The Influences of TSH Stimulation Level, Stimulated Tg Level and Tg/TSH Ratio on the Therapeutic Effect of 131I Treatment in DTC Patients
- PMID: 34177793
- PMCID: PMC8232882
- DOI: 10.3389/fendo.2021.601960
The Influences of TSH Stimulation Level, Stimulated Tg Level and Tg/TSH Ratio on the Therapeutic Effect of 131I Treatment in DTC Patients
Abstract
Purpose: To study the influences of pre-ablation TSH stimulation level, sTg and sTg/TSH ratio on the therapeutic effect of the first 131I treatment in DTCs.
Methods: According to the thyroid stimulating hormone (TSH) levels (mU/l), all the 479 differentiated thyroid cancer (DTC) patients were divided into two groups: TSH < 30 and TSH ≥ 30. The TSH ≥ 30 group was divided into three subgroups: 30 ≤ TSH < 60, 60 ≤ TSH < 90 and TSH ≥ 90. The clinical features and the therapeutic effects of the first 131I treatment were analyzed. The cutoffs of stimulated thyroglobulin (sTg) and sTg/TSH ratio were calculated to predict the therapeutic effect of 131I treatment.
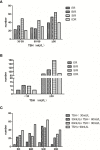
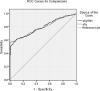
Results: Among the three subgroups, the TSH ≥ 90 subgroup was younger and less likely to be associated with cervical lymph node metastasis (LNM). The postoperative levothyroxine (L-T4) dose in the 60 ≤ TSH < 90 subgroup was the lowest. Between the two groups, patients in the TSH < 30 group had higher postoperative L-T4 dose and longer thyroid hormone withdrawal (THW) time. The excellent response rates six months after the first 131I treatment among the three subgroups and between the two groups were not of statistical significance. The distribution of different TSH stimulation levels among each response group was similar. The cutoffs for the better therapeutic effect of the first 131I treatment in sTg and sTg/TSH were < 9.51 ng/ml and < 0.11, respectively. Both univariate and multivariate logistic regressions showed that cervical LNM, distant metastasis, higher sTg and higher sTg/TSH ratio predicted poorer therapeutic effect.
Conclusions: There was no significant influence of TSH stimulation levels before the first 131I treatment on the therapeutic effect of DTC. The sTg/TSH ratio can be considered as another predictor of 131I therapeutic effect.
Keywords: 131I treatment; TSH stimulation level; differentiated thyroid cancer; sTg; sTg/TSH ratio; therapeutic effect.
Copyright © 2021 Zheng, Rui, Wang, Li, Tan and Liu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Stimulating thyroglobulin to TSH ratio predict long-term efficacy of 131I therapy in patients with differentiated thyroid cancer after total thyroidectomy: a retrospective study.Endocrine. 2024 Jun;84(3):1064-1071. doi: 10.1007/s12020-023-03663-6. Epub 2024 Jan 3. Endocrine. 2024. PMID: 38172344
-
Thyroglobulin levels and thyroglobulin/thyrotropin ratio could predict the success of the ablative/therapeutic 131I in the differentiated thyroid cancers.Endocr Res. 2017 Feb;42(1):42-48. doi: 10.3109/07435800.2016.1173056. Epub 2016 May 4. Endocr Res. 2017. PMID: 27144920
-
Clinical Role of Pre-ablation Stimulated Thyroglobulin and Thyroid-Stimulating Hormone Ratio for Radioactive Iodine Treatment in Adults with Papillary Thyroid Cancer.Clin Oncol (R Coll Radiol). 2025 May;41:103797. doi: 10.1016/j.clon.2025.103797. Epub 2025 Mar 6. Clin Oncol (R Coll Radiol). 2025. PMID: 40147171
-
Follow-up of differentiated thyroid carcinoma.Minerva Endocrinol. 2004 Dec;29(4):161-74. Minerva Endocrinol. 2004. PMID: 15765026 Review. English, Italian.
-
Recombinant human thyrotropin-aided versus thyroid hormone withdrawal-aided radioiodine treatment for differentiated thyroid cancer after total thyroidectomy: a meta-analysis.Radiother Oncol. 2014 Jan;110(1):25-30. doi: 10.1016/j.radonc.2013.12.018. Epub 2014 Jan 28. Radiother Oncol. 2014. PMID: 24485353 Review.
Cited by
-
Comparing the efficacy of thyroglobulin and thyroglobulin/ thyroid-stimulating hormone ratio models in predicting a successful response to radioactive iodine therapy.BMC Endocr Disord. 2023 Jan 20;23(1):19. doi: 10.1186/s12902-022-01261-7. BMC Endocr Disord. 2023. PMID: 36670396 Free PMC article.
-
[Insufficient elevation of TSH before therapy with I131 in a patient with metastatic differentiated thyroid carcinoma].Rev Fac Cien Med Univ Nac Cordoba. 2023 Jun 30;80(2):149-152. doi: 10.31053/1853.0605.v80.n2.38112. Rev Fac Cien Med Univ Nac Cordoba. 2023. PMID: 37402303 Free PMC article. Spanish.
-
Combination of Stimulated Thyroglobulin and Antithyroglobulin Antibody Predicts the Efficacy and Prognosis of 131I Therapy in Patients With Differentiated Thyroid Cancer Following Total Thyroidectomy: A Retrospective Study.Front Endocrinol (Lausanne). 2022 Apr 6;13:857057. doi: 10.3389/fendo.2022.857057. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 35464061 Free PMC article.
-
Higher adjuvant radioactive iodine therapy dosage helps intermediate-risk papillary thyroid carcinoma patients achieve better therapeutic effect.Front Endocrinol (Lausanne). 2024 Jan 17;14:1307325. doi: 10.3389/fendo.2023.1307325. eCollection 2023. Front Endocrinol (Lausanne). 2024. PMID: 38298190 Free PMC article.
-
Analysis of factors influencing the clinical outcome after surgery and 131I therapy in patients with moderate-risk thyroid papillary carcinoma.Front Endocrinol (Lausanne). 2022 Oct 14;13:1015798. doi: 10.3389/fendo.2022.1015798. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 36313750 Free PMC article.
References
-
- Haugen BR, Alexander EK, Bible KC, Doherty GM, Mandel SJ, Nikiforov YE, et al. . 2015 American Thyroid Association Management Guidelines for Adult Patients With Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid (2016) 26(1):1–133. 10.1089/thy.2015.0020 - DOI - PMC - PubMed
-
- Lawal IO, Nyakale NE, Harry LM, Lengana T, Mokgoro NP, Vorster M, et al. . Higher Preablative Serum Thyroid-Stimulating Hormone Level Predicts Radioiodine Ablation Effectiveness in Patients With Differentiated Thyroid Carcinoma. Nucl Med Commun (2017) 38(3):222–7. 10.1097/MNM.0000000000000640 - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

