Nasal High Flow at 25 L/min or Expiratory Resistive Load Do Not Improve Regional Lung Function in Patients With COPD: A Functional CT Imaging Study
- PMID: 34177626
- PMCID: PMC8222991
- DOI: 10.3389/fphys.2021.683316
Nasal High Flow at 25 L/min or Expiratory Resistive Load Do Not Improve Regional Lung Function in Patients With COPD: A Functional CT Imaging Study
Abstract
Background: Nasal high flow (NHF) is a non-invasive breathing therapy that is based on the delivery via a large-caliber nasal cannula of heated and humidified air at flow rates that exceed peak inspiratory flow. It is thought that positive airway pressure generated by NHF can help reduce gas trapping and improve regional lung ventilation. There are no data to confirm this hypothesis at flow rates applicable in stable chronic obstructive pulmonary disease (COPD) patients.
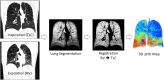
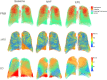
Methods: In this study, we used non-rigid registration of computed tomography (CT) images acquired at maximal expiration and inspiration to compute regional lung attenuation changes (ΔHU), and lung displacement (LD), indices of regional lung ventilation. Parametric response maps (Galban et al., 2012) were also computed in each experimental condition. Eight COPD patients were assessed at baseline (BL) and after 5 min of NHF and expiratory resistive loading (ERL).
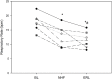
Results: ΔHU was: BL (median, IQR): 85 (67.2, 102.8); NHF: 90.7 (57.4, 97.6); ERL: 74.6 (46.4, 89.6) HU (p = 0.531); and LD: 27.8 (22.3, 39.3); 17.6 (15.4, 27.9); and 20.4 (16.6, 23.6) mm (p = 0.120) in the 3 conditions, respectively. No significant difference in trapping was observed. Respiratory rate significantly decreased with both treatments [BL: 17.3 (16.4, 18.9); NHF: 13.7; ERL: 11.4 (9.6, 13.2) bpm; and p < 0.001].
Conclusion: Neither NHF at 25 L/min nor ERL significantly improved the regional lung ventilation of stable COPD patients with gas trapping, based on functional lung CT imaging. Further study including more subjects is needed to assess the potential effect of NHF on regional lung function at higher flow rates.
Clinical trial registration: www.clinicaltrials.gov/under, identifier NCT03821311.
Keywords: COPD; computed tomography; expiratory resistive loading; image processing; nasal high flow cannula.
Copyright © 2021 Cohen, Broche, Machichi, Ferretti, Tamisier, Pépin and Bayat.
Conflict of interest statement
J-LP has received grants and research funds for other studies from: Air Liquide Foundation, Agiradom, AstraZeneca, Fisher & Paykel, Mutualia, Philips, Resmed, Vitalaire, Boehringer Ingelheim, Jazz Pharmaceuticals, Night Balance, and Sefam. SB received funding from Fisher & Paykel for this study. The funder was involved in the study design, but not the collection, analysis, interpretation of data, the writing of this article, or the decision to submit it for publication. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Modelling nasal high flow therapy effects on upper airway resistance and resistive work of breathing.Respir Physiol Neurobiol. 2018 Aug;254:23-29. doi: 10.1016/j.resp.2018.03.014. Epub 2018 Apr 7. Respir Physiol Neurobiol. 2018. PMID: 29635072
-
Nasal highflow improves ventilation in patients with COPD.Int J Chron Obstruct Pulmon Dis. 2016 May 25;11:1077-85. doi: 10.2147/COPD.S104616. eCollection 2016. Int J Chron Obstruct Pulmon Dis. 2016. PMID: 27307723 Free PMC article. Clinical Trial.
-
Effect of respiratory rate and size of cannula on pressure and dead-space clearance during nasal high flow in patients with COPD and acute respiratory failure.J Appl Physiol (1985). 2022 Feb 1;132(2):553-563. doi: 10.1152/japplphysiol.00769.2021. Epub 2022 Jan 27. J Appl Physiol (1985). 2022. PMID: 35085029 Free PMC article.
-
Nasal High Flow for Stable Patients with Chronic Obstructive Pulmonary Disease: A Systematic Review and Meta-Analysis.COPD. 2019 Dec;16(5-6):368-377. doi: 10.1080/15412555.2019.1672637. Epub 2019 Oct 27. COPD. 2019. PMID: 31656111
-
[Nasal Highflow (NHF): A New Therapeutic Option for the Treatment of Respiratory Failure].Pneumologie. 2016 Jan;70(1):49-54. doi: 10.1055/s-0041-110286. Epub 2016 Jan 20. Pneumologie. 2016. PMID: 26789432 Review. German.
References
-
- Adams R., Bischof L. (1994). Seeded region growing. IEEE Transact. 16 641–647.
-
- Ashraf-Kashani N., Kumar R. (2017). High-flow nasal oxygen therapy. BJA Educat. 17 63–67.
-
- Chanques G., Riboulet F., Molinari N., Carr J., Jung B., Prades A., et al. (2013). Comparison of three high flow oxygen therapy delivery devices: a clinical physiological cross-over study. Min. Anestesiol. 79 1344–1355. - PubMed
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials

