Role of Photobiomodulation Therapy in Modulating Oxidative Stress in Temporomandibular Disorders. A Systematic Review and Meta-Analysis of Human Randomised Controlled Trials
- PMID: 34202292
- PMCID: PMC8300797
- DOI: 10.3390/antiox10071028
Role of Photobiomodulation Therapy in Modulating Oxidative Stress in Temporomandibular Disorders. A Systematic Review and Meta-Analysis of Human Randomised Controlled Trials
Abstract
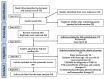
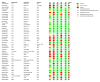
This systematic review and meta-analysis (PROSPERO registration; ref CRD 42020198921) aimed to govern photobiomodulation therapy (PBMT) efficacy in temporomandibular disorder (TMD). PRISMA guidelines and Cochrane Collaboration recommendations were followed. Differences in pain reduction assessment by qualitative measurement with visual analogue scale pain (VAS), pressure threshold (PPT) and maximum mouth opening (MMO) were calculated with 95% confidence intervals and pooled in a random effects model with a subgroup analysis, evaluating the role of follow-up duration. Heterogeneity was analysed using Q and I2 tests. Publication bias was assessed by visual examination of funnel plot symmetry. Qualitative analysis revealed 46% of the 44 included studies showed a high risk of bias. Meta-analysis on 32 out of 44 studies revealed statistically significant intergroup differences (SSID) for VAS (SMD = -0.55; 95% CI = -0.82 to -0.27; Z = 3.90 (p < 0.001)), PPT (SMD = -0.45; 95% CI = -0.89 to 0.00; Z = 1.97 (p = 0.05)) and MMO (SMD = -0.45; 95% CI = -0.89 to 0.00; Z = 1.97 (p = 0.05)), favouring PBMT compared to control treatment strategies. Sensitivity analysis revealed SSID (SMD = -0.53; 95% CI = -0.73 to -0.32; Z = 5.02 (p < 0.0001)) with low heterogeneity (Τ2 = 0.02; χ2 = 16.03 (p = 0.31); I2 = 13%). Hence, this review, for first time, proposed suggested recommendations for PBMT protocols and methodology for future extensive TMD research.
Keywords: TMD standard care; light-emitting diodes; low-level laser therapy; orofacial pain; oxidative stress; photobiomodulation; randomised controlled trials; reactive oxygen species; synovial joint proinflammatory mediators; temporomandibular joint disorder.
Conflict of interest statement
The authors declare no conflict of interest.
Figures











References
-
- De La Torre Canales G., Câmara-Souza M.B., Muñoz Lora V.R.M., Guarda-Nardini L., Conti P.C.R., Rodrigues Garcia R.M., Del Bel Cury A.A., Manfredini D. Prevalence of psychosocial impairment in temporomandibular disorder patients: A systematic review. J. Oral Rehabil. 2018;45:881–889. doi: 10.1111/joor.12685. - DOI - PubMed
-
- Benoliel R., Svensson P., Evers S., Wang S.J., Barke A., Korwisi B., Rief W., Treede R.D. IASP Taskforce for the Classification of Chronic Pain. The IASP classification of chronic pain for ICD-11: Chronic secondary headache or orofacial pain. Pain. 2019;160:60–68. doi: 10.1097/j.pain.0000000000001435. - DOI - PubMed
-
- Sessle B.J. The neural basis of temporomandibular joint and masticatory muscle pain. J. Orofac. Pain. 1999;13:238–245. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

