Inches, Centimeters, and Yards: Overlooked Definition Choices Inhibit Interpretation of Morphine Equivalence
- PMID: 34116543
- PMCID: PMC8270512
- DOI: 10.1097/AJP.0000000000000948
Inches, Centimeters, and Yards: Overlooked Definition Choices Inhibit Interpretation of Morphine Equivalence
Abstract
Objective: Morphine-standardized doses are used in clinical practice and research to account for molecular potency. Ninety milligrams of morphine equivalents (MME) per day are considered a "high dose" risk threshold in guidelines, laws, and by payers. Although ubiquitously cited, the "CDC definition" of daily MME lacks a clearly defined denominator. Our objective was to assess denominator-dependency on "high dose" classification across competing definitions.
Methods: To identify definitional variants, we reviewed literature and electronic prescribing tools, yielding 4 unique definitions. Using Prescription Drug Monitoring Programs data (July to September 2018), we conducted a population-based cohort study of 3,916,461 patients receiving outpatient opioid analgesics in California (CA) and Florida (FL). The binary outcome was whether patients were deemed "high dose" (>90 MME/d) compared across 4 definitions. We calculated I2 for heterogeneity attributable to the definition.
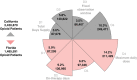
Results: Among 9,436,640 prescriptions, 42% overlapped, which led denominator definitions to impact daily MME values. Across definitions, average daily MME varied 3-fold (range: 17 to 52 [CA] and 23 to 65 mg [FL]). Across definitions, prevalence of "high dose" individuals ranged 5.9% to 14.2% (FL) and 3.5% to 10.3% (CA). Definitional variation alone would impact a hypothetical surveillance study trying to establish how much more "high dose" prescribing was present in FL than CA: from 39% to 84% more. Meta-analyses revealed strong heterogeneity (I2 range: 86% to 99%). In sensitivity analysis, including unit interval 90.0 to 90.9 increased "high dose" population fraction by 15%.
Discussion: While 90 MME may have cautionary mnemonic benefits, without harmonization of calculation, its utility is limited. Comparison between studies using daily MME requires explicit attention to definitional variation.
Copyright © 2021 The Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
Supported by FDA and BJA. US Food and Drug Administration, Silver Spring, MD (HHSF223201810183C) funded the efforts of N.D., B.A.C., and T.C. The US Department of Justice, Bureau of Justice Assistance, Washington, DC (2017-PM-BX-K038) funded the efforts of Y.W., J.B., and C.D. The BJA is a component of the Department of Justice’s Office of Justice Programs, which also includes the Bureau of Justice Statistics, the National Institute of Justice, the Office of Juvenile Justice and Delinquency Prevention, the Office for Victims of Crime, and the SMART Office. Funding agencies had no involvement in study design, analysis, interpretation, or decision to publish. N.D. is a part-time methods consultant to the Researched Abuse, Diversion, and Addiction-Related Surveillance (RADARS) System of Denver Health and Hospitals Authority, a political subdivision of the State of Colorado. RADARS System had no knowledge of or involvement in this analysis. N.D. has no relationship with any pharmaceutical manufacturer or distributor. The remaining authors declare no conflict of interest.
Figures
Similar articles
-
The association between hydroxyurea adherence and opioid utilization among Texas Medicaid enrollees with sickle cell disease.J Manag Care Spec Pharm. 2020 Nov;26(11):1412-1422. doi: 10.18553/jmcp.2020.26.11.1412. J Manag Care Spec Pharm. 2020. PMID: 33119448 Free PMC article.
-
Controlled Substance Prescribing Patterns--Prescription Behavior Surveillance System, Eight States, 2013.MMWR Surveill Summ. 2015 Oct 16;64(9):1-14. doi: 10.15585/mmwr.ss6409a1. MMWR Surveill Summ. 2015. PMID: 26469747
-
Characteristics of New Opioid Use Among Medicare Beneficiaries: Identifying High-Risk Patterns.J Manag Care Spec Pharm. 2019 Sep;25(9):966-972. doi: 10.18553/jmcp.2019.25.9.966. J Manag Care Spec Pharm. 2019. PMID: 31456497 Free PMC article.
-
Impact of Iowa's Prescription Monitoring Program on Opioid Pain Reliever Prescribing Patterns: An Interrupted Time Series Study 2003-2014.Pain Med. 2019 Feb 1;20(2):290-300. doi: 10.1093/pm/pny029. Pain Med. 2019. PMID: 29509935
-
Prescriber Education Interventions to Optimize Opioid Prescribing in Acute Care: A Systematic Review.Pain Physician. 2019 Nov;22(6):E551-E562. Pain Physician. 2019. PMID: 31775401
Cited by
-
Do Postoperative Orthopedic Patients Accurately Report Their Narcotic Medication Usage Using the Interventional Pain Assessment Drugs Scale?Cureus. 2025 Jun 12;17(6):e85852. doi: 10.7759/cureus.85852. eCollection 2025 Jun. Cureus. 2025. PMID: 40656340 Free PMC article.
-
Standardizing research methods for opioid dose comparison: the NIH HEAL morphine milligram equivalent calculator.Pain. 2025 Feb 3;166(8):1729-1737. doi: 10.1097/j.pain.0000000000003529. Pain. 2025. PMID: 39907478
-
Accuracy and validity of reported opioid prescription days' supply.Pharmacoepidemiol Drug Saf. 2022 Dec;31(12):1253-1261. doi: 10.1002/pds.5528. Epub 2022 Aug 30. Pharmacoepidemiol Drug Saf. 2022. PMID: 36053913 Free PMC article.
-
Concordance between controlled substance receipt and post-mortem toxicology in opioid-detected overdose deaths: A statewide analysis.Drug Alcohol Depend. 2023 Mar 1;244:109788. doi: 10.1016/j.drugalcdep.2023.109788. Epub 2023 Jan 30. Drug Alcohol Depend. 2023. PMID: 36738634 Free PMC article.
-
Post-Acute Care Setting After Hip Fracture Hospitalization and Subsequent Opioid Use in Older Adults.J Am Med Dir Assoc. 2023 Jul;24(7):971-977.e4. doi: 10.1016/j.jamda.2023.03.012. Epub 2023 Apr 17. J Am Med Dir Assoc. 2023. PMID: 37080246 Free PMC article.
References
-
- Foley KM. The treatment of cancer pain. N Engl J Med. 1985;313:84–95. - PubMed
-
- Eddy NB, Lee LE. The analgesic equivalence to morphine and relative side action liability of oxymorphone (14-hydroxydihydro morphinone). J Pharmacol Exp Ther. 1959;125:116–121. - PubMed
-
- Fudin J, Raouf M, Wegrzyn EL. Opioid dosing policy: pharmacological considerations regarding equianalgesic dosing. A White Paper from the Academy of Integrative Pain Management. American Academy of Integrative Pain Management; 2017.
-
- Dasgupta N, Kramer ED, Zalman M-A, et al. . Association between non-medical and prescriptive usage of opioids. Drug Alcohol Depend. 2006;82:135–142. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Miscellaneous

