Gastric Emptying Time and Volume of the Small Intestine as Objective Markers in Patients With Symptoms of Diabetic Enteropathy
- PMID: 34210904
- PMCID: PMC8266501
- DOI: 10.5056/jnm19195
Gastric Emptying Time and Volume of the Small Intestine as Objective Markers in Patients With Symptoms of Diabetic Enteropathy
Abstract
Background/aims: Patients with diabetes mellitus (DM) often suffer from gastrointestinal (GI) symptoms, but these correlate poorly to established objective GI motility measures. Our aim is to perform a detailed evaluation of potential measures of gastric and small intestinal motility in patients with DM type 1 and severe GI symptoms.
Methods: Twenty patients with DM and 20 healthy controls (HCs) were included. GI motility was examined with a 3-dimensional-Transit capsule, while organ volumes were determined by CT scans.
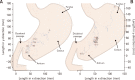
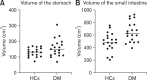
Results: Patients with DM and HCs did not differ with regard to median gastric contraction frequency (DM: 3.0 contractions/minute [interquartile range {IQR}, 2.9-3.0]; HCs: 2.9 [IQR, 2.8-3.1]; P = 0.725), amplitude of gastric contractions (DM: 9 mm [IQR, 8-11]; HCs: 11 mm (IQR, 9-12); P = 0.151) or fasting volume of the stomach wall (DM: 149 cm3 [IQR, 112-187]; HCs: 132 cm3 [IQR, 107-154]; P = 0.121). Median gastric emptying time was prolonged in patients (DM: 3.3 hours [IQR, 2.6-4.6]; HCs: 2.4 hours [IQR, 1.8-2.7]; P = 0.002). No difference was found in small intestinal transit time (DM: 5 hours [IQR, 3.7-5.6]; HCs: 4.8 hours [IQR, 3.9-6.0]; P = 0.883). However, patients with DM had significantly larger volume of the small intestinal wall (DM: 623 cm3 [IQR, 487-766]; HCs: 478 cm3 [IQR, 393-589]; P = 0.003). Among patients, 13 (68%) had small intestinal wall volume and 9 (50%) had gastric emptying time above the upper 95% percentile of HCs.
Conclusion: In our study, gastric emptying time and volume of the small intestinal wall appeared to be the best objective measures in patients with DM type 1 and symptoms and gastroenteropathy.
Keywords: Diabetes mellitus; Diabetic neuropathies; Gastric emptying; Gastrointestinal motility; Organ size.
Conflict of interest statement
Figures
Similar articles
-
Panenteric Transit Times and Contractile Activity in Diabetic Gastroenteropathy.J Neurogastroenterol Motil. 2025 Apr 30;31(2):241-255. doi: 10.5056/jnm24126. J Neurogastroenterol Motil. 2025. PMID: 40205900 Free PMC article.
-
Colonic motility in patients with type 1 diabetes and gastrointestinal symptoms.Neurogastroenterol Motil. 2020 Dec;32(12):e13948. doi: 10.1111/nmo.13948. Epub 2020 Jul 20. Neurogastroenterol Motil. 2020. PMID: 32688448
-
Gastric electrical stimulation: an evidence-based analysis.Ont Health Technol Assess Ser. 2006;6(16):1-79. Epub 2006 Aug 1. Ont Health Technol Assess Ser. 2006. PMID: 23074486 Free PMC article.
-
Central nervous system action of peptides to influence gastrointestinal motor function.Gastroenterology. 1990 Feb;98(2):517-28. doi: 10.1016/0016-5085(90)90849-v. Gastroenterology. 1990. PMID: 2104814 Review.
-
Gastrointestinal motility disorders in patients with diabetes mellitus.J Intern Med. 1995 Apr;237(4):403-9. doi: 10.1111/j.1365-2796.1995.tb01194.x. J Intern Med. 1995. PMID: 7714464 Review.
Cited by
-
Gut region-specific TNFR expression: TNFR2 is more affected than TNFR1 in duodenal myenteric ganglia of diabetic rats.World J Diabetes. 2023 Jan 15;14(1):48-61. doi: 10.4239/wjd.v14.i1.48. World J Diabetes. 2023. PMID: 36684383 Free PMC article.
-
Gut Region-Specific Interleukin 1β Induction in Different Myenteric Neuronal Subpopulations of Type 1 Diabetic Rats.Int J Mol Sci. 2023 Mar 18;24(6):5804. doi: 10.3390/ijms24065804. Int J Mol Sci. 2023. PMID: 36982878 Free PMC article.
-
Panenteric Transit Times and Contractile Activity in Diabetic Gastroenteropathy.J Neurogastroenterol Motil. 2025 Apr 30;31(2):241-255. doi: 10.5056/jnm24126. J Neurogastroenterol Motil. 2025. PMID: 40205900 Free PMC article.
-
Apoptosis and Oxidative Stress in Human Intestinal Epithelial Caco-2 Cells Caused by Marine Phycotoxin Azaspiracid-2.Toxins (Basel). 2024 Aug 31;16(9):381. doi: 10.3390/toxins16090381. Toxins (Basel). 2024. PMID: 39330839 Free PMC article.
-
MRI-Based Quantification of Pan-Alimentary Function and Motility in Subjects with Diabetes and Gastrointestinal Symptoms.J Clin Med. 2023 Sep 14;12(18):5968. doi: 10.3390/jcm12185968. J Clin Med. 2023. PMID: 37762909 Free PMC article.
References
-
- Clouse RE, Lustman PJ. Gastrointestinal symptoms in diabetic patients: lack of association with neuropathy. Am J Gastroenterol. 1989;84:868–872. - PubMed
LinkOut - more resources
Full Text Sources

