Does loss of spondylolisthesis reduction impact clinical and radiographic outcomes after minimally invasive transforaminal lumbar interbody fusion?
- PMID: 34118417
- PMCID: PMC11980685
- DOI: 10.1016/j.spinee.2021.06.009
Does loss of spondylolisthesis reduction impact clinical and radiographic outcomes after minimally invasive transforaminal lumbar interbody fusion?
Abstract
Background context: Minimally invasive transforaminal lumbar interbody fusion (MI-TLIF) is a common operative approach to address degenerative lumbar stenosis and spondylolisthesis which has failed nonoperative care. Compared to open TLIF, MI-TLIF relies to a greater extent on indirect decompression resulting in a heightened awareness of spondylolisthesis reduction among MI surgeons. To what extent intraoperative reduction is achieved as well as the rate and clinical impact of loss or reduction and slip recurrence remain unknown.
Purpose: To determine the rate and clinical impact of slip recurrence after MI-TLIF with expandable cage technology STUDY DESIGN/SETTING: Retrospective Cohort Study PATIENT SAMPLE: Patients undergoing MI-TLIF for degenerative spondylolisthesis using an articulating, expandable cage OUTCOME MEASURES: Patient-reported outcome measures (PROMs), including the Oswestry Disability Index (ODI), visual analog scale (VAS) for back/leg pain, Short Form-12 (SF-12), and PROMIS Physical Function (PF) METHODS: Patients undergoing MI-TLIF for degenerative spondylolisthesis using articulating, expandable cages from 2017 to 2019 were retrospectively studied. Lateral radiographs were reviewed and evaluated for the presence or absence of spondylolisthesis preoperatively, intraoperatively, and at follow-up times including 2 weeks, 6 weeks, 12 weeks, 6 months, and 1 year postoperatively. Spondylolisthesis was measured from the posterior inferior corner of the cephalad vertebra to the posterior superior corner of the caudal vertebra, with any measurement >1 mm classified as spondylolisthesis, and Meyerding grade was noted. Intraoperative reduction was measured, and loss of reduction was defined as >1 mm increase in spondylolisthesis comparing follow-up imaging to intraoperative films. PROMs were recorded at the preoperative and follow-up time points. Fusion was assessed at 1 year postoperatively via CT.
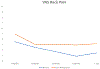
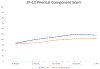
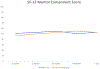
Results: A total of 63 patients and 70 levels were included, with mean age 59.8 years (SD,13.8). 19 levels (27.1%) had complete reduction intraoperatively, 40 (57.1%) had partial reduction, and 11 (15.7%) had no reduction. Of the 30 levels with loss of reduction (50.8%), 20 (66.7%) occurred by 2 weeks postoperatively and 28 (93.3%) occurred by 12 weeks postoperatively. At 6 months, there were significant differences between those who had loss of reduction and those who did not in VAS back pain (3.0 vs. 0.9, p = .017) and SF-12 PCS (41.5 vs. 50.0, p = .035), but no differences were found between the groups for any instruments at any other time points. The overall fusion rate was 82.1% (32/39) at 1 year postoperatively. There was no significant difference in fusion rate between the loss of reduction (16/20) and no loss of reduction (20/23) groups. Patients with loss of reduction had no difference in reoperation rate (1/28) compared to those without loss of reduction (2/24).
Conclusions: While a majority of patients demonstrated reduction intraoperatively, 51% had loss of reduction, most commonly in the acute postoperative period. There were few differences in PROMs between patients who had loss of reduction and those who did not, suggesting that radiographic loss of reduction after MI-TLIF in the setting of degenerative spondylolisthesis may not be clinically meaningful.
Keywords: Degenerative lumbar disease; Interbody fusion; MI-TLIF; Patient-reported outcomes; Prognosis; Risk factors; Spondylolisthesis; TLIF.
Copyright © 2021 Elsevier Inc. All rights reserved.
Figures




References
-
- Jang J-W, Park J-H, Hyun S-J, et al. Clinical Outcomes and Radiologic Changes After Microsurgical Bilateral Decompression by a Unilateral Approach in Patients With Lumbar Spinal Stenosis and Grade I Degenerative Spondylolisthesis With a Minimum 3-Year Follow-Up. Clin spine Surg 2016;29:268–71. - PubMed
-
- Kelleher MO, Timlin M, Persaud O, et al. Success and failure of minimally invasive decompression for focal lumbar spinal stenosis in patients with and without deformity. Spine (Phila Pa 1976) 2010;35:E981–7. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

