Risk of Lung Allograft Dysfunction Associated With Aspergillus Infection
- PMID: 34113715
- PMCID: PMC8184025
- DOI: 10.1097/TXD.0000000000001128
Risk of Lung Allograft Dysfunction Associated With Aspergillus Infection
Abstract
We sought to determine whether invasive aspergillosis (IA) during the first year after lung transplantation increased the risk of chronic lung allograft dysfunction (CLAD).
Methods: We retrospectively reviewed the records of 191 patients who underwent lung transplantation at our institution between January 2013 and December 2017. Screening for Aspergillus was with bronchial aspirates, bronchoalveolar lavage if indicated or during surveillance bronchoscopy, radiography, and computed tomography. We used Fine and Gray multivariable regression to identify potential risk factors for CLAD.
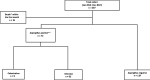
Results: During the first posttransplant year, 72 patients had at least 1 deep-airway sample positive for Aspergillus; 63 were classified as having IA and were included in the study. Median number of endoscopies per patient during the first year was 9 (range, 1-44). Median time from transplantation to first Aspergillus-positive sample was 121 d. Bronchial aspirate samples and bronchoalveolar lavage fluid were positive in 71 and 44 patients, respectively. Aspergillus fumigatus (n = 36, 50%) predominated; bacterial samples were also positive in 22 (31%) patients. IA within 4 mo after transplantation was independently associated with CLAD development (subdistribution hazard ratio, 3.75; 95% confidence interval [CI], 1.61-8.73; P < 0.01) by regression analysis. Survival at 3 and 5 y conditional on 1-y CLAD-free survival was 37% (95% CI, 24%-58%), and 24% (95% CI, 11%-52%) in the IA <4 mo group compared to 65% (95% CI, 57%-73%) and 54% (95% CI, 43%-66%) in the non-IA group and to 69% (95% CI, 58%-83%) and 54% (95% CI, 35%-82%) in the IA ≥4 mo group, respectively (P < 0.01, logrank test).
Conclusions: Our evaluation of de novo IA showed that this infection was most strongly associated with CLAD when found within 4 mo after transplantation.
Copyright © 2021 The Author(s). Transplantation Direct. Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
The authors declare no funding or conflicts of interest.
Figures


References
-
- Chambers DC, Cherikh WS, Harhay MO, et al. ; International Society for Heart and Lung Transplantation. The international thoracic organ transplant registry of the International Society for Heart and Lung Transplantation: thirty-sixth adult lung and heart-lung transplantation report-2019; Focus theme: donor and recipient size match. J Heart Lung Transplant. 2019; 38:1042–1055 - PMC - PubMed
-
- Bando K, Paradis IL, Similo S, et al. . Obliterative bronchiolitis after lung and heart-lung transplantation. An analysis of risk factors and management. J Thorac Cardiovasc Surg. 1995; 110:4–13; discussion 13 - PubMed
-
- Girgis RE, Tu I, Berry GJ, et al. . Risk factors for the development of obliterative bronchiolitis after lung transplantation. J Heart Lung Transplant. 1996; 15:1200–1208 - PubMed
LinkOut - more resources
Full Text Sources

