Four-Dimensional flow Magnetic Resonance Imaging for Assessment of Pediatric Coarctation of the Aorta
- PMID: 34173693
- PMCID: PMC9084555
- DOI: 10.1002/jmri.27802
Four-Dimensional flow Magnetic Resonance Imaging for Assessment of Pediatric Coarctation of the Aorta
Abstract
Background: Coarctation of the aorta (CoA) typically requires repair, but re-interventions and vascular complications occur, particularly with associated defects like bicuspid aortic valve (BAV). Magnetic resonance imaging (MRI) may identify anatomic and hemodynamic factors contributing to clinical complications.
Purpose: To investigate 4D flow MRI characteristics in pediatric CoA to determine parameters for long-term clinical surveillance.
Study type: Retrospective.
Population: CoA (n = 21), CoA with BAV (n = 24), BAV alone (n = 29), and healthy control (n = 25).
Field strength/sequence: A 1.5 T, 3D CE IR FLASH MRA, 4D flow MRI using 3D time resolved PC-MRI with velocity encoding.
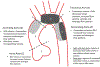
Assessment: Thoracic aorta diameters were measured from 3D CE-MRA. Peak systolic velocities and wall shear stress were calculated and flow patterns were visualized throughout the thoracic aorta using 4D flow. Repair characteristics, re-interventions, and need for anti-hypertensive medications were recorded.
Statistics: Descriptive statistics, ANOVA with post hoc t-testing and Bonferroni correction, Kruskal-Wallis H, intraclass correlation coefficient, Fleiss' kappa.
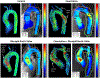
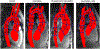
Results: Patients with CoA with or without repair had smaller transverse arch diameters compared to BAV alone and control cohorts (P < 0.05), higher peak systolic flow velocities and wall shear stress compared to controls in the transverse arch and descending aorta (P < 0.05), and flow derangements in the descending aorta. The most common CoA repairs were extended end-to-end anastomosis (n = 22/45, 48.9%, age at repair 1 ± 2 years, seven re-interventions) and stent/interposition graft placement (n = 10/45, 22.2%, age at repair 12 ± 3 years, one re-intervention). Anti-hypertensive medications were prescribed to 33.3% (n = 15/45) of CoA and 34.4% of BAV alone patients (n = 10/29).
Data conclusions: Despite repair, CoA alters hemodynamics and flow patterns in the transverse arch and descending aorta. These findings may contribute to vascular remodeling and secondary complications. 4D flow MRI may be valuable in risk stratification, treatment selection and postintervention assessment. Long-term, prospective studies are warranted to correlate patient and MRI factors with clinical outcomes.
Evidence level: 3 TECHNICAL EFFICACY: Stage 3.
Keywords: 4D flow; cardiac; coarctation of the aorta; congenital heart disease; pediatrics.
© 2021 International Society for Magnetic Resonance in Medicine.
Figures
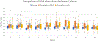
Similar articles
-
4D flow MRI, cardiac function, and T1 -mapping: Association of valve-mediated changes in aortic hemodynamics with left ventricular remodeling.J Magn Reson Imaging. 2018 Jul;48(1):121-131. doi: 10.1002/jmri.25916. Epub 2017 Dec 5. J Magn Reson Imaging. 2018. PMID: 29206322 Free PMC article.
-
Altered 4-D magnetic resonance imaging flow characteristics in complex congenital aortic arch repair.Pediatr Radiol. 2020 Jan;50(1):17-27. doi: 10.1007/s00247-019-04507-0. Epub 2019 Aug 31. Pediatr Radiol. 2020. PMID: 31473788 Free PMC article.
-
Aortic hemodynamics in patients with and without repair of aortic coarctation: in vivo analysis by 4D flow-sensitive magnetic resonance imaging.Invest Radiol. 2011 May;46(5):317-25. doi: 10.1097/RLI.0b013e3182034fc2. Invest Radiol. 2011. PMID: 21285892
-
Multimodality imaging in bicuspid aortic valve.Prog Cardiovasc Dis. 2020 Jul-Aug;63(4):442-451. doi: 10.1016/j.pcad.2020.06.003. Epub 2020 Jun 9. Prog Cardiovasc Dis. 2020. PMID: 32531300 Review.
-
Utility of 4D Flow MRI in Thoracic Aortic Diseases: A Literature Review of Clinical Applications and Current Evidence.Magn Reson Med Sci. 2022 Mar 1;21(2):327-339. doi: 10.2463/mrms.rev.2021-0046. Epub 2021 Sep 8. Magn Reson Med Sci. 2022. PMID: 34497166 Free PMC article. Review.
Cited by
-
Going with the flow: Implementing a 4D flow MRI program at a children's hospital.Pediatr Radiol. 2024 Nov 14. doi: 10.1007/s00247-024-06093-2. Online ahead of print. Pediatr Radiol. 2024. PMID: 39540925 Review.
-
Coarctation Balloon Angioplasty in a Rare Case with Congenitally Corrected Transposition of the Great Arteries and Ebstein's Anomaly.J Tehran Heart Cent. 2024 Apr;19(2):132-135. doi: 10.18502/jthc.v19i2.16203. J Tehran Heart Cent. 2024. PMID: 40322770 Free PMC article.
-
Intraventricular haemodynamic changes caused by increased left ventricular afterload in re-coarctation of aorta: a case report.Eur Heart J Case Rep. 2023 Oct 16;7(11):ytad514. doi: 10.1093/ehjcr/ytad514. eCollection 2023 Nov. Eur Heart J Case Rep. 2023. PMID: 37942351 Free PMC article.
-
Enhanced 4D Flow MRI-Based CFD with Adaptive Mesh Refinement for Flow Dynamics Assessment in Coarctation of the Aorta.Ann Biomed Eng. 2022 Aug;50(8):1001-1016. doi: 10.1007/s10439-022-02980-7. Epub 2022 May 27. Ann Biomed Eng. 2022. PMID: 35624334 Free PMC article.
-
Comparison of 2D and 4D Flow MRI in Neonates Without General Anesthesia.J Magn Reson Imaging. 2023 Jan;57(1):71-82. doi: 10.1002/jmri.28303. Epub 2022 Jun 21. J Magn Reson Imaging. 2023. PMID: 35726779 Free PMC article.
References
-
- Niaz T, Poterucha JT, Johnson JN, et al. Incidence, morphology, and progression of bicuspid aortic valve in pediatric and young adult subjects with coexisting congenital heart defects. Congenit Heart Dis 2017;129:261–269. - PubMed
-
- Sugimoto A, Ota N, Miyakoshi C, et al. Mid to long-term aortic valve related outcomes after conventional repair for patients with interrupted aortic arch or coarctation of the aorta combined with ventricular septal defect: The impact of bicuspid aortic valve. Eur J Cardiothorac Surg 2014;46:952–960. - PubMed
-
- Connolly HM, Huston J, Brown RD Jr, Warnes CA, Ammash NM, Tajik AJ. Intracranial aneurysms in patients with coarctation of the aorta: A prospective magnetic resonance angiography study of 100 patients. Mayo Clin Proc 2003;78:1491–1499. - PubMed
-
- Brown ML, Burkhart HM, Connolly HM, et al. Coarctation of the aorta: Lifelong surveillance is mandatory following surgical repair. J Am Coll Cardiol 2013;10(62):1020–1025. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

