Changes in Physicians' Perceptions and Practices on Neonatal Pain Management Over the Past 20 Years. A Survey Conducted at Two Time-Points
- PMID: 34150688
- PMCID: PMC8211759
- DOI: 10.3389/fped.2021.667806
Changes in Physicians' Perceptions and Practices on Neonatal Pain Management Over the Past 20 Years. A Survey Conducted at Two Time-Points
Abstract
Intense research for more than three decades expelled the view that neonates do not experience pain. The aim of this survey was to investigate whether the Greek physicians involved in neonatal intensive care have changed their perceptions regarding neonatal pain, adapting their management practices to the knowledge that have emerged in the past 20-years. This study is a survey conducted at two time-points, 20 years apart. Anonymous questionnaires were distributed to 117 and 145 physicians working in neonatal intensive care units (NICUs) all over Greece in years 2000 and 2019, respectively. The response rate was 90.6 and 80.7% in 2000 and 2019, respectively. All respondents, at both time-points, believed that neonates experience pain, which has serious acute and long-term consequences, while the vast majority considered analgesia-sedation (A-S) during painful interventions as obligatory. Utilization of NICU protocols and pain assessment tools remained low although increased significantly between 2000 and 2019. The use of systemic A-S postoperatively was high at both time-points, while its implementation in infants subjected to prolonged pain, specifically mechanical ventilation, increased significantly by 2019. Systemic or local analgesia for acute procedural pain was used by lower proportions of physicians in 2019, except for the tracheal intubation. In contrast, the use of sweet solutions and non-pharmacological measures prior to or during bedside procedures significantly increased over time. Opioid administration significantly increased, while a shift from morphine to fentanyl was observed. International literature and perinatal-neonatal congresses were stated as the main sources of updating physicians' knowledge and improving management practice on neonatal pain prevention and treatment. In conclusion, Greek NICU-physicians' perceptions that neonates can experience pain with potentially serious acute and long-term consequences remained strong over the past 20 years. Although physicians' practices on neonatal pain management improved, they are still suboptimal, while significant differences exist among centers. Continuing education, globally accepted management protocols, and readily applied pain assessment tools would further improve the management of procedural pain and stress in neonates.
Keywords: analgesics; mechanical ventilation; neonatal pain; non-pharmacological interventions; pain assessment tools; preterm neonates; procedural pain; sedatives.
Copyright © 2021 Agakidou, Tsoni, Stathopoulou, Thomaidou, Farini, Kontou, Karagianni and Sarafidis.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
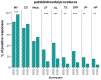

References
LinkOut - more resources
Full Text Sources
Miscellaneous

