Body mass index and severity/fatality from coronavirus disease 2019: A nationwide epidemiological study in Korea
- PMID: 34157043
- PMCID: PMC8219144
- DOI: 10.1371/journal.pone.0253640
Body mass index and severity/fatality from coronavirus disease 2019: A nationwide epidemiological study in Korea
Erratum in
-
Correction: Body mass index and severity/fatality from coronavirus disease 2019: A nationwide epidemiological study in Korea.PLoS One. 2024 Apr 4;19(4):e0301962. doi: 10.1371/journal.pone.0301962. eCollection 2024. PLoS One. 2024. PMID: 38573926 Free PMC article.
Abstract
Objective: Obesity has been reported as a risk factor for severe coronavirus disease 2019 (COVID-19) in recent studies. However, the relationship between body mass index (BMI) and COVID-19 severity and fatality are unclear.
Research design and methods: This study included 4,141 COVID-19 patients who were released from isolation or had died as of April 30, 2020. This nationwide data was provided by the Korean Centers for Disease Control and Prevention Agency. BMI was categorized as follows; < 18.5 kg/m2, 18.5-22.9 kg/m2, 23.0-24.9 kg/m2, 25.0-29.9 kg/m2, and ≥ 30 kg/m2. We defined a fatal illness if the patient had died.
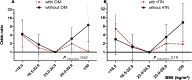
Results: Among participants, those with a BMI of 18.5-22.9 kg/m2 were the most common (42.0%), followed by 25.0-29.9 kg/m2 (24.4%), 23.0-24.9 kg/m2 (24.3%), ≥ 30 kg/m2 (4.7%), and < 18.5 kg/m2 (4.6%). In addition, 1,654 (41.2%) were men and 3.04% were fatalities. Multivariable analysis showed that age, male sex, BMI < 18.5 kg/m2, BMI ≥ 25 kg/m2, diabetes mellitus, chronic kidney disease, cancer, and dementia were independent risk factors for fatal illness. In particular, BMI < 18.5 kg/m2 (odds ratio [OR] 3.97, 95% CI 1.77-8.92), 25.0-29.9 kg/m2 (2.43, 1.32-4.47), and ≥ 30 kg/m2 (4.32, 1.37-13.61) were found to have higher ORs than the BMI of 23.0-24.9 kg/m2 (reference). There was no significant difference between those with a BMI of 18.5-22.9 kg/m2 (1.59, 0.88-2.89) and 23.0-24.9 kg/m2.
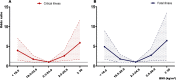
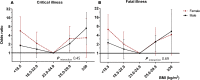
Conclusions: This study demonstrated a non-linear (U-shaped) relationship between BMI and fatal illness. Subjects with a BMI of < 18.5 kg/m2 and those with a BMI ≥ 25 kg/m2 had a high risk of fatal illness. Maintaining a healthy weight is important not only to prevent chronic cardiometabolic diseases, but also to improve the outcome of COVID-19.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
References
-
- Di Angelantonio E, Bhupathiraju SN, Wormser D, Gao P, Kaptoge S, de Gonzalez AB, et al.. Body-mass index and all-cause mortality: individual-participant-data meta-analysis of 239 prospective studies in four continents. The Lancet. 2016;388(10046):776–86. doi: 10.1016/S0140-6736(16)30175-1 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

