satisfaction questions. For the Yes-No question on benefit of the program, all of the patients selected "Yes." Mean HbA1c decreased from 7.6% to 7.0% (P=.004). There were no severe hypoglycemia events (glucose level <3.0 mmol/L) reported. Mean weight decreased from 76.8 kg to 73.9 kg (P<.001), a mean decrease of 3.5% from baseline weight. Mean BMI decreased from 27.8 kg/m2 to 26.7 kg/m2 (P<.001).
Conclusions: The personalized mHealth program was feasible, acceptable, and produced significant reductions in HbA1c (P=.004) and body weight (P<.001) in individuals with type 2 diabetes. Such mHealth programs could overcome challenges posed to chronic disease management by COVID-19, including disruptions to in-person health care access.
Keywords: COVID-19; HbA1c; blood glucose; body mass index; chronic disease; diabetes; glycated hemoglobin A; intervention; mHealth; mobile applications; outcome; prediabetic state; self-management; text messaging; type 2 diabetes.
©Ian Yi Han Ang, Kyle Xin Quan Tan, Clive Tan, Chiew Hoon Tan, James Wei Ming Kwek, Joanne Tay, Sue Anne Toh. Originally published in JMIR Diabetes (https://diabetes.jmir.org), 09.07.2021.
Conflict of interest statement
Conflicts of Interest: KTXQ, JT, and SAT are cofounders and shareholders of NOVI Health. IYHA, CT, TCH, and JWMK declare no conflicts of interest.
Figures

References
-
- Saeedi P, Petersohn I, Salpea P, Malanda B, Karuranga S, Unwin N, Colagiuri S, Guariguata L, Motala AA, Ogurtsova K, Shaw JE, Bright D, Williams R, IDF Diabetes Atlas Committee Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: results from the International Diabetes Federation Diabetes Atlas, 9 edition. Diabetes Res Clin Pract. 2019 Nov;157:107843. doi: 10.1016/j.diabres.2019.107843. - DOI - PubMed
-
- Ng SHX, Rahman N, Ang IYH, Sridharan S, Ramachandran S, Wang DD, Khoo A, Tan CS, Feng M, Toh SES, Tan XQ. Characterising and predicting persistent high-cost utilisers in healthcare: a retrospective cohort study in Singapore. BMJ Open. 2020 Jan 06;10(1):e031622. doi: 10.1136/bmjopen-2019-031622. https://bmjopen.bmj.com/lookup/pmidlookup?view=long&pmid=31911514 - DOI - PMC - PubMed
-
- Aziz Z, Absetz P, Oldroyd J, Pronk NP, Oldenburg B. A systematic review of real-world diabetes prevention programs: learnings from the last 15 years. Implement Sci. 2015 Dec 15;10:172. doi: 10.1186/s13012-015-0354-6. https://implementationscience.biomedcentral.com/articles/10.1186/s13012-... - DOI - DOI - PMC - PubMed
-
- Chrvala CA, Sherr D, Lipman RD. Diabetes self-management education for adults with type 2 diabetes mellitus: a systematic review of the effect on glycemic control. Patient Educ Couns. 2016 Dec;99(6):926–43. doi: 10.1016/j.pec.2015.11.003. https://linkinghub.elsevier.com/retrieve/pii/S0738-3991(15)30116-6 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

