Association between epidural analgesia and indications for intrapartum caesarean delivery in group 1 of the 10-group classification system at a tertiary maternity hospital, Shanghai, China: a retrospective cohort study
- PMID: 34187400
- PMCID: PMC8243735
- DOI: 10.1186/s12884-021-03925-z
Association between epidural analgesia and indications for intrapartum caesarean delivery in group 1 of the 10-group classification system at a tertiary maternity hospital, Shanghai, China: a retrospective cohort study
Abstract
Background: In this study, we aimed to determine whether epidural analgesia affects the indications for intrapartum caesarean delivery, such as foetal distress, dystocia, or maternal request, in nulliparous term women with spontaneous labour (Group 1 in the 10-Group Classification System).
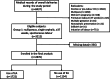
Methods: We conducted a retrospective cohort study and collected data from the electronic medical records of deliveries performed in our institution between 1 January 2017 and 30 June 2017. Women conforming to the criterion of Group 1 according to the 10-Group Classification System were enrolled. We compared labour outcomes between women with and without epidural analgesia and analysed the association between epidural analgesia and indications for caesarean by using multivariate logistic regression analysis.
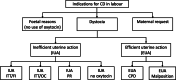
Results: A total of 3212 women met the inclusion criteria, and 2876 were enrolled in the final analyses. Women who received epidural analgesia had a significantly lower intrapartum caesarean delivery rate (16.0% vs. 26.7%, P < 0.001), higher rates of amniotomy (53.4% vs. 42.3%, P < 0.001) and oxytocin augmentation (79.5% vs. 67.0%, P < 0.001), and a higher incidence of intrapartum fever (≥38 °C) (23.3% vs. 8.5%, P < 0.001) than those who did not receive epidural analgesia. There were no significant differences between the groups for most indications, except a lower probability of maternal request for caesarean delivery (3.9% vs. 10.5%, P < 0.001) observed in women who received epidural analgesia than in those who did not. Epidural analgesia was revealed to be associated with a decreased risk of maternal request for caesarean delivery (adjusted odds ratio [aOR], 0.30; 95% confidence interval [CI], 0.22-0.42; P < 0.001); however, oxytocin augmentation was related to an increased risk of maternal request (aOR, 2.34; 95%CI, 1.47-3.75; P < 0.001). Regarding the reasons for the maternal request for caesarean delivery, significantly fewer women complained of pain (0.5% vs. 4.6%, P < 0.001) or had no labour progress (1.3% vs. 3.6%, P < 0.001) among those who received analgesia.
Conclusions: Among the women in Group 1, epidural analgesia was associated with a lower intrapartum caesarean delivery rate, which may be explained by a reduction in the risk of maternal request for an intrapartum caesarean delivery.
Keywords: Caesarean delivery; Epidural anaesthesia; Intrapartum; Labour pain; Nulliparous women.
Conflict of interest statement
The authors report no conflicts of interest.
Figures
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

